Relationship between iron deficiency anemia during pregnancy and paraoxonase-1 level and perinatal outcome
-
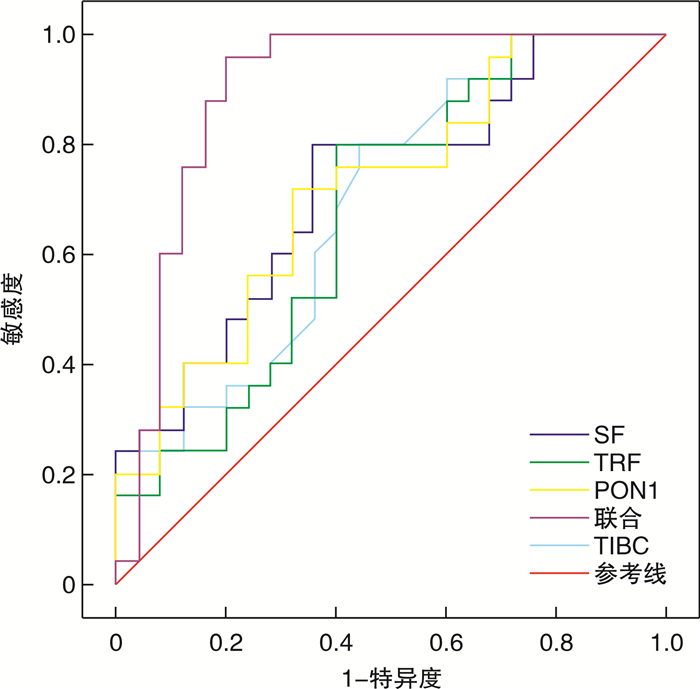
摘要: 目的 分析妊娠期缺铁性贫血指标,铁蛋白(SF)、转铁蛋白(TRF)、总铁结合力(TIBC)及对氧磷酶-1(PON-1)水平与围生结局的关系。方法 选取2017年1月—2020年1月收治的116例妊娠期贫血患者作为观察组,并选取同期100例妊娠期正常女性作为对照组,检测血清SF、TRF、TIBC、PON-1水平,并记录围生结局,采用多因素logistic回归分析影响围生结局的独立危险因素;同时绘制ROC曲线分析血清SF、TRF、TIBC、PON-1水平预测围生结局的价值。结果 观察组血清SF、PON-1水平低于对照组,TRF、TIBC高于对照组(P< 0.05);观察组妊娠期高血压、产后出血、胎膜早破及早产发生率高于对照组(P< 0.05);妊娠期高血压、产后出血、胎膜早破及早产患者血清SF、PON-1水平低于非妊娠期高血压、产后出血、胎膜早破及早产患者,TRF、TIBC水平高于非妊娠期高血压、产后出血、胎膜早破及早产患者(P< 0.05);多因素logistic回归分析显示,血清SF、TRF、TIBC、PON-1水平是影响围生结局的独立危险因素(P< 0.05);ROC曲线分析显示,血清SF、TRF、TIBC、PON-1水平联合预测围生结局的敏感度及特异度均高于单独预测(P< 0.05)。结论 妊娠期贫血患者血清SF、PON-1水平呈低表达,TRF、TIBC水平呈高表达,对围生结局预测价值较高,同时也是影响妊娠期贫血围生结局的独立危险因素。Abstract: Objective To analyze the relationship between the levels of ferritin(SF), transferrin(TRF), total iron binding force(TIBC) and paraoxonase-1(PON-1) and the perinatal outcome of iron deficiency anemia during pregnancy.Methods A total of 116 patients with gestational anemia admitted to the hospital from January 2017 to January 2020 were enrolled as observation group, while other 100 normal pregnant women were enrolled as control group. The levels of SF, TRF, TIBC and PON-1 were detected, and perinatal outcomes were recorded. The independent risk factors affecting perinatal outcomes were analyzed by multivariate logistic regression analysis. The predictive value of serum SF, TRF, TIBC and PON-1 levels for perinatal outcomes was analyzed by ROC curves.Results The levels of SF and PON-1 in observation group were lower than those in control group, while TRF and TIBC were higher than those in control group(P< 0.05). The incidences of gestational hypertension, postpartum hemorrhage, premature rupture of membranes and premature delivery in observation group were higher than those in control group(P< 0.05). The levels of serum SF and PON-1 in the patients with gestational hypertension, postpartum hemorrhage, premature rupture of membranes and premature delivery were lower than those without gestational hypertension, postpartum hemorrhage, premature rupture of membranes or premature delivery, while TRF and TIBC were higher than those patients(P< 0.05). Multivariate logistic regression analysis showed that levels of SF, TRF, TIBC and PON-1 were independent risk factors affecting perinatal outcomes(P< 0.05). ROC curves analysis showed that sensitivity and specificity of SF combined with TRF, TIBC and PON-1 for predicting perinatal outcomes were higher than those of single index(P< 0.05).Conclusion The levels of SF and PON-1 are low, while levels of TRF and TIBC are high in the patients with gestational anemia. They may be of high predictive value for perinatal outcomes, which can be also independent risk factors that affect perinatal outcomes of gestational anemia.
-

-
表 1 2组血清SF、TRF、TIBC、PON-1水平比较
X±S 组别 SF/(μg·L-1) TRF/(g·L-1) TIBC/(μmol·L-1) Pon-1/(U·L-1) 观察组(n=116) 63.40±10.57 3.58±1.02 75.29±14.37 460.22±42.37 对照组(n=100) 97.52±15.22 2.20±0.57 51.42±9.55 652.77±50.28 t 19.337 12.007 14.135 78.132 P < 0.001 < 0.001 < 0.001 < 0.001 表 2 2组围生结局比较
例(%) 组别 妊娠期高血压 产后出血 胎膜早破 早产 观察组(n=116) 12(10.34) 13(11.21) 18(15.52) 13(11.21) 对照组(n=100) 3(3.00) 3(3.00) 2(2.00) 3(3.00) χ2 4.483 5.274 11.679 5.274 P 0.034 0.022 0.001 0.022 表 3 不同围生结局血清SF、TRF、TIBC、PON-1水平比较
X±S 组别 SF/(μg·L-1) TRF/(g·L-1) TIBC/(μmol·L-1) Pon-1/(U·L-1) 妊娠期高血压 有(n=11) 57.64±7.621) 3.19±0.531) 70.22±12.031) 496.20±46.341) 无(n=105) 75.22±12.04 2.36±0.25 57.22±9.34 600.23±50.17 产后出血 有(n=10) 56.19±7.501) 3.15±0.501) 69.19±11.971) 497.03±46.381) 无(n=106) 76.23±12.18 2.41±0.30 57.90±10.17 601.22±50.87 胎膜早破 有(n=18) 55.28±6.961) 3.12±0.471) 70.30±12.111) 496.88±46.451) 无(n=98) 74.98±11.95 2.34±0.24 58.04±9.24 602.31±51.04 早产 有(n=13) 56.07±7.421) 3.17±0.521) 70.10±11.821) 497.23±16.501) 无(n=103) 74.80±11.88 2.36±0.25 57.92±10.20 600.88±50.24 与无妊娠期高血压、无产后出血、无胎膜早破及无早产患者比较,1)P < 0.05。 表 4 影响围生结局的多因素logistic回归分析
因素 β SE Wald χ2 P OR 95%CI SF 1.177 0.347 11.505 0.001 3.245 1.644~6.405 TRF 1.135 0.352 10.397 0.002 3.111 1.561~6.202 TIBC 1.124 0.402 7.818 0.005 3.077 1.399~6.766 Pon-1 1.117 0.380 8.641 0.003 3.056 1.451~6.435 -
[1] 史生辉, 李燕君, 李生有, 等. 健脾生血片与右旋糖酐铁片治疗妊娠期缺铁性贫血的临床对比研究[J]. 世界中医药, 2018, 13(9): 2241-2243. https://www.cnki.com.cn/Article/CJFDTOTAL-SJZA201809036.htm
[2] 于修文, 杨慧健. 原始细胞不增多骨髓增生异常综合征骨髓细胞发育异常特征分析[J]. 临床血液学杂志, 2019, 32(6): 418-422. http://lcxz.cbpt.cnki.net/WKC/WebPublication/paperDigest.aspx?paperID=eb6f5215-a665-434c-880e-8635db2f695c
[3] 刘馨遥, 邵盈盈. 妊娠期贫血患者血常规检测情况及妊娠结局分析[J]. 中国妇幼保健, 2020, 35(5): 823-826. https://www.cnki.com.cn/Article/CJFDTOTAL-ZFYB202005013.htm
[4] 张琳, 宋玮钕, 黄桉风, 等. 妊娠期缺铁性贫血患者血Hb、SF、PON1水平与围生结局的关系[J]. 浙江医学, 2019, 41(12): 1295-1297, 1333. https://www.cnki.com.cn/Article/CJFDTOTAL-ZJYE201912019.htm
[5] 张亚平, 李姣, 吴文新, 等. 肝癌贫血患者血清hepcidin的表达及与炎性因子的相关性分析[J]. 河北医药, 2019, 41(3): 421-424. https://www.cnki.com.cn/Article/CJFDTOTAL-HBYZ201903024.htm
[6] 王青波, 林宏, 张国军, 等. sTfR、EPO的检测对孕妇缺铁性贫血诊断价值分析[J]. 标记免疫分析与临床, 2019, 26(1): 37-39, 69. https://www.cnki.com.cn/Article/CJFDTOTAL-BJMY201901009.htm
[7] 杜宝丽, 李晓燕, 孙琪. 妊娠期和产后严重贫血孕产妇不良妊娠结局风险的多水平分析研究[J]. 中国性科学, 2020, 29(11): 58-63. https://www.cnki.com.cn/Article/CJFDTOTAL-XKXZ202011020.htm
[8] 张瀚月, 张璐璐, 许瑞, 等. 网织红细胞血红蛋白含量等指标在妊娠期缺铁性贫血筛检中的意义[J]. 中国医药, 2019, 14(5): 763-767. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGYG201905030.htm
[9] 陈慧, 熊尚全; ,杨新春, 等. 调理气血类中成药防治动脉粥样硬化性心血管疾病临床应用专家共识[J]. 临床心血管病杂志, 2020, 36(2): 97-104. https://www.cnki.com.cn/Article/CJFDTOTAL-LCXB202002001.htm
[10] 单秀玲, 董其虎, 孙璐, 等. 孕早期铁缺乏与妊娠和出生结局关系[J]. 中国计划生育学杂志, 2019, 27(12): 1704-1706. https://www.cnki.com.cn/Article/CJFDTOTAL-JHSY201912037.htm
[11] 周丽, 孟文颖. 妊娠期血清转铁蛋白、总铁结合力与妊娠期代谢综合征相关性[J]. 中国计划生育学杂志, 2020, 28(12): 2098-2101. https://www.cnki.com.cn/Article/CJFDTOTAL-JHSY202012043.htm
[12] 余敏, 陈道平, 文静. 老年缺铁性贫血患者体液免疫和细胞免疫功能的变化[J]. 贵州医科大学学报, 2018, 43(6): 698-702. https://www.cnki.com.cn/Article/CJFDTOTAL-GYYB201806018.htm
[13] 董淑晓, 刘志虎, 石国素. 子痫前期患者PON1活性和AOPP水平及对疾病严重程度的影响[J]. 中国妇幼保健, 2019, 34(12): 2698-2701. https://www.cnki.com.cn/Article/CJFDTOTAL-ZFYB201912012.htm
[14] 张若尘, 马爱群, 卢群. PON1浓度在冠心病合并肥胖患者中的变化及其与代谢状态、炎性反应的相关性[J]. 中国分子心脏病学杂志, 2020, 20(4): 3459-3463. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGFB202004006.htm
[15] 张凤霞, 孙艳艳, 郑秀芬, 等. 转铁蛋白、血清铁及不饱和铁结合力联合检测对妊娠期缺铁性贫血的临床价值[J]. 中国医刊, 2018, 53(04): 438-441. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGYI201804026.htm
-




 下载:
下载: