Clinicopathological features and prognosis of 207 patients with primary CD5-positive diffuse large B-cell lymphoma: a multicenter retrospective study of Huaihai Lymphoma Working Group
-
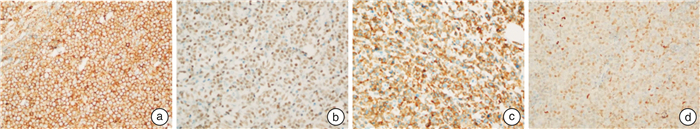
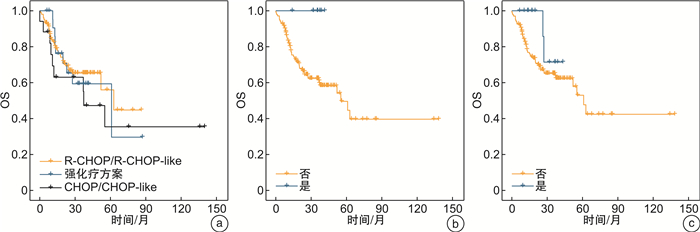
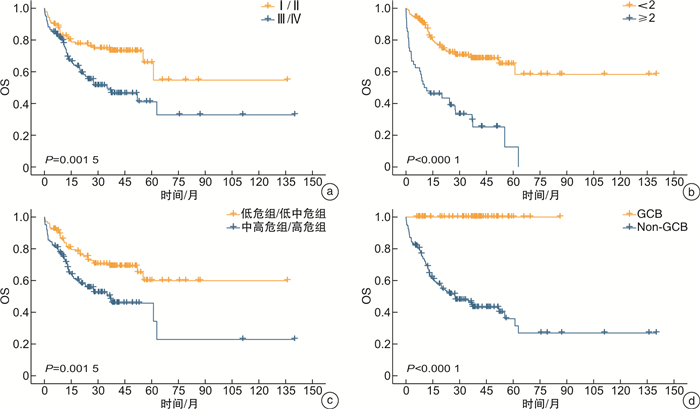
摘要: 目的 探讨原发性CD5阳性弥漫大B细胞淋巴瘤(CD5+DLBCL)的临床病理特征和预后影响因素。方法 收集2010年3月—2021年8月淮海淋巴瘤协作组中11家医疗中心确诊的207例CD5+DLBCL患者的临床资料。采用免疫组织化学方法分析患者的病理特征,基于Cox比例风险回归模型筛选CD5+DLBCL患者的预后影响因素。结果 207例患者中男102例,女105例,中位年龄61(24~90)岁,5年总体生存率为47.5%,Ann Arbor分期Ⅲ/Ⅳ期119例(57.5%),44例(21.3%)出现中枢神经受累,MYC/BCL-2双表达95例(45.9%)。采用R-CHOP/R-CHOP-like治疗方案、强化疗治疗方案和CHOP/CHOP-like治疗方案的患者间生存时间比较,差异均无统计学意义;接受BTK抑制剂泽布替尼治疗方案的患者生存时间明显优于未使用BTK抑制剂的患者(P=0.038)。Kaplan-Meier分析结果表明,Ann Arbor分期、ECOG评分、IPI评分和细胞起源影响患者的生存(P< 0.05)。多因素分析结果提示,年龄、白蛋白和ECOG评分是预后的独立影响因素(P< 0.05)。结论 CD5+DLBCL患者具有独特的临床病理特征,年龄、白蛋白和ECOG评分是预后的独立影响因素。
-
关键词:
- 原发性CD5阳性弥漫大B细胞淋巴瘤 /
- 临床病理特征 /
- 预后分析
Abstract: Objective To investigate the clinicopathological features and prognostic factors of primary CD5+diffuse large B-cell lymphoma(CD5+DLBCL).Methods Clinical data of 207 patients with CD5+DLBCL diagnosed in 11 medical centers in the Huaihai Lymphoma Working Group from March 2010 to August 2021 were collected. Immunohistochemical methods were used to analyze the pathological characteristics of patients, and Cox proportional risk regression model was used to screen the prognostic factors of CD5+DLBCL patients.Results The median age at diagnosis was 61(24-90) years old, with 102 males and 105 females. The overall 5-year survival rate was 47.5%. One hundred and nineteen cases(57.5%) were Ann Arbor stage Ⅲ/Ⅳ, 44 cases(21.3%) had central nervous system involvement, and 95 cases(45.9%) had MYC/BCL-2 double expression. There was no difference in survival among patients treated with R-CHOP/R-CHOP-like, intensive chemotherapy, or CHOP/CHOP-like, and patients treated with BTK inhibitor zanubrutinib had significantly better survival than those without BTK inhibitor(P=0.038). Kaplan-Meier analysis showed that Ann Arbor staging, ECOG score, IPI score and cell origin influenced survival(P< 0.05). Multivariate analysis indicated that age, albumin and ECOG score were independent prognostic factors(P< 0.05).Conclusion CD5+DLBCL patients have unique clinicopathological features, and age, albumin and ECOG score are independent prognostic factors. -

-
表 1 207例CD5+DLBCL患者的临床特征与免疫表型间的相关分析
临床特征 MYC/例 χ2 P BCL-2/例 χ2 P BCL-6/例 χ2 P - + - + - + 性别 男 66 36 0.023 0.879 31 71 0.019 0.892 45 57 0.360 0.548 女 69 36 31 74 42 63 B症状 无 103 45 4.386 0.036 41 107 1.252 0.263 56 92 3.744 0.053 有 32 27 21 38 31 28 中枢受累 无 111 52 2.805 0.094 45 118 2.009 0.156 65 98 1.457 0.227 有 24 20 17 27 22 22 骨髓受累 无 111 49 5.370 0.024 42 118 4.602 0.032 58 102 9.659 0.002 有 24 23 20 27 29 18 Ann Arbor分期 Ⅰ/Ⅱ期 61 27 1.135 0.287 27 61 0.039 0.844 31 57 2.907 0.088 Ⅲ/Ⅳ期 74 45 35 84 56 63 细胞起源 GCB 43 17 1.976 0.160 16 44 0.696 0.404 23 37 0.676 0.411 Non-GCB 92 55 46 101 64 83 表 2 存活组与死亡组患者间临床特征比较
例(%) 临床特征 存活组(126例) 死亡组(81例) χ2 P 临床特征 存活组(126例) 死亡组(81例) χ2 P Ann Arbor分期 9.036 0.003 BCL-2 0.053 0.818 Ⅰ/Ⅱ期 64(50.79) 24(29.63) 阴性 37(29.37) 25(30.86) Ⅲ/Ⅳ期 62(49.21) 57(70.37) 阳性 89(70.63) 56(69.14) ECOG评分 29.949 < 0.001 BCL-6 0.091 0.763 < 2 113(89.68) 24(29.63) 阴性 54(42.86) 33(40.74) ≥2 13(10.32) 57(70.37) 阳性 72(57.14) 48(59.26) MYC 2.082 0.149 Ki-67 0.307 0.580 阴性 87(69.05) 48(59.26) ≤90% 123(97.62) 78(96.30) 阳性 39(30.95) 33(40.74) > 90% 3(2.38) 3(3.70) 表 3 207例CD5+DLBCL患者的预后影响因素分析
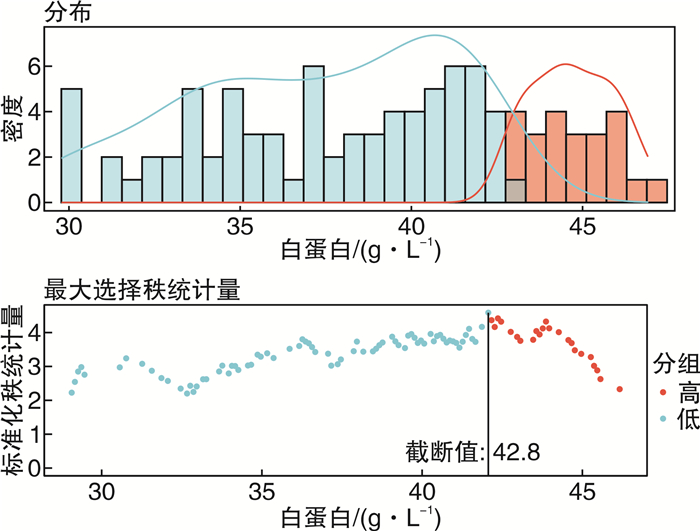
单因素分析 多因素分析 变量 HR P 变量 HR 95%CI P 年龄 > 74岁 4.313 < 0.001 年龄 红细胞计数 > 4.2×109/L 0.354 < 0.001 ≤74岁 白蛋白 > 42.8 g/L 0.269 < 0.001 > 74岁 6.791 2.514~18.341 < 0.001 血红蛋白 > 131.0 g/L 0.448 0.003 白蛋白 中性粒细胞计数 > 3.8×109/L 2.081 0.003 ≤42.8 g/L 乳酸脱氢酶 > 344.0 U/L 1.984 0.003 > 42.8 g/L 0.265 0.103~0.684 0.006 白细胞计数 > 5.8×109/L 2.040 0.004 ECOG评分 Ann Arbor分期(Ⅲ/Ⅳ期) 2.132 0.002 < 2 ECOG评分 > 2 3.288 < 0.001 ≥2 2.401 1.233~4.673 0.010 IPI评分(中高危组/高危组) 2.263 0.001 红细胞计数 B症状(有) 1.814 0.010 ≤4.2×109/L 中枢受累(有) 1.798 0.015 > 4.2×109/L 0.252 0.063~1.010 0.052 -
[1] Sehn LH, Salles G. Diffuse Large B-Cell Lymphoma[J]. N Engl J Med, 2021, 384(9): 842-858. doi: 10.1056/NEJMra2027612
[2] 谢萌, 张青青, 郭瑞昕, 等. 头颈部弥漫大B细胞淋巴瘤的临床特征分析[J]. 临床耳鼻咽喉头颈外科杂志, 2022, 36(1): 1-7. https://www.cnki.com.cn/Article/CJFDTOTAL-LCEH202201001.htm
[3] 徐卫, 梁金花. 弥漫大B细胞淋巴瘤新基因分型及分子靶向的治疗进展[J]. 临床血液学杂志, 2020, 33(9): 594-598. https://www.cnki.com.cn/Article/CJFDTOTAL-LCXZ202009002.htm
[4] Durani U, Ansell SM. CD5+ diffuse large B-cell lymphoma: a narrative review[J]. Leuk Lymphoma, 2021, 62(13): 3078-3086. doi: 10.1080/10428194.2021.1953010
[5] Na HY, Choe JY, Shin SA, et al. Characteristics of CD5-positive diffuse large B-cell lymphoma among Koreans: High incidence of BCL2 and MYC double-expressors[J]. PLoS One, 2019, 14(10): e0224247. doi: 10.1371/journal.pone.0224247
[6] Shen Z, Wang L, Zhang B, et al. Development and Validation of a Novel Prognostic Nomogram for CD5-Positive Diffuse Large B-Cell Lymphoma: A Retrospective Multicenter Study in China[J]. Front Oncol, 2021, 11: 754180. doi: 10.3389/fonc.2021.754180
[7] Hans CP, Weisenburger DD, Greiner TC, et al. Confirmation of the molecular classification of diffuse large B-cell lymphoma by immunohistochemistry using a tissue microarray[J]. Blood, 2004, 103(1): 275-282. doi: 10.1182/blood-2003-05-1545
[8] Burgueño-Bucio E, Mier-Aguilar CA, Soldevila G. The multiple faces of CD5[J]. J Leukoc Biol, 2019, 105(5): 891-904. doi: 10.1002/JLB.MR0618-226R
[9] Thakral B, Medeiros LJ, Desai P, et al. Prognostic impact of CD5 expression in diffuse large B-cell lymphoma in patients treated with rituximab-EPOCH[J]. Eur J Haematol, 2017, 98(4): 415-421. doi: 10.1111/ejh.12847
[10] Xu Y, Sun W, Li F. De Novo CD5+ Diffuse Large B-Cell Lymphoma: Biology, Mechanism, and Treatment Advances[J]. Clin Lymphoma Myeloma Leuk, 2020, 20(10): e782-e790. doi: 10.1016/j.clml.2020.05.003
[11] Zhao P, Li L, Zhou S, et al. CD5 expression correlates with inferior survival and enhances the negative effect of p53 overexpression in diffuse large B-cell lymphoma[J]. Hematol Oncol, 2019, 37(4): 360-367. doi: 10.1002/hon.2657
[12] Tang H, Zhou H, Wei J, et al. Clinicopathologic significance and therapeutic implication of de novo CD5+ diffuse large B-cell lymphoma[J]. Hematology, 2019, 24(1): 446-454. doi: 10.1080/16078454.2019.1614289
[13] 王保峰, 胡红霞. 伴CD5表达的原发性弥漫大B细胞淋巴瘤患者的临床及预后特征分析[J]. 广东医学, 2020, 41(9): 915-920. https://www.cnki.com.cn/Article/CJFDTOTAL-GAYX202009013.htm
[14] 苏永宏, 焦宁超. 沙利度胺联合R-CHOP化疗方案对CD20阳性弥漫大B细胞淋巴瘤患者疗效及其对TNF-α、PDGF-BB的影响[J]. 临床血液学杂志, 2020, 33(5): 326-329. https://www.cnki.com.cn/Article/CJFDTOTAL-LCXZ202005007.htm
[15] Ge J, Xia Y, Sun Z, et al. Improving outcomes in limited-stage de novo CD5+ DLBCL: systemic approaches with consolidative radiation[J]. Leuk Lymphoma, 2022, 63(6): 1369-1374. doi: 10.1080/10428194.2021.2023742
[16] Hyo R, Tomita N, Takeuchi K, et al. The therapeutic effect of rituximab on CD5-positive and CD5-negative diffuse large B-cell lymphoma[J]. Hematol Oncol, 2010, 28(1): 27-32.
[17] Miyazaki K, Asano N, Yamada T, et al. DA-EPOCH-R combined with high-dose methotrexate in patients with newly diagnosed stage Ⅱ-Ⅳ CD5-positive diffuse large B-cell lymphoma: a single-arm, open-label, phase Ⅱ study[J]. Haematologica, 2020, 105(9): 2308-2315. doi: 10.3324/haematol.2019.231076
[18] Miyazaki K, Yamaguchi M, Suzuki R, et al. CD5-positive diffuse large B-cell lymphoma: a retrospective study in 337 patients treated by chemotherapy with or without rituximab[J]. Ann Oncol, 2011, 22(7): 1601-1607. doi: 10.1093/annonc/mdq627
-




 下载:
下载: