-
摘要: 目的 研究认识血小板单采活化的特点,分析单采血小板活化的相关因素,识别验证对单采过程诱导活化敏感个体,合理处置,减少血小板输注无效(PTR)发生频率。方法 随机收集台州市中心血站的单采血小板样本,在下机后30 min内用PAC-1、CD62p荧光抗体标记并用1%甲醛固定,随后及时上机检测活化百分率,同时收集该样本对应献血者的体检、献血前筛查、单采数据。对收集的各类数据进行相应的统计分析。结果 PAC-1、CD62p阳性表达率分别为(35.3±23.5)%、(2.7±2.9)%,两者配对t检验统计分析显示两者的差异有统计学意义(t=18.853,P< 0.01);相关分析显示,PAC-1、CD62p的阳性表达率分别与HGB和HCT呈负相关(r=-0.257,P=0.001;r=-0.177,P=0.021;r=-0.262,P=0.001;r=-0.187,P=0.015),与献血者年龄呈正相关(r=0.237,P=0.002;r=0.242,P=0.002);以献血者为自变量、PAC-1阳性表达率为因变量的单因素方差分析,差异有统计学意义。结论 单采活化是以GPⅡbⅢa构象改变暴露出纤维蛋白原结合位点为特征的血小板早期活化形式为主,而α颗粒膜融合表达CD62p的晚期活化则处于较低的水平,且这2种活化形式存在正相关关系(r=0.503,P< 0.01);与活化百分率相关指标可以为献血者的筛查及单采血小板产品的合理处置提供参考;血小板单采PAC-1阳性表达存在个体差异,是献血者固有的血小板反应特性。Abstract: Objective To study and understand the characteristics of platelet apheresis activation, analyze the related factors of platelet activation during apheresis, identify and verify individuals who were sensitive to activation induced by apheresis, and handle them rationally to reduce the frequency of platelet transfusion failure(PTR).Methods Apheresis platelet samples from this station were randomly collected, labeled with PAC-1 and CD62p fluorescent antibodies and fixed with 1% formaldehyde within half an hour after getting off the machine, and then the activation percentage was detected on the machine in time, and the medical examination data, pre-donation screening data and apheresis data of the blood donors corresponding to the samples was collected. The collected data was statistically analyzed.Results The positive expression rates of PAC-1 and CD62p were (35.3±23.5)% and (2.7±2.9)%, respectively. The paired t-test statistical analysis showed that the difference was statistically significant(t=18.853,P< 0.01); correlation analysis showed that the positive expression rates of PAC-1 and CD62p were negatively correlated with HGB and HCT, respectively(r=-0.257,P=0.001;r=-0.177,P=0.021;r=-0.262,P=0.001;r=-0.187,P=0.015), positively correlated with the age of blood donors(r=0.237,P=0.002; r=0.242,P=0.002); one-way ANOVA with blood donors as the independent variable PAC-1 positive expression rate as the dependent variable. It was statistically significant.Conclusion Apheresis activation is mainly the early activation form of platelets characterized by the conformational change of GPⅡb Ⅲa exposing the fibrinogen binding site, while the late activation of α-granule membrane fusion expressing CD62p is at a lower level, and there is a positive correlation between the two activation forms(r=0.503,P< 0.01); the index related to the activation percentage can be used for the screening of blood donors and provide reference for the reasonable disposal of apheresis platelet product.There were individual differences in the positive expression of PAC-1 in platelet apheresis, which might be the inherent platelet reaction characteristic of blood donors.
-
Key words:
- apheresis platelet /
- platelet activation /
- related factors /
- individual differences
-

-
表 1 高反应组阳性表达率
% 献血者 样本1 样本2 样本3 PAC-1 CD62p PAC-1 CD62p PAC-1 CD62p A 79.9 1.1 72.8 4.0 77.8 1.6 B 90.1 4.6 79.7 5.5 68.6 6.9 C 87.6 6.1 68.8 1.0 D 81.9 2.3 71.0 1.8 E 77.5 1.0 39.2 0.7 F 72.1 3.6 47.4 2.2 表 2 中反应组阳性表达率
% 献血者 样本1 样本2 PAC-1 CD62p PAC-1 CD62p N 54.0 2.6 22.3 0.5 O 21.4 0.6 52.1 7.1 P 45.7 2.7 14.8 0.9 Q 57.4 0.5 46.9 2.8 R 16.7 1.2 41.2 3.3 表 3 低反应组阳性表达率
% 献血者 样本1 样本2 PAC-1 CD62p PAC-1 CD62p G 17.9 1.2 5.2 0.7 H 29.1 1.2 9.7 0.2 I 28.1 3.0 1.9 0.3 J 35.2 2.4 26.4 1.8 K 24.5 1.2 2.9 2.4 L 13.8 0.3 6.0 0.8 M 27.4 1.0 8.4 0.7 表 4 Spearman双变量相关分析结果
献血者 PAC-1 CD62p r P r P CD62P 0.503 0 身高 -0.121 0.116 -0.129 0.093 体重 -0.066 0.392 -0.026 0.739 脉搏 -0.125 0.105 0.032 0.683 收缩压 -0.001 0.986 0.132 0.086 舒张压 -0.064 0.406 0.038 0.624 年龄 0.237 0.002 0.242 0.002 总次数 -0.049 0.526 -0.020 0.793 间隔 0.031 0.689 0.093 0.226 WBC 0.125 0.105 0.048 0.538 HCT -0.262 0.001 -0.187 0.015 HGB -0.257 0.001 -0.177 0.021 ALT -0.038 0.623 0.068 0.375 PLT -0.051 0.510 0.029 0.705 循环血量 -0.229 0.003 0.041 0.599 抗凝剂 -0.229 0.003 0.030 0.698 总次数为血小板捐献者捐献血小板总次数;间隔为本次捐献与上次血小板捐献间隔天数。 -
[1] 中国医师协会输血科医师分会, 中华医学会临床输血学分会. 血小板抗体检测专家共识[J]. 临床输血与检验, 2020, 22(2): 1-5. https://www.cnki.com.cn/Article/CJFDTOTAL-LSXY202001001.htm
[2] Hughes DL, Evans G, Metcalfe P, et al. Tracking and characterisation of transfused platelets by two colour, whole blood flow cytometry[J]. Br J Haematol, 2005, 130(5): 791-794. doi: 10.1111/j.1365-2141.2005.05671.x
[3] Murphy S. Utility of in vitro tests in predicting the in vivo viability of stored PLTs[J]. Transfusion, 2004, 44(4): 618-619. doi: 10.1111/j.1537-2995.2004.00355.x
[4] 周明, 陈洋, 王敏, 等. 机采血小板储存损伤对临床疗效的影响[J]. 临床输血与检验, 2019, 21(2): 129-133. doi: 10.3969/j.issn.1671-2587.2019.02.005
[5] Shattil SJ, Motulsky HJ, Insel PA, et al. Expression of fibrinogen receptors during activation and subsequent desensitization of human platelets by epinephrine[J]. Blood, 1986, 68(6): 1224-1231. doi: 10.1182/blood.V68.6.1224.1224
[6] 傅晓岚, 陈兆珍, 成晓玲, 等. 流式细胞仪双色术检测机采血小板活化方法[J]. 第三军医大学学报, 2003, (18): 1672-1673. doi: 10.3321/j.issn:1000-5404.2003.18.026
[7] 姚勇, 张欢欢, 孙振超, 等. 3种血细胞分离机采集血小板活化和功能的分析[J]. 临床血液学杂志, 2021, 34(2): 127-129. https://www.cnki.com.cn/Article/CJFDTOTAL-LCXZ202102013.htm
[8] 夏薇, 陈婷梅, 王宵霞. 临床血液学检验技术[M]. 北京: 人民卫生出版社, 2018: 46-47.
[9] 山媛, 胡军, 赵瑞, 等. PAC-1、CD62P水平在早期诊治和预测脑梗死病情程度中的价值[J]. 中华保健医学杂志, 2019, 21(6): 562-564. https://www.cnki.com.cn/Article/CJFDTOTAL-JFJB201906029.htm
[10] 钟淑萍, 李学刚, 何志国, 等. 系统性红斑狼疮患者血小板PAC-1和CD62P表达的研究[J]. 新医学, 2013, 44(11): 779-782. doi: 10.3969/g.issn.0253-9802.2013.11.012
[11] 李勇, 李一. 实用血小板免疫生物学[M]. 北京: 科学技术出版社, 2019: 254-255.
[12] Yee DL, Sun CW, Bergeron AL, et al. Aggregometry detects platelet hyperreactivity in healthy individuals[J]. Blood, 2005, 106(8): 2723-2729.
[13] Garner SF, Jones CI, Stephens J, et al. Apheresis donors and platelet function: inherent platelet responsiveness influences platelet quality[J]. Transfusion, 2008, 48(4): 673-680.
[14] Fontana P, Dupont A, Gandrille S, et al. Adenosine diphosphate-induced platelet aggregation is associated with P2Y12 gene sequence variations in healthy subjects[J]. Circulation, 2003, 108(8): 989-995.
[15] Metcalfe P, Williamson LM, Reutelingsperger CP, et al. Activation during preparation of therapeutic platelets affects deterioration during storage: a comparative flow cytometric study of different production methods[J]. Br J Haematol, 1997, 98(1): 86-95.
-

| 引用本文: | 张开文, 潘洁, 杨文萍, 等. 血小板单采活化及个体差异[J]. 临床血液学杂志, 2022, 35(10): 735-738. doi: 10.13201/j.issn.1004-2806.2022.10.010 |
| Citation: | ZHANG Kaiwen, PAN Jie, YANG Wenping, et al. Platelet apheresis activation and individual differences[J]. J Clin Hematol, 2022, 35(10): 735-738. doi: 10.13201/j.issn.1004-2806.2022.10.010 |
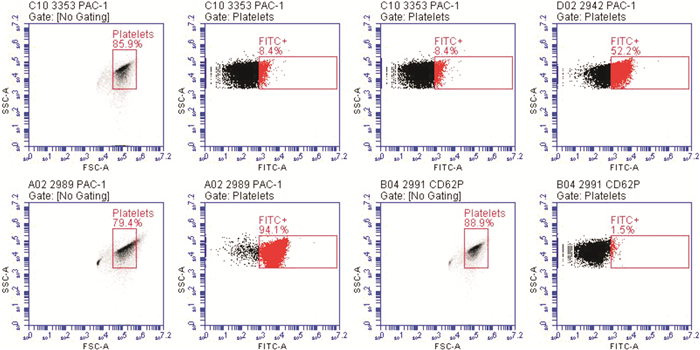
- Figure 1.



 下载:
下载: