Predictive value of albumin/globulin on renal damage and severity in patients with systemic lupus erythematosus
-
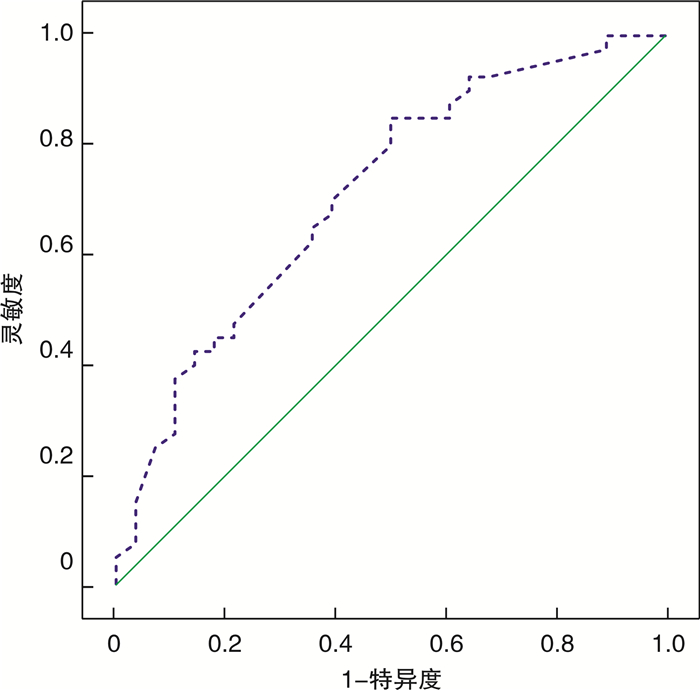
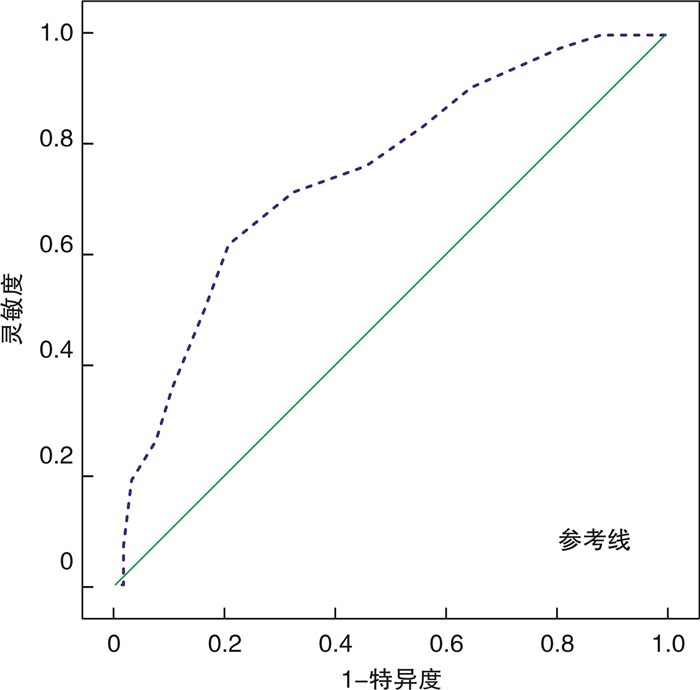
摘要: 目的 探讨白蛋白/球蛋白(AGR)对系统性红斑狼疮(SLE)合并肾损害和肾脏损伤程度预测价值的研究。方法 选取SLE患者110例, 根据有无肾损害分为狼疮肾炎组(LN组)和非狼疮肾炎组(非LN组), LN患者中根据尿素氮(BUN)、肌酐(Cr)是否超过参考值分为肾功能异常组和肾功能正常组, 比较以上组别临床资料差异, 分析AGR在纠正混杂因素前后对LN和肾功能异常的影响。结果 AGR预测非LN的曲线下面积(AUC)为0.748(0.655~0.842), 最佳截断值为1.35。AGR预测肾功能正常LN患者的AUC为0.713(0.588~0.838), 最佳截断值为1.20。LN组SLE疾病活动指数(SLE-DAI)、C反应蛋白(CRP)、血沉(ESR)均高于非LN组, 血红蛋白(Hb)、AGR≥1.35占比低于非LN组, 差异有统计学意义(P< 0.05)。校正混杂因素前后AGR≥1.35对LN的比值比(OR)分别为0.196、0.275。肾功能异常组SLE-DAI、CRP、BUN、Cr、尿微量白蛋白/尿肌酐(ACR)均高于肾功能正常组, AGR≥1.20低于肾功能正常组, 差异有统计学意义(P< 0.05)。校正混杂因素前后AGR≥1.20对肾功能受损LN的OR分别为0.270、0.313。AGR与Hb呈正相关, 与CRP、SLE-DAI、ESR呈负相关, LN患者中AGR与BUN、Cr、ACR呈负相关。结论 AGR可以作为评估SLE肾损害及损害程度的潜在血清学指标。Abstract: Objective To investigate the predictive value of albumin / globulin (AGR) on renal damage and severity in patients with systemic lupus erythematosus(SLE).Methods 110 SLE patients in our hospital were divided into lupus nephritis group(LN) and non LN group according to renal damage. LN patients were divided into abnormal renal function group and normal renal function group according to whether BUN and Cr exceeded the reference value. The differences of clinical data between the above groups were compared, and the effects of AGR on LN and abnormal renal function before and after correcting confounding factors were analyzed.Results The area under the curve(AUC) of AGR for predicting non LN was 0.748(0.655-0.842), and the best cut off value was 1.35. The AUC of normal renal function predicted by AGR was 0.713(0.588-0.838), and the best cut off value was 1.20. The disease activity index(SLE-DAI), C-reactive protein(CRP) and erythrocyte sedimentation rate(ESR) of LN group were higher than those of non LN group, and the proportions of hemoglobin(Hb) and AGR ≥ 1.35 were lower than those of non LN group(allP< 0.05). After adjusting for confounding factors, theORof AGR ≥ 1.35 for LN was 0.196 and 0.275, respectively. The SLE-DAI, CRP, BUN, Cr and ACR in the abnormal renal function group were higher than those in the normal renal function group, and the proportion of AGR ≥ 1.20 was lower than that in the normal renal function group, the differences were statistically significant(allP< 0.05). After adjusting for confounding factors, theORof AGR ≥ 1.20 on renal function impairment was 0.270 and 0.313, respectively. AGR was positively correlated with Hb and negatively correlated with CRP, SLE-DAI and ESR. In LN patients, AGR was negatively correlated with BUN, Cr and ACR.Conclusion AGR can be used as a potential serological marker to evaluate the renal damage in SLE.
-
Key words:
- systemic lupus erythematosus /
- lupus nephritis /
- serum albumin /
- globulin /
- predictive value
-

-
表 1 LN组和非LN组临床资料比较
X±S 变量 LN组(62例) 非LN组(48例) t/χ2 P 年龄/岁 42.54±6.76 44.77±7.99 1.584 0.116 性别(男/女)/例 7/55 6/42 0.038 0.845 病程/月 11.35±5.33 10.29±6.21 0.962 0.338 SLE-DAI 10.26±3.29 8.33±3.67 2.901 0.005 既往史/例 吸烟 10 9 0.196 0.906 饮酒 8 8 过敏 12 9 实验室指标 AGR≥1.35(是/否)/例 20/42 34/14 16.109 < 0.001 Hb/(g·L-1) 106.54±16.27 114.33±12.39 2.755 0.007 RDW/fl 47.54±3.64 46.33±2.73 1.922 0.057 CRP/(mg·L-1) 7.25±2.22 5.37±3.39 3.505 < 0.001 血Ca/(mmol·L-1) 2.81±0.41 2.68±0.35 1.756 0.082 ESR/(mm·h-1) 26.36±6.33 21.57±5.41 4.189 < 0.001 补体C3/(g·L-1) 0.52±0.29 0.61±0.31 1.566 0.120 补体C4/(g·L-1) 0.13±0.08 0.15±0.06 1.445 0.151 表 2 校正混杂因素前后AGR对LN的影响
变量 β Wald P OR 95%CI 下限 上限 AGR≥1.35校正前 -1.629 15.199 < 0.001 0.196 0.086 0.445 AGR≥1.35校正后 -1.291 10.150 0.001 0.275 0.124 0.608 表 3 SLE合并肾功能异常单因素分析
X±S 变量 肾功能异常组(28例) 肾功能正常组(34例) t/χ2 P 年龄/岁 42.07±6.90 43.11±5.74 0.648 0.519 性别(男/女)/例 2/26 5/29 0.877 0.349 病程/月 12.09±6.32 10.78±5.17 0.898 0.373 SLE-DAI 12.01±3.10 8.89±3.45 3.708 < 0.001 实验室指标 A/G≥1.20(是/否)/例 11/17 24/10 6.120 0.013 Hb/(g·L-1) 103.34±16.76 109.26±14.91 1.471 0.147 RDW/fl 47.96±3.98 47.21±3.23 0.819 0.416 CRP/(mg·L-1) 8.51±3.56 6.02±2.21 3.369 0.001 血Ca/(mmol·L-1) 2.90±0.38 2.73±0.34 1.858 0.068 ESR/(mm·h-1) 27.17±6.54 25.69±4.97 1.012 0.316 补体C3/(g·L-1) 0.51±0.29 0.53±0.31 0.260 0.796 补体C4/(g·L-1) 0.12±0.07 0.13±0.08 0.518 0.606 BUN/(mmol·L-1) 14.72±3.28 6.95±2.17 11.170 < 0.001 Cr/(μmol·L-1) 204.56±36.62 82.33±12.79 18.190 < 0.001 ACR/(μg·mg-1) 202.49±39.94 62.55±16.17 18.670 < 0.001 表 4 校正混杂因素前后AGR对肾功能异常的影响
变量 β Wald P OR 95%CI 下限 上限 AGR校正混杂因素前 -1.311 5.896 0.015 0.270 0.094 0.777 AGR校正混杂因素后 -1.163 4.706 0.030 0.313 0.109 0.894 -
[1] 邓胜, 陈键. 血细胞比值、平均血小板体积评估系统性红斑狼疮活动性研究[J]. 临床血液学杂志, 2021, 36(6): 415-418, 422. https://www.cnki.com.cn/Article/CJFDTOTAL-LCXZ202106009.htm
[2] Afzal W, Haghi M, Hasni SA, et al. Lupus hepatitis, more than just elevated liver enzymes[J]. Scand J Rheumatol, 2020, 49(6): 427-433. doi: 10.1080/03009742.2020.1744712
[3] Ma HY, Chen S, Cao WD, et al. Diagnostic value of TWEAK for predicting active lupus nephritis in patients with systemic lupus erythematosus: a systematic review and meta-analysis[J]. Ren Fail, 2021, 43(1): 20-31. doi: 10.1080/0886022X.2020.1853568
[4] 林维, 张卫茹, 李通, 等. 中性粒细胞/淋巴细胞比值与系统性红斑狼疮脏器受累及疾病活动的相关性分析[J]. 中华肾脏病杂志, 2019, 35(3): 191-197.
[5] Liu XR, Qi YY, Zhao YF, et al. Albumin-to-globulin ratio(AGR)as a potential marker of predicting lupus nephritis in Chinese patients with systemic lupus erythematosus[J]. Lupus, 2021, 30(3): 412-420. doi: 10.1177/0961203320981139
[6] Kiriakidou M, Ching CL. Systemic Lupus Erythematosus[J]. Ann Intern Med, 2020, 172(11): ITC81-ITC96. doi: 10.7326/AITC202006020
[7] 李鎛江, 董建华, 潘红霞, 等. 中性粒细胞-淋巴细胞比值与系统性红斑狼疮肾损害的相关性分析[J]. 现代医学, 2021, 49(4): 400-406. doi: 10.3969/j.issn.1671-7562.2021.04.006
[8] 许文荣, 龚道元, 胥文春, 等. 临床基础检验[M]. 北京, 人民卫生出版社, 2019: 161-163.
[9] 梁涛, 张晓宝, 张德太, 等. 3项指标联合检测在糖尿病肾病中的早期诊断价值[J]. 临床血液学杂志, 2019, 32(4): 247-250. https://www.cnki.com.cn/Article/CJFDTOTAL-LCXZ201904002.htm
[10] Wei C, Li T, Xuan X, et al. Serum albumin predicts hyperuricemia in patients with idiopathic membranous nephropathy[J]. Clin Nephrol, 2021, 96(4): 191-198. doi: 10.5414/CN110524
[11] Yu H, Han H, Li J, et al. Alpha-hydroxybutyrate dehydrogenase as a biomarker for predicting systemic lupus erythematosus with liver injury[J]. Int Immunopharmacol, 2019, 77: 105922. doi: 10.1016/j.intimp.2019.105922
[12] Wenderfer SE, Eldin KW. Lupus Nephritis[J]. Pediatr Clin North Am, 2019, 66(1): 87-99. doi: 10.1016/j.pcl.2018.08.007
[13] Wang CM, Deng JH, Mao GF, et al. Serum Amyloid A: A Potential Biomarker Assessing Disease Activity in Systemic Lupus Erythematosus[J]. Med Sci Monit, 2020, 26: e923290.
[14] Littlejohn E, Marder W, Lewis E, et al. The ratio of erythrocyte sedimentation rate to C-reactive protein is useful in distinguishing infection from flare in systemic lupus erythematosus patients presenting with fever[J]. Lupus, 2018, 27(7): 1123-1129. doi: 10.1177/0961203318763732
[15] Toubi E, Vadasz Z. Innate immune-responses and their role in driving autoimmunity[J]. Autoimmun Rev, 2019, 18(3): 306-311. doi: 10.1016/j.autrev.2018.10.005
[16] 周丽, 胡豪飞, 何永成. 中性粒细胞/淋巴细胞比值与狼疮性肾炎肾功能及肾脏预后的关系[J]. 中国中西医结合肾病杂志, 2019, 20(4): 302-306. doi: 10.3969/j.issn.1009-587X.2019.04.007
-




 下载:
下载: