Study on predictive value of shock index in postpartum hemorrhage blood transfusion treatment and ICU admission
-
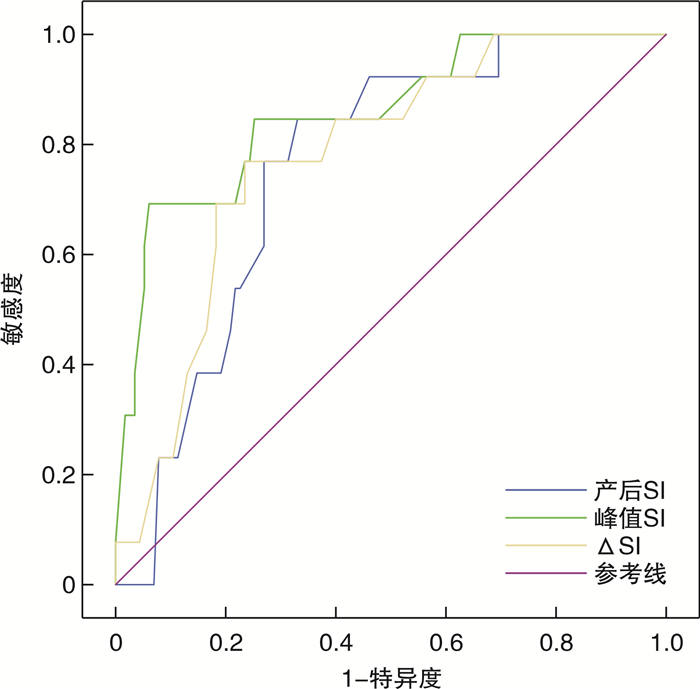
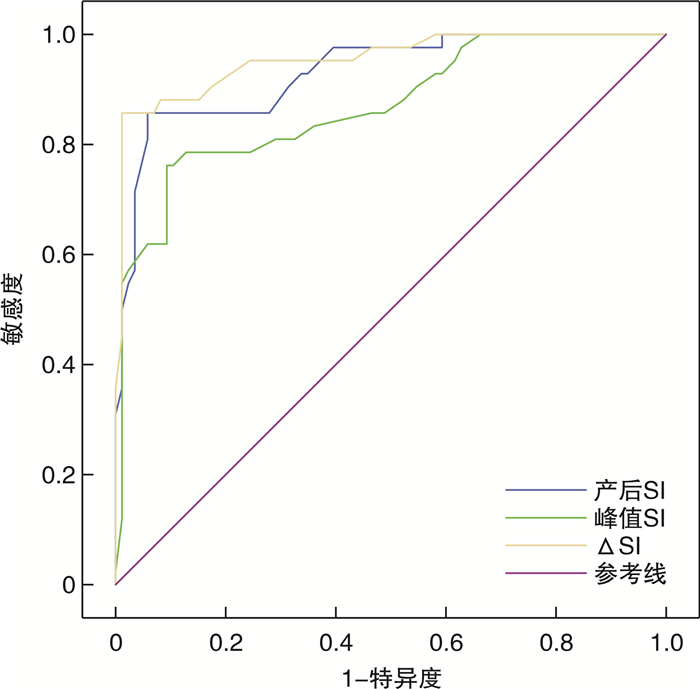
摘要: 目的 分析不同阶段休克指数(SI)对产后出血(PPH)输血治疗和入住ICU的预测价值。方法 选取PPH产妇128例,根据生产时有无输血分为输血组(42例)和未输血组(86例),收集所有产妇年龄、身高、体重、并发症、产前血常规、血压、24 h失血量、住院天数和是否入住ICU,并对以上资料进行统计分析。结果 输血组和未输血组是否前置胎盘、是否人工剥离胎盘、产前血红蛋白、产前血细胞比容、24 h失血量、产后心率、产后血压、产后SI>1、峰值SI、△SI、住院天数、是否入住ICU等比较,差异均有统计学意义(均P< 0.05)。前置胎盘、人工剥离胎盘、产前Hb、失血量、产后SI>1均为PPH输血治疗的独立影响因素。产后SI、峰值SI、△SI(峰值SI-产前SI)预测PPH输血治疗的曲线下面积(AUC)分别为0.931、0.869、0.955,且3种方法预测AUC两两比较差异有统计学意义(均P< 0.05)。产后SI、峰值SI、△SI预测产后入住ICU的AUC分别为0.758、0.857、0.770,且峰值SI预测AUC高于产后SI和△SI,差异有统计学意义(均P< 0.05)。结论 产后SI>1为PPH输血治疗的独立影响因素,△SI对PPH输血预测价值优于产后SI和峰值SI,峰值SI对入住ICU治疗预测价值优于产后SI和△SI。Abstract: Objective To analyze the predictive value of shock index(SI) in different stages of postpartum hemorrhage(PPH) blood transfusion treatment and ICU admission.Methods A total of 128 cases of PPH puerpera in our hospital were selected and divided into postpartum blood transfusion group(42 cases) and non blood transfusion group(86 cases) according to postpartum blood transfusion. The age, height, weight, complications, prenatal blood routine, blood pressure, 24 h blood loss, length of hospital stay and ICU stay of all puerpera were collected, and the above data were statistically analyzed.Results There were significant differences in placenta previa, artificial exfoliation, prenatal Hb, HCT, 24 h blood loss, postpartum HR, postpartum blood pressure, postpartum SI>1, peak SI, △ SI, length of hospital stay and ICU stay between the postpartum blood transfusion group and non blood transfusion group(allP< 0.05). Placenta previa, artificial exfoliated placenta, prenatal Hb, blood loss and postpartum SI>1 were all independent influencing factors of PPH blood transfusion. The area under the curve(AUC) of postpartum SI, peak SI and △SI in predicting PPH blood transfusion treatment were 0.931, 0.869 and 0.955 respectively, and there were significant differences between the three methods in predicting AUC(allP< 0.05).Conclusion Postpartum SI>1 is an independent influencing factor of PPH blood transfusion. The predictive value of △SI is better than postpartum SI and peak SI, and the predictive value of peak SI in ICU treatment is better than postpartum SI and △SI.
-
Key words:
- shock index /
- postpartum hemorrhage /
- forecast value /
- placenta previa /
- scar uterus
-

-
表 1 不同组别临床资料比较
例,X±S 临床资料 产后输血组(n=42) 未输血组(n=86) t(χ2) P 年龄/岁 31.27±4.65 30.56±4.72 0.803 0.423 BMI/(kg·m-2) 27.55±3.27 28.01±4.01 0.645 0.520 初产妇/经产妇 25/17 57/29 0.559 0.455 单胎/多胎 36/6 82/4 3.637 0.057 妊娠期高血压(是/否) 2/40 2/84 0.553 0.457 妊娠期糖尿病(是/否) 5/37 7/79 0.471 0.493 前置胎盘(是/否) 9/33 2/84 13.109 < 0.001 瘢痕子宫(是/否) 4/38 1/85 3.264 0.071 绒毛膜羊膜炎(是/否) 2/40 1/85 0.412 0.521 人工剥离胎盘(是/否) 17/25 9/77 15.702 0.000 婴儿体重/g 3021.62±375.22 3044.57±421.17 0.300 0.765 产前Hb/(g·L-1) 102.54±12.32 114.33±14.11 4.621 < 0.001 产前Hct/% 32.56±3.54 34.67±4.11 2.849 0.005 产前HR/bpm 77.56±8.51 75.00±7.63 1.716 0.089 产前SBP/mmHg 113.12±16.56 112.10±14.33 0.387 0.720 产前DBP/mmHg 69.57±9.54 70.33±8.33 0.462 0.645 产前SI 0.68±0.12 0.67±0.10 0.497 0.620 孕周 37.56±2.16 38.55±3.79 1.571 0.118 24 h失血量/mL 1752.32±312.11 920.58±217.54 17.516 < 0.001 产后HR/bpm 114.70±10.52 86.59±7.33 17.561 < 0.001 产后SBP/mmHg 98.55±6.59 110.32±9.33 7.325 < 0.001 产后DBP/mmHg 62.57±8.47 67.87±9.32 3.110 < 0.001 产后SI>1(是/否) 36/6 4/82 86.310 < 0.001 峰值SI 1.11±0.25 0.82±0.13 8.647 < 0.001 △SI 0.44±0.16 0.16±0.11 11.582 < 0.001 产后住院天数 5.52±1.24 4.57±1.33 3.877 < 0.001 产后入住ICU(是/否) 12/30 1/76 20.773 < 0.001 表 2 PPH输血治疗的二元logistic回归分析
变量 B Wald P OR 95%CI 前置胎盘 1.855 10.435 < 0.001 6.389 2.074~19.683 人工剥离胎盘 0.709 15.739 0.021 2.032 1.431~2.884 产前Hb -0.112 21.082 0.036 0.894 0.852~0.938 失血量 0.612 6.126 0.013 1.844 1.136~2.985 产后SI>1 1.946 10.799 < 0.001 7.000 2.193~22.343 表 3 不同SI对PPH输注治疗预测价值比较
检测方法 面积差异 z P ΔSI vs产后SI 0.024 1.986 0.048 ΔSI vs峰值SI 0.086 2.952 0.012 产后SI vs峰值SI 0.062 2.247 0.024 表 4 不同SI对PPH入住ICU预测价值比较
检测方法 面积差异 z P ΔSI vs产后SI 0.012 1.321 0.154 ΔSI vs峰值SI 0.078 2.724 0.018 产后SI vs峰值SI 0.099 3.544 < 0.001 -
[1] 黄颖. 红细胞血浆联合冷沉淀输注用于产后大出血疗效观察[J]. 临床血液学杂志, 2020, 33(12): 844-847. http://lcxz.cbpt.cnki.net/WKC/WebPublication/paperDigest.aspx?paperID=9053cd8d-dc07-49d1-aa3b-fac0cbb3fb0c
[2] Higgins N, Patel SK, Toledo P. Postpartum hemorrhage revisited: new challenges and solutions[J]. Curr Opin Anaesthesiol, 2019, 32(3): 278-284. doi: 10.1097/ACO.0000000000000717
[3] 朱方玉, 漆洪波. ACOG实践简报"产后出血(2017版)"解读[J]. 中国实用妇科与产科杂志, 2018, 34(6): 623-627. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGSF201806013.htm
[4] Tanacan A, Yalcin A, Unal C, et al. Fatal Postpartum Hemorrhage in a Patient with Niemann-Pick Disease Type B[J]. Case Rep Obstet Gynecol, 2018, 2018: 9719374.
[5] Hcini N, Mchirgui A, Pomar L, et al. Early Prediction of Blood Loss and Postpartum Hemorrhage after Vaginal Delivery by Ultrasound Measurement of Intrauterine Content[J]. Ultrasound Med Biol, 2020, 46(11): 3145-3153. doi: 10.1016/j.ultrasmedbio.2020.07.017
[6] 中国妇幼保健协会放射介入专业委员会, 中国医师协会微无创专业委员会手术安全委员会及质量控制专委会, 中国医师协会微无创专业委员会妇产科出血性疾病全程管理专委会. 血管内介入技术在产后出血防治中的应用专家共识(2019)[J]. 中国实用妇科与产科杂志, 2019, 35(12): 1333-1339. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGSF201912014.htm
[7] Surbek D, Vial Y, Girard T, et al. Patient blood management(PBM)in pregnancy and childbirth: literature review and expert opinion[J]. Arch Gynecol Obstet, 2020, 301(2): 627-641. doi: 10.1007/s00404-019-05374-8
[8] Wang IJ, Bae BK, Park SW, et al. Pre-hospital modified shock index for prediction of massive transfusion and mortality in trauma patients[J]. Am J Emerg Med, 2020, 38(2): 187-190. doi: 10.1016/j.ajem.2019.01.056
[9] Borovac-Pinheiro A, Ribeiro FM, Morais SS, et al. Shock index and heart rate standard reference values in the immediate postpartum period: A cohort study[J]. PLoS One, 2019, 14(6): e0217907. doi: 10.1371/journal.pone.0217907
[10] Kohn JR, Dildy GA, Eppes CS. Shock index and delta-shock index are superior to existing maternal early warning criteria to identify postpartum hemorrhage and need for intervention[J]. J Matern Fetal Neonatal Med, 2019, 32(8): 1238-1244. doi: 10.1080/14767058.2017.1402882
[11] Oyelese Y, Ananth CV. Postpartum hemorrhage: epidemiology, risk factors, and causes[J]. Clin Obstet Gynecol, 2010, 53(1): 147-56. doi: 10.1097/GRF.0b013e3181cc406d
[12] 潘剑芳. 凶险性前置胎盘合并产后出血的影响因素分析[J]. 中国妇幼保健, 2020, 35(10): 1802-1804. https://www.cnki.com.cn/Article/CJFDTOTAL-ZFYB202010014.htm
[13] Edwards HM. Aetiology and treatment of severe postpartum haemorrhage[J]. Dan Med J, 2018, 65(3)130-139.
[14] Feduniw S, Warzecha D, Szymusik I, et al. Epidemiology, prevention and management of early postpartum hemorrhage-a systematic review[J]. Ginekol Pol, 2020, 91(1): 38-44. doi: 10.5603/GP.2020.0009
[15] Muñoz M, Stensballe J, Ducloy-Bouthors AS, et al. Patient blood management in obstetrics: prevention and treatment of postpartum haemorrhage. A NATA consensus statement[J]. Blood Transfus, 2019, 17(2): 112-136.
-




 下载:
下载: