Cause analysis of estimation error of blood loss in intractable postpartum hemorrhage
-
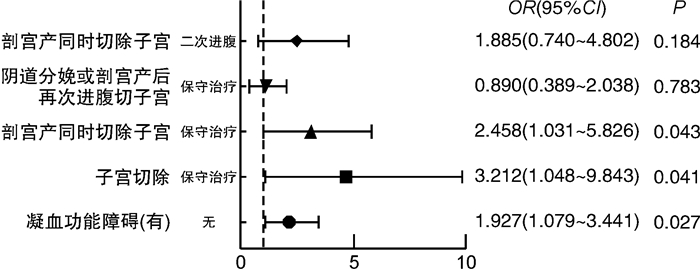
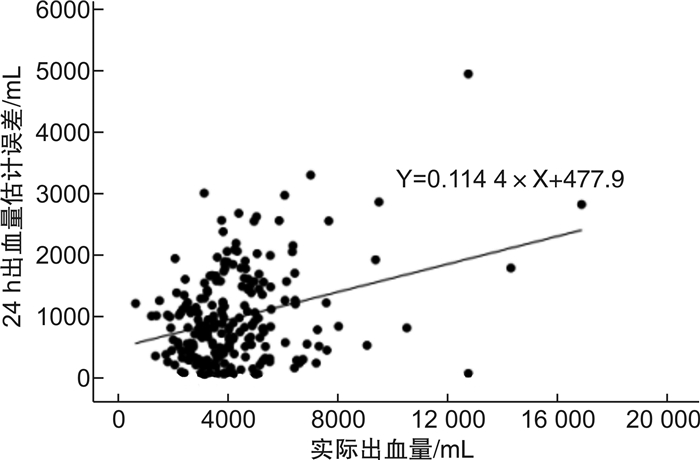
摘要: 目的 分析难治性产后出血的出血量估计误差的原因,为临床准确估计出血量提供依据。方法 分析2008年1月至2019年12月分娩的发生难治性产后出血的产妇228例。根据产后24 h出血量误差是否超过产妇血容量的20%分为2组:A组(出血量估计误差 < 产妇血容量的20%)133例,B组(出血量估计误差≥产妇血容量的20%)95例。对影响出血量估计误差的各种可疑因素进行单因素分析及二元logistic回归分析。结果 凝血功能障碍(是/否)、子宫切除/保守治疗这2类因素,A组与B组比较差异有统计学意义(P< 0.05)。结论 对于难治性产后出血的患者,当其出现凝血功能障碍、需切除子宫才能有效止血,特别是行剖宫产需同时切除子宫时,出血量的估计可能严重不足,临床上应对这部分患者更加重视,多方面综合评估其出血量。Abstract: Objective To analyze the reasons for estimation error of intractable postpartum hemorrhage(PPH) and provide a reasonable estimate of the blood loss in practice.Methods A total of 228 cases of intractable PPH were selected from January 2008 to December 2019 in the Affiliated Obstetrics and Gynecology Hospital of Nanjing Medical University. Two groups were divided according to the estimation error of 24-hour blood loss: group A(estimation error < 20% of maternal blood volume, 133 cases) and group B(estimation error≥20% of maternal blood volume, 95 cases). Univariate analysis and binary logistic regression analysis were used to analyze the suspicious factors influencing the estimation error of blood loss.Results Coagulation dysfunction(yes/no) and hysterectomy/conservative treatment were significantly different between group A and group B(P< 0.05).Conclusion For patients with intractable PPH, when coagulation dysfunction occurs and hysterectomy is needed to effectively stop bleeding, especially when cesarean section is performed at the same time, the estimation of blood loss may be seriously insufficient. In clinical practice, comprehensive evaluation should be considered and more attention should be paid to these patients.
-
Key words:
- intractable postpartum hemorrhage /
- estimation error of blood loss /
- cause
-

-
表 1 2组产妇的一般情况分析
X ±S 变量 A组(133例) B组(95例) t 年龄/岁 32.87±4.610 32.46±5.00 0.637 身高/cm 161.14±4.51 160.70±5.08 0.695 体重/kg 71.70±8.49 71.18±8.16 0.460 分娩孕周 36.52±3.75 36.26±3.75 0.529 表 2 影响难治性产后出血患者出血量估计误差的单因素分析
例(%) 变量 A组(133例) B组(95例) χ2 P 分娩方式 0.177 0.674 剖宫产 112(84.2) 78(82.1) 阴道分娩 21(15.8) 17(17.9) 凝血功能障碍 6.816 0.009 是 43(32.3) 47(49.5) 否 90(67.7) 48(50.5) 隐性出血 0.014 0.906 有 23(17.3) 17(17.9) 无 110(82.7) 78(82.1) 胎盘异常 0.008 0.927 是 79(59.4) 57(60.0) 否 54(40.6) 38(40.0) 外科手术/介入 3.352 0.187 介入 82(61.7) 47(49.5) 外科手术+介入 12(9.0) 11(11.6) 外科手术 39(29.3) 37(38.9) 外科手术方式 4.44 0.035 子宫切除 34(25.6) 39(41.1) 保守治疗 14(10.5) 5(5.3) 子宫切除进腹次数 1.779 0.182 剖宫产并同时切除 13(9.8) 21(22.1) 分娩或剖宫产后再次进腹切除 21(15.8) 18(18.9) -
[1] 刘兴会, 张力, 张静. 《产后出血预防与处理指南(草案)》(2009)及《产后出血预防与处理指南(2014年版)》解读[J]. 中华妇幼临床医学杂志(电子版), 2015, 11(4): 433-447. doi: 10.3877/cma.j.issn.1673-5250.2015.04.002
[2] Bienstock JL, Eke AC, Hueppchen NA. Postpartum Hemorrhage[J]. N Engl J Med, 2021, 384(17): 1635-1645. doi: 10.1056/NEJMra1513247
[3] 中华医学会妇产科学分会产科学组. 产后出血预防与处理指南(2014)[J]. 中华妇产科杂志, 2014, 49(9): 641-646. doi: 10.3760/cma.j.issn.0529-567x.2014.09.001
[4] 谢幸, 孔北华, 段涛. 妇产科学[M]. 9版. 北京: 人民卫生出版社, 2018: 204.
[5] 于布为, 王国林, 王泉云, 等. 临床麻醉监测指南(2014)[M]//中华医学会麻醉学分会. 2014版中国麻醉学指南与专家共识. 北京: 人民卫生出版社, 2015: 20.
[6] Wang F, Lu N, Weng X, et al. Measurement of postpartum blood loss using a new two-set liquid collection bag for vaginal delivery: A prospective, randomized, case control study[J]. Medicine(Baltimore), 2021, 100(19): e25906.
[7] Kreutziger J, Puchner P, Schmid S, et al. Accuracy of training blood volume quantification using a visual estimation tool[J]. World J Emerg Med, 2021, 12(3): 174-178. doi: 10.5847/wjem.j.1920-8642.2021.03.002
[8] Konig G, Waters JH, Hsieh E, et al. In Vitro Evaluation of a Novel Image Processing Device to Estimate Surgical Blood Loss in Suction Canisters[J]. Anesth Analg, 2018, 126(2): 621-628. doi: 10.1213/ANE.0000000000002692
[9] 黄丹. 不同分娩方式在产后出血量估计上的差异[J]. 中西医结合心血管病电子杂志, 2018, 6(33): 34-34. doi: 10.3969/j.issn.2095-6681.2018.33.022
[10] 沈玲玉, 陈婧, 张兰, 等. 休克指数对产后出血输血治疗和入住ICU预测价值的研究[J]. 临床血液学杂志, 2022, 35(2): 103-107. https://www.cnki.com.cn/Article/CJFDTOTAL-LCXZ202202005.htm
-




 下载:
下载: