Prognostic analysis of preoperative albumin-to-alkaline phosphatase ratio in patients with colorectal cancer undergoing radical surgery
-
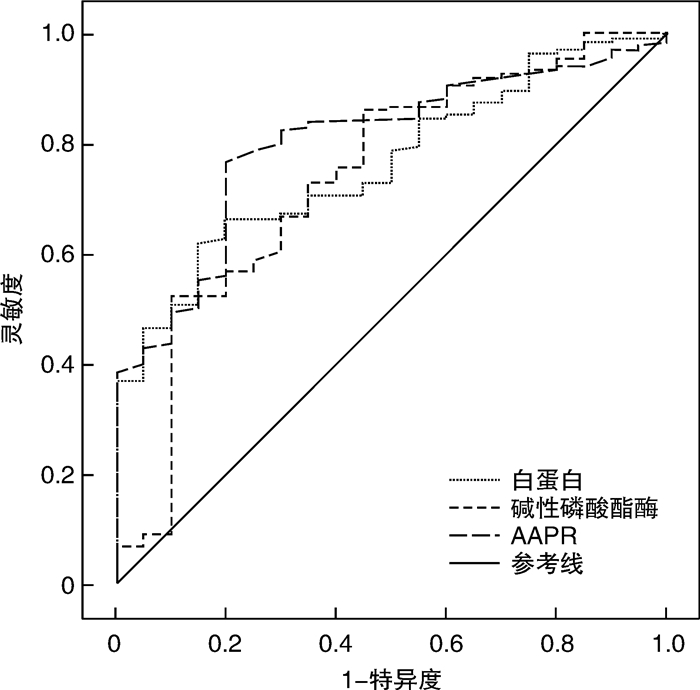
摘要: 目的 分析术前白蛋白与碱性磷酸酶比值(AAPR)对结直肠癌根治术患者预后的预测价值。方法 选取南通市第一人民医院2019年1月—2021年12月收治的162例结直肠癌患者作为研究对象,所有患者均行结直肠癌根治术治疗,术前检测白蛋白、碱性磷酸酶水平并计算AAPR,术后对患者进行为期1年的跟踪随访,以病灶复发或转移作为随访终点事件,评估患者预后情况。采用Cox回归分析检验术前AAPR对结直肠癌根治术患者预后的影响,绘制受试者工作特征(ROC)曲线,以曲线下面积(AUC)检验术前AAPR对结直肠癌根治术患者预后的预测价值。结果 随访期间共有6例患者失访,最终156例患者进入本次研究。156例患者中预后不良20例,占12.82%。不同预后结直肠癌根治术患者TNM分期、分化程度、肿瘤直径、白蛋白、碱性磷酸酶、AAPR比较,差异有统计学意义(P < 0.05)。Cox回归分析显示,TNM分期为Ⅲ期、低分化程度、肿瘤直径≥5 cm、白蛋白水平低、碱性磷酸酶水平高、AAPR低是结直肠癌根治术患者预后不良的影响因素(P < 0.05)。ROC曲线分析显示,白蛋白、碱性磷酸酶、AAPR预测结直肠癌根治术患者预后的AUC分别为0.763、0.737、0.802,其中AAPR预测价值最佳。结论 术前AAPR是影响结直肠癌根治术患者预后的重要因素,且术前AAPR对结直肠癌根治术患者预后具有较高的预测价值。Abstract: Objective To analyze the prognostic value of preoperative albumin-to-alkaline phosphatase ratio(AAPR) in patients with colorectal cancer undergoing radical surgery.Methods A total of 162 patients with colorectal cancer admitted to Nantong First People's Hospital from January 2019 to December 2021 were included as the study subjects. All patients were treated with radical resection of colorectal cancer. The levels of albumin and alkaline phosphatase were measured before operation and AAPR was calculated. The patients were followed up for 1 year after operation, and the recurrence or metastasis of the lesion was taken as the end point of follow-up to evaluate the prognosis of the patients. Cox regression analysis was used to test the influence of preoperative AAPR on the prognosis of patients with colorectal cancer undergoing radical surgery, and the receiver operating characteristic curve(ROC) of subjects was drawn. The area under the curve(AUC) was used to test the predictive value of preoperative AAPR on the prognosis of the patients with colorectal cancer undergoing radical surgery.Results A total of 6 patients were lost during the follow-up period, and 156 patients finally entered the study. Among 156 patients, 20 cases had poor prognosis, accounting for 12.82%. There were statistical significant differences in TNM stage, differentiation degree, tumor diameter, albumin, alkaline phosphatase and AAPR among the patients with different prognosis after radical resection of colorectal cancer(P < 0.05). Cox regression analysis showed that TNM stage Ⅲ, low differentiation, tumor diameter≥5 cm, low albumin level, high alkaline phosphatase level and low AAPR were the influencing factors of poor prognosis in the patients with colorectal cancer after radical surgery(P < 0.05). ROC curve analysis showed that the AUC of albumin, alkaline phosphatase and AAPR in predicting the prognosis of the patients with colorectal cancer after radical surgery were 0.763, 0.737 and 0.802, respectively, of which AAPR was the best predictor.Conclusion Preoperative AAPR might be an important factor affecting the prognosis of patients with colorectal cancer after radical surgery, and preoperative AAPR might have a high predictive value for the prognosis of patients with colorectal cancer after radical surgery.
-
Key words:
- colorectal cancer /
- albumin /
- alkaline phosphatase /
- prognosis
-

-
表 1 基线资料比较
例(%) 资料 预后不良(n=20) 预后良好(n=136) Z/χ2 P 资料 预后不良(n=20) 预后良好(n=136) Z/χ2 P 性别 0.120 0.729 组织学分型 1.335 0.248 男 12(60.00) 76(55.88) 腺癌 15(75.00) 119(87.50) 女 8(40.00) 60(44.12) 腺鳞癌 5(25.00) 17(12.50) 年龄/岁 1.243 0.265 TNM分期 6.712 0.010 ≥60 11(55.00) 92(67.65) Ⅱ期 3(15.00) 62(45.59) <60 9(45.00) 44(32.35) Ⅲ期 17(85.00) 74(54.41) 疾病类型 0.047 0.829 肿瘤直径/cm 4.473 0.034 结肠癌 13(65.00) 85(62.50) ≥5 9(45.00) 28(20.59) 直肠癌 7(35.00) 51(37.50) <5 11(55.00) 108(79.41) 分化程度 2.174 0.030 合并症 高分化 5(25.00) 64(47.06) 高血压 4(20.00) 25(18.38) 0.018 0.893 中分化 5(25.00) 35(25.74) 糖尿病 3(15.00) 20(14.49) 0.092 0.762 低分化 10(50.00) 37(27.20) 冠心病 3(15.00) 14(10.29) 0.061 0.805 表 2 实验室指标比较
X±S 指标 预后不良(n=20) 预后良好(n=136) t P 谷丙转氨酶/(U/L) 30.56±3.85 29.46±4.02 1.137 0.257 谷草转氨酶/(U/L) 28.75±3.57 28.99±3.64 0.265 0.791 肌酐/(μmol/L) 75.84±8.02 76.33±7.85 0.265 0.792 尿素氮/(mmol/L) 5.16±0.22 5.10±0.26 0.977 0.330 尿酸/(μmol/L) 248.77±23.52 250.09±22.78 0.241 0.810 CA199/(U/mL) 34.58±3.66 33.62±3.77 1.060 0.291 CEA/(ng/mL) 15.64±2.37 14.75±2.34 1.572 0.118 红细胞计数/(×1012/L) 4.86±0.22 4.90±0.20 0.830 0.408 白细胞计数/(×109/L) 6.20±1.02 6.15±1.06 0.160 0.873 血小板计数/(×109/L) 218.83±25.85 220.11±24.78 0.216 0.829 血红蛋白/(g/L) 120.52±15.87 118.75±16.32 0.452 0.652 纤维蛋白原/(g/L) 3.05±0.22 2.98±0.19 1.678 0.095 D-二聚体/(mg/L) 0.28±0.10 0.26±0.08 1.453 0.148 白蛋白/(g/L) 39.65±4.28 44.60±5.02 4.193 < 0.001 碱性磷酸酶/(U/L) 92.21±26.75 71.94±19.30 4.155 < 0.001 AAPR 0.43±0.16 0.62±0.26 3.247 0.001 表 3 自变量赋值与说明
自变量 变量说明 赋值情况 TNM分期 分类变量 Ⅲ期=“1”,Ⅱ期=“0” 分化程度 分类变量 高分化=“1”,中分化=“2”,低分化=“3” 肿瘤直径 分类变量 ≥5 cm=“1”, < 5 cm=“0” 白蛋白 连续变量 - 碱性磷酸酶 连续变量 - AAPR 连续变量 - 表 4 结直肠癌根治术患者预后的影响因素分析
因素 β SE Wald P OR 95%CI TNM分期 2.415 0.996 5.884 0.015 11.189 1.590~78.740 分化程度(以高分化为对照) 中分化 -0.880 0.916 0.992 0.337 0.415 0.069~2.500 低分化 -2.803 1.340 4.373 0.037 0.061 0.004~0.839 肿瘤直径 2.227 1.120 3.956 0.047 9.270 1.033~83.199 白蛋白 -0.218 0.053 16.635 < 0.001 0.804 0.724~0.893 碱性磷酸酶 0.041 0.011 14.857 < 0.001 1.042 1.021~1.064 AAPR -3.818 1.396 7.478 < 0.001 0.022 0.001~0.339 表 5 AAPR对结直肠癌根治术患者预后的预测价值
检验变量 AUC AUC的95%CI P 截断值 特异度 灵敏度 约登指数 白蛋白 0.763 0.671~0.856 < 0.001 41.955 g/L 0.662 0.750 0.412 碱性磷酸酶 0.738 0.613~0.862 0.001 79.065 U/L 0.669 0.700 0.369 AAPR 0.802 0.712~0.892 < 0.001 0.465 0.669 0.800 0.469 -
[1] Braun R, Bruch HP, Keck T, et al. Radical resection of locally recurrent colorectal cancer significantly improves overall survival: a single-center cohort study[J]. Dig Surg, 2019, 36(6): 470-478. doi: 10.1159/000491099
[2] 程莉莉, 王琳, 董颖. 结肠癌中长链非编码RNA LUCAT1水平与患者预后的关系及对结肠癌细胞迁移、侵袭的影响[J]. 临床血液学杂志, 2021, 34(2): 89-92. doi: 10.13201/j.issn.1004-2806.2021.02.003
[3] 郭雅慧, 费素娟. 血浆CLIP4基因甲基化检测与3种血清肿瘤标志物对结直肠癌诊断效果的对比性研究[J]. 中国中西医结合消化杂志, 2022, 30(5): 338-345. https://www.cnki.com.cn/Article/CJFDTOTAL-ZXPW202205007.htm
[4] 蒋永杰, 寇邦国, 杜文龙, 等. 基于术前NLR、LMR、CEA和CA19-9对结肠癌根治术后预后列线图预测模型的构建及评价[J]. 解放军医学杂志, 2022, 47(9): 893-901. https://www.cnki.com.cn/Article/CJFDTOTAL-JFJY202209014.htm
[5] Wang Y, Xiong F, Yang J, et al. Decreased albumin-to-alkaline phosphatase ratio predicted poor survival of resectable gastric cancer patients[J]. J Gastrointest Oncol, 2021, 12(4): 1338-1350. doi: 10.21037/jgo-21-430
[6] Sandfeld-Paulsen B, Aggerholm-Pedersen N, Winther-Larsen A. Pretreatment albumin-to-alkaline phosphatase ratio is a prognostic marker in lung cancer patients: a registry-based study of 7077 lung cancer patients[J]. Cancers(Basel), 2021, 13(23): 6133.
[7] 葛均波, 徐永健, 王辰. 内科学[M]. 9版. 北京: 人民卫生出版社, 2018: 381-382.
[8] 王巧瑜, 温凌, 潘洁, 等. 粪便脱落细胞IKZF1甲基化联合血清CEA、CA50检测对结肠癌的诊断价值分析[J]. 中国中西医结合消化杂志, 2021, 29(12): 899-903. https://www.cnki.com.cn/Article/CJFDTOTAL-ZXPW202112013.htm
[9] Alyabsi M, Sabatin F, Ramadan M, et al. Colorectal cancer survival among Ministry of National Guard-Health Affairs(MNG-HA)population 2009-2017: retrospective study[J]. BMC Cancer, 2021, 21(1): 1-11. doi: 10.1186/s12885-020-07763-8
[10] Pu HJ, Pang XL, Fu JP, et al. Significance of tumor deposits combined with lymph node metastasis in stage Ⅲ colorectal cancer patients: a retrospective multi-center cohort study from China[J]. Int J Colorectal Dis, 2022, 37(6): 1411-1420. doi: 10.1007/s00384-022-04149-z
[11] 李岩, 黄波, 张静. 白蛋白/球蛋白对系统性红斑狼疮肾损害及严重程度预测价值研究[J]. 临床血液学杂志, 2022, 35(4): 268-272. doi: 10.13201/j.issn.1004-2806.2022.04.008
[12] Liu XQ, Li Y, Zhao Q, et al. Albumin-to-alkaline phosphatase ratio: a novel prognostic index for patients with driver mutation-negative advanced non-small cell lung cancer[J]. Clin Respir J, 2021, 15(5): 540-549. doi: 10.1111/crj.13339
[13] 马祎菲, 梁新军, 魏少忠. 炎症与免疫指标在可切除性结直肠癌中的预后价值[J]. 中国癌症杂志, 2021, 31(9): 845-851. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGAZ202109014.htm
[14] 徐明月, 李园, 王有龙, 等. 术后C反应蛋白与白蛋白比值与结直肠癌术后并发症的相关性研究[J]. 中华外科杂志, 2021, 59(2): 144-148. https://cdmd.cnki.com.cn/Article/CDMD-10366-1023604156.htm
[15] Zhang F, Lu SX, Tian MX, et al. Albumin-to-alkaline phosphatase ratio is an independent prognostic indicator in combined hepatocellular and cholangiocarcinoma[J]. J Cancer, 2020, 11(17): 5177-5186.
[16] 吴云, 金汉生. 原发性非小细胞肺癌肺叶切除术后血清白蛋白、碱性磷酸酶表达与预后相关性[J]. 安徽医药, 2022, 26(9): 1874-1878. https://www.cnki.com.cn/Article/CJFDTOTAL-AHYY202209042.htm
[17] 胡康, 谭可, 童卫东, 等. 术后白蛋白下降分数对直肠癌保肛术后并发症及长期预后的预测价值[J]. 第三军医大学学报, 2021, 43(19): 1899-1908. https://www.cnki.com.cn/Article/CJFDTOTAL-DSDX202119010.htm
[18] 宋建宁, 李俊, 杨鋆, 等. 全身免疫炎症评分与结直肠癌临床病理特征的相关性分析[J]. 中华消化外科杂志, 2021, 20(10): 1091-1097.
[19] 陈胜灯, 牟志强, 陈忠垚, 等. 碱性磷酸酶与前白蛋白比值对肝细胞癌根治性切除术后患者预后及并发症的预测价值[J]. 临床肝胆病杂志, 2023, 39(1): 118-127. https://www.cnki.com.cn/Article/CJFDTOTAL-LCGD202301022.htm
[20] Zhang F, Lu SX, Hu KS, et al. Albumin-to-alkaline phosphatase ratio as a predictor of tumor recurrence and prognosis in patients with early-stage hepatocellular carcinoma undergoing radiofrequency ablation as initial therapy[J]. Int J Hyperthermia, 2021, 38(1): 1-10.
[21] 王景林, 刘雪影, 李珀, 等. 不同分期结直肠癌间质病理特征与预后及淋巴结转移的相关性[J]. 肿瘤, 2021, 41(1): 45-56. https://www.cnki.com.cn/Article/CJFDTOTAL-ZZLL202101004.htm
[22] 郑款恒, 钟平, 李峰, 等. 不同T分期结直肠癌发生肝肺转移患者的临床病理特征及预后[J]. 中华实验外科杂志, 2022, 39(4): 710-715.
[23] 岳思宇, 李绍东, 孟闫凯, 等. 双能CT淋巴结特征、临床病理特征预测结直肠癌肿瘤沉积的价值[J]. 临床放射学杂志, 2022, 41(9): 1693-1698. https://www.cnki.com.cn/Article/CJFDTOTAL-LCFS202209018.htm
-




 下载:
下载: