Clinical significance of procalcitonin, C-reactive protein and white blood cell parameters in diagnosis of severity of neonatal sepsis
-
摘要: 目的 探究降钙素原(PCT)、C反应蛋白(CRP)及白细胞参数对新生儿败血症早期诊断治疗和病情评估的临床意义。方法 回顾性分析2019年1月至2020年12月收治的67例新生儿败血症患儿临床资料, 将其设为观察组, 选择同期收治的67例局部感染新生儿作为对照组, 比较2组患儿PCT、CRP、白细胞计数(WBC)、中性粒细胞计数(NEU)水平差异, 将存在显著差异的指标使用受试者工作特征曲线(ROC)对新生儿败血症的诊断效能进行分析。使用新生儿危重症评分(NCIS)对观察组患儿病情进行评估, 分析不同病情患儿PCT、CRP、WBC、NEU水平差异, 使用Spearman相关分析探究PCT、CRP、WBC、NEU水平与患儿病情的相关性。结果 观察组患儿PCT、CRP、WBC水平均高于对照组(均P< 0.05), 2组患儿NEU水平差异无统计学意义(P>0.05);ROC曲线结果显示, PCT、CRP、WBC水平对新生儿败血症的诊断效能均较高(AUC=0.893、0.848、0.923, 均P< 0.05);非危重组患儿PCT、CRP、WBC、NEU水平均低于危重组、极危重组, 危重组患儿PCT水平均低于极危重组(均P< 0.05), 危重组、极危重组患儿CRP、WBC、NEU水平差异无统计学意义(P>0.05);Spearman相关分析发现, 新生儿败血症患儿病情与PCT、CRP、WBC、NEU水平均呈正相关(r=0.856、0.700、0.654、0.598, 均P< 0.05)。结论 PCT、CRP、WBC可作为诊断新生儿败血症的指标, PCT、CRP、WBC、NEU可用于评估新生儿败血症患儿的病情严重程度。Abstract: Objective To explore the clinical significance of procalcitonin(PCT), C-reactive protein(CRP) and white blood cell parameters in the early diagnosis and treatment of neonatal sepsis and evaluation of disease severity.Methods The clinical data of 67 children with neonatal sepsis admitted to the hospital between January 2019 and December 2020 were retrospectively analyzed, and the patients were selected as observation group, and another 67 neonates with local infection treated during the same period were included in control group. The levels of PCT, CRP and white blood cell parameters(white blood cell count[WBC], neutrophil count[NEU]) were compared between the two groups. Receiver operating characteristic(ROC) curve was used to analyze the diagnostic efficiency of the indicator with significant differences on neonatal sepsis. Neonatal Critical Illness Score(NCIS) was applied to evaluate the disease severity of children in observation group, and the differences in levels of PCT, CRP and white blood cell parameters(WBC, NEU) were analyzed among children with different disease severity status. Spearman correlation analysis was used to explore the correlation between the levels of PCT, CRP, WBC and NEU and disease severity of children.Results The levels of PCT, CRP and WBC in observation group were higher than those in control group(allP< 0.05), and there was no significant difference in the level of NEU between the two groups(P>0.05). ROC curve results showed that the levels of PCT, CRP and WBC had high diagnostic efficiency on neonatal sepsis(AUC=0.893, 0.848, 0.923, allP< 0.05). The levels of PCT, CRP, WBC and NEU in non-critically ill group were lower than those in critically ill group and extremely ill group, and the level of PCT in critically ill group was lower than that in extremely ill group(allP< 0.05), and there were no statistical differences between critically ill group and extremely ill group in terms of CRP, WBC and NEU(P>0.05). Spearman correlation analysis showed that the disease severity of children with neonatal sepsis was positively correlated with the levels of PCT, CRP, WBC and NEU(r=0.856、0.700、0.654、0.598, allP< 0.05).Conclusion PCT, CRP, and WBC can be used as indicators for the diagnosis of neonatal sepsis. PCT, CRP, WBC, and NEU can be used to assess the severity of neonatal sepsis in children.
-
Key words:
- procalcitonin /
- C-reactive protein /
- white blood cell parameters /
- neonatal sepsis /
- diagnosis
-

-
表 1 不同患儿PCT、CRP、WBC、NEU水平比较
X±S 组别 PCT/(μg·L-1) CRP/(mg·L-1) WBC/(×109·L-1) NEU/% 观察组(67例) 13.18±6.86 15.12±4.62 25.15±6.12 46.85±8.73 对照组(67例) 5.11±1.38 9.57±2.68 13.38±5.66 44.06±10.43 t 9.435 8.505 11.564 1.679 P 0.001 0.001 0.001 0.096 表 2 PCT、CRP、WBC水平对新生儿败血症的诊断效能
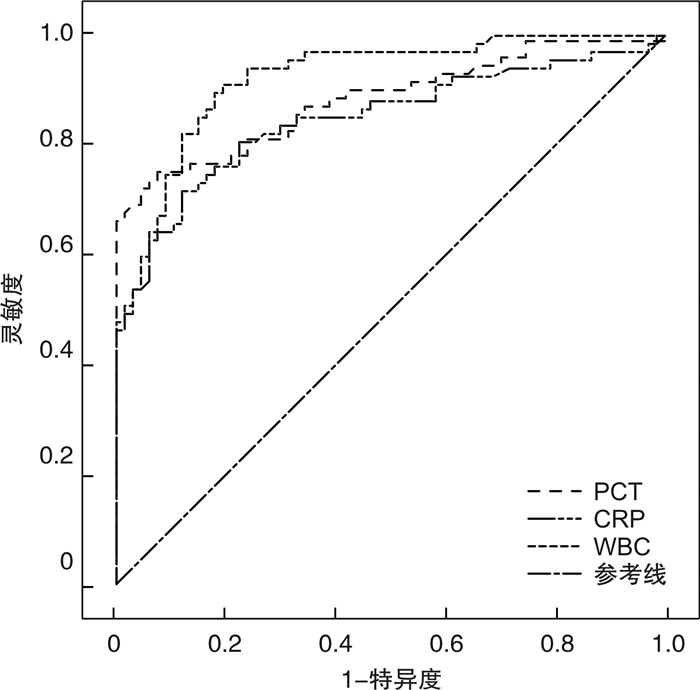
指标 预测标准 AUC 95%CI 敏感性/% 特异性/% P PCT 6.87 0.893 0.828~0.940 94.03 74.63 < 0.05 CRP 12.91 0.848 0.776~0.904 88.06 71.64 < 0.05 WBC 18.07 0.923 0.865~0.962 82.09 89.55 < 0.05 表 3 病情不同程度患儿PCT、CRP、WBC、NEU水平比较
X±S 组别 PCT/(μg·L-1) CRP/(mg·L-1) WBC/(×109·L-1) NEU/% 非危重组(31例) 7.05±2.30 11.36±3.10 20.58±3.61 40.93±6.22 危重组(21例) 16.52±4.42 18.09±3.39 28.61±5.67 51.22±6.52 极危重组(15例) 21.17±3.79 18.72±2.25 29.77±3.95 51.97±8.32 F 100.48 44.44 31.15 20.160 P 0.001 0.001 0.001 0.001 表 4 PCT、CRP、WBC、NEU水平与患儿病情的相关性分析
指标 r P PCT 0.856 0.001 CRP 0.700 0.001 WBC 0.654 0.001 NEU 0.598 0.001 -
[1] 李俊乔, 周启立, 刘利蕊, 等. C-反应蛋白、白细胞介素-6及降钙素原在新生儿早发型败血症中的诊断价值[J]. 中国妇幼保健, 2019, 34(12): 2746-2748. https://www.cnki.com.cn/Article/CJFDTOTAL-ZFYB201912028.htm
[2] 郭景瑞, 高奶荣, 祝颖, 等. 新生儿败血症T淋巴细胞亚群、PCT、CRP、Lac及炎症因子的检测及其临床意义[J]. 海南医学, 2020, 31(20): 2620-2622. doi: 10.3969/j.issn.1003-6350.2020.20.010
[3] 李园, 齐荣, 程雨嘉, 等. 降钙素原与新生儿败血症的相关性分析[J]. 中国妇幼健康研究, 2019, 30(10): 1196-1200. doi: 10.3969/j.issn.1673-5293.2019.10.003
[4] 崔海涛, 秦洪伟. PCT、CRP联合血清淀粉样蛋白A在细菌性肺炎与病毒性肺炎中的应用[J]. 临床血液学杂志, 2018, 31(8): 603-606. https://www.cnki.com.cn/Article/CJFDTOTAL-LCXZ201808009.htm
[5] 杨素艳, 孙夫强, 段洋. 早发型败血症早产儿脐血培养价值研究[J]. 中国全科医学, 2020, 23(27): 3422-3426. doi: 10.12114/j.issn.1007-9572.2020.00.380
[6] 中华医学会儿科学分会新生儿学组, 中国医师协会新生儿科医师分会感染专业委员会. 新生儿败血症诊断及治疗专家共识(2019年版)[J]. 中华儿科杂志, 2019, 57(4): 252-257. doi: 10.3760/cma.j.issn.0578-1310.2019.04.005
[7] 肖燕, 闫媛媛, 娄君鸽. 肺超声评分对评估新生儿感染性肺炎病情严重程度的应用价值分析[J]. 中华全科医学, 2020, 18(10): 1711-1714. https://www.cnki.com.cn/Article/CJFDTOTAL-SYQY202010028.htm
[8] 陆文峰, 张洁, 方成志. 新生儿败血症发病情况及早期诊断指标分析[J]. 中国妇幼健康研究, 2017, 28(8): 908-910. doi: 10.3969/j.issn.1673-5293.2017.08.005
[9] 马利, 修欣欣, 翟颖, 等. 降钙素原在严重创伤后脓毒血症诊断及预后中的临床应用价值[J]. 临床血液学杂志, 2019, 32(6): 411-414. https://www.cnki.com.cn/Article/CJFDTOTAL-LCXZ201906002.htm
[10] 严争, 陈涵强, 刘凡, 等. CD64联合C-反应蛋白及降钙素原检测在新生儿败血症的临床研究[J]. 中国小儿急救医学, 2017, 24(10): 725-728. doi: 10.3760/cma.j.issn.1673-4912.2017.10.002
[11] 谷磊, 杨玉芹, 王霞. PCT、hs-CRP及二者联合检测对新生儿败血症的诊断价值[J]. 检验医学, 2018, 33(7): 597-600. doi: 10.3969/j.issn.1673-8640.2018.07.004
[12] 施灵敏, 楼文文, 宫剑, 等. 降钙素原在新生儿败血症早期诊断中的价值[J]. 中国卫生检验杂志, 2019, 29(11): 1354-1356. https://www.cnki.com.cn/Article/CJFDTOTAL-ZWJZ201911024.htm
[13] 隆耀清. 血清CRP、SAA、PCT检测在新生儿败血症中的诊断价值[J]. 临床检验杂志(电子版), 2019, 8(3): 40-41. https://www.cnki.com.cn/Article/CJFDTOTAL-LNJI201903024.htm
[14] 朱丽坤, 温洁新. Hs-CRP与PCT在新生儿败血症早期诊断及病情评估中的应用[J]. 实用医学杂志, 2016, 32(6): 1002-1003. doi: 10.3969/j.issn.1006-5725.2016.06.044
-




 下载:
下载: