Changes and clinical value of levels of serum LDH, SF and Th17 in patients with myelodysplastic syndromes
-
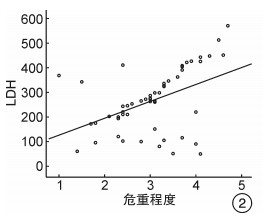
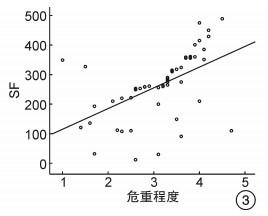
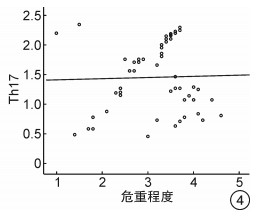
摘要: 目的 研究血清乳酸脱氢酶(LDH)、铁蛋白(SF)以及辅助性T细胞17(Th17)水平变化对骨髓增生异常综合征(MDS)的诊断价值。方法 选取2019年10月至2020年10月收治的53例MDS患者作为观察组, 按照国际预后积分系统(IPSS)的分级标准分为低危组12例, 中危-Ⅰ组14例, 中危-Ⅱ组17例, 高危组10例, 并选择同期进行体检的健康者50例为对照组, 患者入院后抽取空腹状静脉血5 mL, 离心后使用比色法测定LDH水平, 使用化学发光免疫分析法测定SF水平, 使用流式细胞术检测Th17水平。比较观察组各组与对照组间的LDH、SF、Th17水平差异, 分析以上参数与IPSS评分的关系。结果 观察组患者的LDH、SF及Th17百分比均高于对照组(P< 0.05), 随着危险等级升高, 观察组患者的LDH和SF水平上升(P< 0.05), Th17水平在中低危时随着危险等级上升而上升, 高危组Th17水平下降(P< 0.05);LDH、SF、Th17诊断MDS的AUC、敏感度、特异性、临界值分别为0.900、90.63%、90.48%、305.22 U/L;0.839、86.21%、83.33%、299.98 μg/L;0.843、87.10%、81.82%、1.96%;血清LDH与SF水平与病情危重程度呈正相关(P< 0.05)。结论 MDS患者血清LDH、SF、Th17水平上升, 其水平对MDS的诊断有较高的价值, 病情危重程度随着LDH、SF水平的升高而加重, Th17水平与病情危重程度无明显相关性。Abstract: Objective To study the diagnostic value of levels of serum lactate dehydrogenase(LDH), ferritin(SF) and helper T cell 17(Th17) on myelodysplastic syndromes(MDS).Methods A total of 53 MDS patients admitted to the hospital between October 2019 and October 2020 were selected as observation group, and divided into low-risk group(12 cases), intermediate-risk I group(14 cases), intermediate-risk II group(17 cases) and high-risk group(10 cases) according to the International Prognostic Scoring System(IPSS) grading standards. Another 50 healthy people who underwent physical examination in the hospital during the same period were selected as control group. After admission, 5 mL of fasting venous blood were extracted from the patients. After centrifugation, the level of LDH was determined by colorimetry, and the level of SF was measured by chemiluminescence immunoassay, and the level of Th17 was detected by flow cytometry. The differences in the levels of LDH, SF and Th17 were compared between observation group and control group, and the relationship between the above parameters and IPSS score was analyzed.Results The LDH, SF and percentage of Th17 in observation group were higher than those in control group(P< 0.05). As the risk level increased, the levels of LDH and SF in observation group were increased(P< 0.05), and Th17 level was increased in intermediate-risk group and low-risk group and decreased in high-risk group(P< 0.05) with the increase of risk level. The AUC, sensitivity, specificity and cutoff value of diagnosis of MDS were 0.900, 90.63%, 90.48% and 305.22 U/L of LDH, and were 0.839, 86.21%, 83.33% and 299.98 μg/L of SF, and were 0.843, 87.10%, 81.82% and 1.96% of Th17. The levels of LDH and SF were positively correlated with the severity of disease(P< 0.05).Conclusion The levels of serum LDH, SF and Th17 in MDS patients are increased, and their levels are of high value for the diagnosis of MDS. The severity of disease aggravates with the increases of LDH and SF, and the level of Th17 is not obviously correlated with the severity of disease.
-
Key words:
- myelodysplastic syndromes /
- lactate dehydrogenase /
- ferritin /
- helper T cell 17 /
- diagnosis
-

-
表 1 2组患者血清LDH、SF和Th17水平比较
X±S 组别 例数 LDH/(U·L-1) SF/(μg·L-1) Th17/% 观察组 53 262.44±71.37 278.48±82.63 2.05±0.62 对照组 50 148.62±45.23 147.72±41.56 1.32±0.41 t 9.602 10.052 7.004 P < 0.01 < 0.01 < 0.01 表 2 MDS各组患者血清LDH、SF与Th17水平比较
X±S 组别 例数 LDH/(U·L-1) SF/(μg·L-1) Th17/% 低危组 12 182.45±24.38 258.54±79.06 1.35±0.21 中危-Ⅰ组 14 217.32±30.59 462.32±101.48 2.26±0.52 中危-Ⅱ组 17 344.73±66.24 621.28±139.84 2.85±0.76 高危组 10 719.41±112.75 705.69±161.93 1.02±0.29 F 154.132 41.026 45.847 P < 0.01 < 0.01 < 0.01 表 3 LDH、SF与Th17对MDS的诊断价值
项目 AUC 灵敏度/% 特异性/% 临界值 95%CI 约登指数 P LDH 0.900 90.63 90.48 305.22 0.787~0.966 0.811 < 0.01 SF 0.839 86.21 83.33 299.98 0.712~0.926 0.695 < 0.01 Th17 0.843 87.10 81.82 1.96 0.717~0.928 0.689 < 0.01 -
[1] 陈丽娟, 吴亚兵, 韩少玲. 血清SF、LDH及骨髓细胞形态学表现在骨髓增生异常综合征和巨幼细胞性贫血鉴别诊断中的临床意义[J]. 标记免疫分析与临床, 2018, 25(11): 1654-1657. https://www.cnki.com.cn/Article/CJFDTOTAL-BJMY201811021.htm
[2] 杨洁, 杨永宾, 李杰, 等. 可溶性CD44 s、SF、LDH在鉴别巨幼细胞贫血和骨髓增生异常综合征中的意义[J]. 河北医药, 2016, 38(24): 3773-3775. doi: 10.3969/j.issn.1002-7386.2016.24.026
[3] 陈婉淑, 张梦露, 韩冰. 骨髓增生异常综合征和急性髓系白血病的基因突变比较[J]. 中华血液学杂志, 2021, 42(2): 171-176. https://www.cnki.com.cn/Article/CJFDTOTAL-HNYK202003010.htm
[4] 郑丽坤, 成雪, 高庆峰, 等. 骨髓增生异常综合征患者血清乳酸脱氢酶水平动态变化及其意义[J]. 山东医药, 2018, 58(15): 73-75. doi: 10.3969/j.issn.1002-266X.2018.15.022
[5] 高锦程, 洪珞珈. 骨髓增生异常综合征的研究进展[J]. 临床血液学杂志, 2018, 31(1): 66-70. https://www.cnki.com.cn/Article/CJFDTOTAL-LCXZ201801020.htm
[6] 陈春平, 王娟, 徐徐. 骨髓增生异常综合征患者血清LDH、β2-MG、铁蛋白、维生素B12变化与预后的关系[J]. 标记免疫分析与临床, 2021, 28(4): 647-650, 691. https://www.cnki.com.cn/Article/CJFDTOTAL-BJMY202104026.htm
[7] 李康保, 李庆山, 程艳华, 等. 辅助性T细胞17在铁过载骨髓增生异常综合征中的临床意义[J]. 中华内科杂志, 2019, 58(6): 419-422. doi: 10.3760/cma.j.issn.0578-1426.2019.06.004
[8] 蒋显勇, 陈晓利, 梁庄严, 等. SF、Vit B12和FA对骨髓增生异常综合征3种亚型的价值[J]. 检验医学, 2018, 33(7): 581-585. doi: 10.3969/j.issn.1673-8640.2018.07.001
[9] 谢春艳, 胡景玉, 多亚莉, 等. MCV、RDW、LDH及FISH联合检测对骨髓增生异常综合征的诊断价值[J]. 海南医学, 2017, 28(15): 2484-2485. doi: 10.3969/j.issn.1003-6350.2017.15.022
[10] 中华医学会血液学分会. 骨髓增生异常综合征中国诊断与治疗指南(2019年版)[J]. 中华血液学杂志, 2019, 40(2): 89-97.
[11] 丁宇斌, 唐玉凤, 唐旭东. 骨髓增生异常综合征基因突变的研究进展[J]. 临床与实验病理学杂志, 2021, 37(2): 198-201. https://www.cnki.com.cn/Article/CJFDTOTAL-LSBL202102021.htm
[12] 岳虹, 张静妮. 血清LDH、CA153、FA和Hcy水平检测在MA和MDS临床鉴别诊断中的作用研究[J]. 检验医学与临床, 2020, 17(19): 2862-2865. doi: 10.3969/j.issn.1672-9455.2020.19.033
[13] 袁舟亮, 胡安群, 刘海燕, 等. 血清中部分生化指标检测对恶性血液病诊断的意义[J]. 安徽医药, 2019, 23(2): 304-307. doi: 10.3969/j.issn.1009-6469.2019.02.025
[14] 刘元军, 青胜兰, 徐锋, 等. 血清LDH、可溶性CD44、SF在骨髓增生异常综合征和急性髓系白血病诊断中的临床意义[J]. 标记免疫分析与临床, 2018, 25(8): 1137-1141. https://www.cnki.com.cn/Article/CJFDTOTAL-BJMY201808014.htm
[15] 杨园, 安田丽, 赵丽. 移植前高血清铁蛋白对急性髓系白血病及骨髓增生异常综合征预后影响研究新进展[J]. 临床血液学杂志, 2019, 32(5): 400-403. https://www.cnki.com.cn/Article/CJFDTOTAL-LCXZ201905019.htm
[16] 程家凤, 王晓培, 郑茜茜, 等. 骨髓增生异常综合征血清铁蛋白检测的临床意义[J]. 白血病·淋巴瘤, 2019, 28(3): 160-163. https://www.cnki.com.cn/Article/CJFDTOTAL-TJIY200404018.htm
[17] 李静. Th17细胞在骨髓增生异常综合征发病机制中的作用[D]. 天津: 天津医科大学, 2016.
[18] 郑丽坤, 成雪, 高庆峰, 等. 骨髓增生异常综合征患者血清乳酸脱氢酶水平动态变化及其意义[J]. 山东医药, 2018, 58(15): 73-75. doi: 10.3969/j.issn.1002-266X.2018.15.022
[19] 于晓倩, 孙龙, 梁超, 等. 以多发皮肤暗红色斑块为首发症状的骨髓增生异常综合征1例[J]. 精准医学杂志, 2021, 36(1): 92-94. https://www.cnki.com.cn/Article/CJFDTOTAL-SPAN202101021.htm
[20] 李莉, 毕庆庆, 郑金菊, 等. 铁蛋白、叶酸和维生素B 12检测在骨髓增生异常综合征诊疗中的价值[J]. 国际检验医学杂志, 2018, 39(18): 2256-2258. doi: 10.3969/j.issn.1673-4130.2018.18.015
-





 下载:
下载: