-
摘要: 目的 通过相关肝功能指标分析,探讨不同程度新生儿高胆红素血症患儿肝脏的损伤程度。方法 回顾性分析2022年1月—2022年12月医院收治的191例新生儿高胆红素血症患儿,以及同期体检的48例健康新生儿的临床资料。按照血清总胆红素(total bilirubin,TBIL)水平分为轻度组(n=74)、中度组(n=53)、重度组(n=64)以及对照组(n=48)4组。检测轻、中、重度组以及对照组新生儿的TBIL、谷丙转氨酶(alanine aminotransferase,ALT)、谷草转氨酶(aspartate aminotransferase,AST)、γ-谷氨酰转移酶(γ-glutamyltransferase,GGT)、碱性磷酸酶(alkaline phosphatase,ALP)、乳酸脱氢酶(lactic dehydrogenase,LDH)、羟丁酸脱氢酶(hydroxybutyrate dehydrogenase,HBDH)水平。统计分析4组肝功能指标,同时将肝功能指标与TBIL水平进行Pearson相关性分析。结果 轻、中、重度组以及对照组4组之间肝功能指标(ALT、AST、ALP、GGT、LDH、HBDH)差异有统计学意义(P<0.05),中度组AST、GGT、ALP、LDH、HBDH水平显著高于对照组(P<0.05),重度组ALT、AST、GGT、LDH、HBDH水平显著高于轻度组(P<0.05),重度组AST、HBDH水平显著高于中度组(P<0.05),ALT、AST、GGT、LDH、HBDH与TBIL水平之间呈显著正相关(P<0.05),而ALP与TBIL水平无相关性(P>0.05)。结论 在新生儿高胆红素血症患儿中,TBIL水平越高,肝脏受损程度越深,因此需要密切关注患儿的肝功能指标,监测病情进展情况,及时准确地开展相应的诊疗措施。Abstract: Objective To analyze the degree of liver injury in neonates with different degrees of hyperbilirubinemia using related liver function indexes.Methods The clinical data of 191 neonates with neonatal hyperbilirubinemia admitted to our hospital from January 2022 to December 2022 and 48 healthy neonates who underwent physical examination during the same period were retrospectively analyzed. According to the serum total bilirubin(TBIL) level, the patients were divided into four groups: mild group(n=74), moderate group(n=53), severe group(n=64) and control group(n=48). The levels of TBIL, alanine aminotransferase(ALT), aspartate aminotransferase(AST), γ-glutamyltransferase(GGT), alkaline phosphatase(ALP), lactic dehydrogenase(LDH)and hydroxybutyrate dehydrogenase(HBDH)in the mild, moderate and severe groups and the control group were detected. The liver function indexes(ALT, AST, ALP, GGT, LDH, HBDH) of the four groups were statistically analyzed, and Pearson correlation analysis was performed between the liver function indexes and the level of TBIL.Results There were significant differences in liver function indexes among the mild, moderate, severe groups and the control group(P<0.05). The levels of AST, GGT, ALP, LDH, HBDH in the moderate group were significantly higher than those in the control group(P<0.05). The levels of ALT, AST, GGT, LDH and HBDH in the severe group were significantly higher than those in the mild group(P<0.05), and the levels of AST and HBDH in the severe group were significantly higher than those in the moderate group(P<0.05). ALT, AST, GGT, LDH and HBDH were positively correlated with TBIL level(P<0.05), while ALP was not correlated with TBIL level(P>0.05).Conclusion In newborn children with high blood bilirubin, different levels of bilirubin may cause a certain degree of damage to the liver function. The higher bilirubin level, the deeper the degree of liver damage. So it need to pay close attention to the patient's liver function indicators, monitoring the progress of the disease, carry out the corresponding treatment measures timely and accurately.
-

-
表 1 4组血清肝功能指标ALT、AST、ALP、GGT、LDH、HBDH水平比较
U/L,X±S 指标 对照组 轻度组 中度组 重度组 F P ALT 9.471±9.562 9.572±6.861 12.304±7.477 13.342±8.0831)2) 3.704 0.012 AST 23.851±15.413 27.322±9.016 33.963±12.1021)2) 39.303±17.6311)2)3) 14.597 <0.001 ALP 189.891±78.614 237.692±70.0601) 242.131±72.3821) 238.675±74.9071) 5.665 0.001 GGT 115.831±131.373 126.153±61.412 163.092±112.8341)2) 173.634±92.0951)2) 4.679 0.003 LDH 383.431±130.793 411.669±96.563 476.402±135.8441)2) 504.754±105.1841)2) 13.513 <0.001 HBDH 222.771±63.422 266.895±77.7671) 291.139±82.5031)2) 325.254±98.8261)2)3) 14.868 <0.001 与对照组比较,1)P<0.05;与轻度组比较,2)P<0.05;与中度组比较,3)P<0.05。 -
[1] 刘翠兰, 熊伶俐, 唐川婷. 高胆红素血症患儿肝肾功能及心肌酶血清学水平表达及临床意义[J]. 湖南师范大学学报(医学版), 2021, 18(4): 163-166.
[2] Routray SS, Behera R, Mallick B, et al. The spectrum of hemolytic disease of the newborn: evaluating the etiology of unconjugated hyperbilirubinemia among neonates pertinent to immunohematological workup[J]. Cureus, 2021, 13(8): e16940.
[3] 孙梅, 李健. 儿童高胆红素血症[J]. 中国实用儿科杂志, 2022, 37(7): 500-504.
[4] 张展, 管蓉, 薛晓霞, 等. 新生儿高胆红素血症患儿肝肾功能、心肌标志物与总胆红素的关系[J]. 分子诊断与治疗杂志, 2021, 13(12): 2047-2050, 2055.
[5] Myle AK, Al-Khattabi GH. Hemolytic disease of the newborn: a review of current trends and prospects[J]. Pediatric Health Med Ther, 2021, 12: 491-498. doi: 10.2147/PHMT.S327032
[6] 孙然, 侯军林, 张圣强. 凝血功能在评估肝脏疾病中的临床意义[J]. 临床和实验医学杂志, 2022, 21(8): 881-884.
[7] 师淑锋, 李晶, 王孝勇. 不同严重程度高胆红素血症新生儿血清AST、CK-MB、LDH、BUN、TBiL水平的表达及临床意义[J]. 保健医学研究与实践, 2022, 19(1): 72-75.
[8] 邵肖梅, 叶鸿瑁, 丘小汕. 实用新生儿学[M]. 4版. 北京: 人民卫生出版社, 2011: 273.
[9] 董青青, 叶光勇. 新生儿ABO溶血病患儿血型及多因素分析[J]. 临床血液学杂志, 2022, 35(6): 410-413, 418. https://lcxy.whuhzzs.com/article/doi/10.13201/j.issn.1004-2806.2022.06.005
[10] Jie J. Effects of comfort care combined with blue-light phototherapy on neonatal jaundice and total bilirubin and high-sensitivity C-reactive protein levels[J]. J King Saud Univ Sci, 2023, 35(2): 102483. doi: 10.1016/j.jksus.2022.102483
[11] Jiang N, Qian L, Lin GK, et al. Maternal blood parameters and risk of neonatal pathological jaundice: a retrospective study[J]. Sci Rep, 2023, 13(1): 26-27. doi: 10.1038/s41598-022-27267-8
[12] Noureldein M, Hill C, Ali A, et al. Neonatal jaundice in infants born at 37 weeks: is NICE treating too many?[J]. Arch Dis Child Fetal Neonatal Ed, 2023, 108(5): 547-548. doi: 10.1136/archdischild-2022-325075
[13] 李洁, 戴丽凤. 血清AST、CKMB、LDH、BUN及TBiL水平表达及对高胆红素血症新生儿的临床意义[J]. 中国妇幼保健, 2019, 34(19): 4481-4484.
[14] Wang HY, Su M, Yang B, et al. The influence of hyperbilirubinemia on indexes of kidney function in neonates[J]. Pediatr Nephrol, 2021, 36(11): 3711-3716. doi: 10.1007/s00467-021-05151-3
[15] Du LZ, Ma XL, Shen XX, et al. Neonatal hyperbilirubinemia management: clinical assessment of bilirubin production[J]. Semin Perinatol, 2021, 45(1): 151351. doi: 10.1016/j.semperi.2020.151351
[16] 米凯, 黄锐. 尿石素A预处理对肝缺血再灌注损伤大鼠模型的保护作用[J]. 临床肝胆病杂志, 2020, 36(8): 1783-1787.
[17] 陈建丽. 肝炎肝硬化患者的肝功能检测结果分析及其临床指导价值[J]. 吉林医学, 2022, 43(3): 808-810.
[18] 古挹端, 叶华英. 临床生化检验在肝脏疾病诊断中的应用价值探讨[J]. 临床医学工程, 2021, 28(10): 1351-1352.
[19] 吴晓双, 安宁, 陈要臻, 等. 游离血红素直接致肝细胞损伤的研究[J]. 临床输血与检验, 2023, 25(4): 444-449.
[20] Parisse S, Gianoncelli A, Isani G, et al. Severity of hepatocyte damage and prognosis in cirrhotic patients correlate with hepatocyte magnesium depletion[J]. Nutrients, 2023, 15(11): 2626. doi: 10.3390/nu15112626
[21] 王姗, 吴庆旺. Hepatology G蛋白偶联胆汁酸受体1和半胱氨酸白三烯受体1的相互作用揭示胆汁酸和白三烯在药物性肝损伤中的影响机制[J]. 临床肝胆病杂志, 2022, 38(11): 2550.
[22] 廖月, 何毅怀, 罗亚文. 氧化应激在急性肝损伤中的作用[J]. 临床肝胆病杂志, 2022, 38(10): 2402-2407.
[23] Aasam AI, Hasan BM, Jalil RA, et al. Cord blood albumin as a predictor of neonatal jaundice[J]. Niger J Clin Pract, 2023, 26(1): 55-58. doi: 10.4103/njcp.njcp_170_22
[24] 韩东煜. 临床生化检验在肝脏疾病患者中的应用价值分析[J]. 中国现代药物应用, 2019, 13(19): 25-26.
[25] 王星, 冯丽, 王晓卫, 等. 血清心肌损伤标志物在新生儿高胆红素血症中诊疗的临床意义[J]. 临床血液学杂志, 2022, 35(12): 878-880, 883. https://lcxy.whuhzzs.com/article/doi/10.13201/j.issn.1004-2806.2022.12.009
[26] 杨志梅. 血清γ-谷氨酰转肽酶碱性磷酸酶总胆汁酸与高胆红素血症新生儿总胆红素水平的相关性分析[J]. 基层医学论坛, 2020, 24(20): 2910-2912.
[27] 程淑一. 新生儿总胆红素水平对肝肾功能及心肌酶谱的影响[J]. 临床医学, 2016, 36(12): 104-105.
-

| 引用本文: | 李亭, 王星, 冯丽, 等. 不同程度新生儿高胆红素血症患儿肝脏损伤程度分析[J]. 临床血液学杂志, 2024, 37(2): 99-102. doi: 10.13201/j.issn.1004-2806.2024.02.005 |
| Citation: | LI Ting, WANG Xing, FENG Li, et al. Analysis of liver injury in neonates with different degrees of hyperbilirubinemia[J]. J Clin Hematol, 2024, 37(2): 99-102. doi: 10.13201/j.issn.1004-2806.2024.02.005 |
- Figure 1.
- Figure 2.
- Figure 3.
- Figure 4.
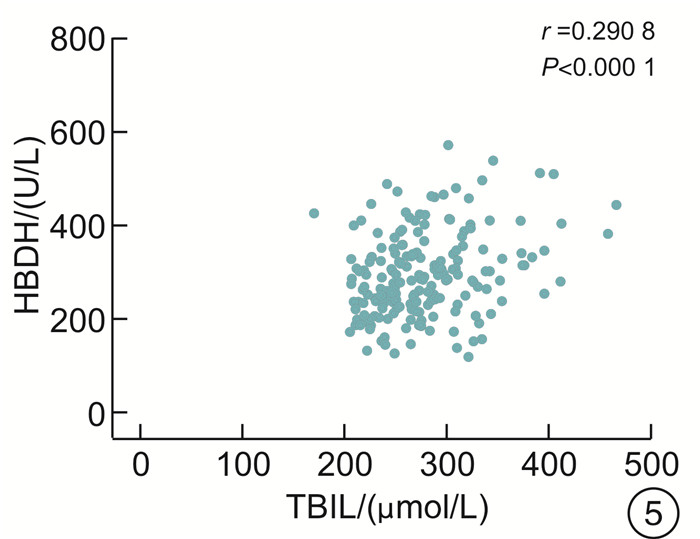
- Figure 5.
- Figure 6.




 下载:
下载: