Dynamic changes and clinical significance of lipid metabolism in elderly patients with severe pneumonia before and after oxygen therapy
-
摘要: 目的 探讨高龄重症肺炎(SP)患者氧疗前后脂代谢指标动态变化及临床意义,为SP临床治疗及预后改善提供经验指导。方法 回顾性分析医院2019年1月—2022年9月收治的150例高龄SP氧疗患者的临床资料,依据入院28 d预后情况分为存活组(n=98)与病死组(n=52),收集2组患者临床资料,统计氧疗前(T0)、氧疗1 d(T1)、氧疗3 d(T2)时的脂代谢指标[总胆固醇(TC)、甘油三酯(TG)、高密度脂蛋白胆固醇(HDL-C)、低密度脂蛋白胆固醇(LDL-C)、载脂蛋白A1(ApoA1)]检测参数并计算高龄SP患者氧疗前后脂代谢指标波动情况。结果 病死组T0、T1、T2时血清TC、TG、LDL-C水平均高于存活组,HDL-C、ApoA1水平低于存活组,差异有统计学意义(P < 0.05)。病死组血清TC、TG、HDL-C、LDL-C、ApoA1波动指标均高于存活组,差异有统计学意义(P < 0.05)。经Pearson相关性检验,TC、TG、HDL-C、LDL-C、ApoA1指标之间呈正相关(r>0,P < 0.05)。多因素Cox回归分析结果显示,血清TG波动大是高龄SP患者氧疗期间病死的危险因素(HR>1,P < 0.05);绘制ROC曲线图,血清TC、TG、HDL-C、LDL-C、ApoA1波动指标对高龄SP患者氧疗期间病死评估的AUC均>0.7,评估价值较好。结论 高龄SP患者病死风险与氧疗前后脂代谢指标波动情况有关,氧疗前后脂代谢指标波动较大的患者病死风险更高,且氧疗前后脂代谢波动情况对高龄SP患者病死风险的评估价值较好,可作为临床评估及改善高龄SP患者预后的生物学指标。Abstract: Objective To investigate the dynamic changes and clinical significance of lipid metabolism in elderly patients with severe pneumonia(SP) before and after oxygen therapy, and provide experience guidance for clinical treatment and prognosis improvement of SP.Methods The clinical data of 150 elderly patients treated with SP oxygen therapy in our hospital from January 2019 to September 2022 were retrospectively analyzed. They were divided into survival group(n=98) and death group(n=52) according to the 28 day prognosis after admission. The clinical data of patients in the two groups were collected, and the lipid metabolism indexes (total cholesterol[TC], triglyceride[TG], high-density lipoprotein cholesterol[HDL-C], low-density lipoprotein cholesterol[LDL-C], apolipoprotein A1[ApoA1]) before oxygen therapy(T0), oxygen therapy 1 d(T1), and oxygen therapy 3 d(T2) were counted, and the fluctuation of lipid metabolism indexes before and after oxygen therapy in elderly SP patients was calculated.Results The levels of serum TC, TG and LDL-C at T0, T1 and T2 in the death group were higher than those in the survival group, and the level of HDL-C, ApoA1 was lower than that in the survival group, with a statistical significant difference(P < 0.05). The fluctuation indexes of serum TC, TG, HDL-C, LDL-C, ApoA1 in the death group were higher than those in the survival group, with a statistical significant difference(P < 0.05). Pearson correlation test showed that TC, TG, HDL-C, LDL-C and ApoA1 were positively correlated(r>0, P < 0.05). Multivariate Cox regression analysis showed that large fluctuation of serum TG was a risk factor for death of elderly SP patients during oxygen therapy(HR>1, P < 0.05). The ROC curve was drawn, and the AUC of serum TC, TG, HDL-C, LDL-C, ApoA1 fluctuation indicators for the assessment of mortality of elderly SP patients during oxygen therapy was greater than 0.7, with a good evaluation value.Conclusion The risk of death of elderly SP patients might be related to the fluctuation of lipid metabolism indexes before and after oxygen therapy. Patients with large fluctuations of lipid metabolism indexes before and after oxygen therapy might had a higher risk of death, and the fluctuation of lipid metabolism before and after oxygen therapy might had a good evaluation value for the risk of death of elderly SP patients, which could be used as a biological indicator for clinical evaluation and improving the prognosis of elderly SP patients.
-
Key words:
- severe pneumonia /
- advanced age /
- oxygen therapy /
- lipid metabolism index
-

-
表 1 2组临床资料比较
X±S 项目 存活组(n=98) 病死组(n=52) t P 血清TC水平/(mmol/L) T0 5.56±1.28 7.77±2.44 6.089 < 0.001 T1 5.19±1.16 6.25±1.93 7.036 < 0.001 T2 4.67±0.93 5.16±1.49 2.186 0.032 血清TG水平/(mmol/L) T0 2.12±0.37 3.09±0.58 10.889 < 0.001 T1 1.84±0.16 2.43±0.42 9.626 < 0.001 T2 1.18±0.11 1.75±0.36 10.828 < 0.001 血清HDL-C水平/(mmol/L) T0 2.25±0.53 1.94±0.71 2.862 0.005 T1 2.08±0.39 1.58±0.55 5.851 < 0.001 T2 1.85±0.34 1.29±0.34 9.633 < 0.001 血清LDL-C水平/(mmol/L) T0 3.52±0.45 4.23±0.51 8.526 < 0.001 T1 3.26±0.37 3.84±0.45 8.521 < 0.001 T2 3.05±0.31 3.21±0.44 2.471 0.016 血清ApoA1水平/(g/L) T0 1.35±0.35 1.22±0.36 2.153 0.033 T1 1.29±0.31 0.82±0.19 11.497 < 0.001 T2 1.25±0.25 0.64±0.13 19.175 < 0.001 入院时舒张压/mmHga 92.36±7.49 93.27±7.55 0.708 0.480 入院时收缩压/mmHg 118.66±10.63 120.46±10.72 0.983 0.327 空腹血糖/(mmol/L) 5.12±0.75 5.28±0.81 1.211 0.228 TSH/(μU/mL) 2.28±0.44 2.33±0.36 0.837 0.404 BUN/(mmol/L) 4.55±0.72 4.38±0.67 1.500 0.136 Scr/(μmol/L) 65.87±5.46 65.96±5.71 0.095 0.925 ALT/(U/L) 20.87±3.19 21.07±3.22 0.364 0.716 AST/(U/L) 25.73±3.42 25.69±3.38 0.068 0.946 D-D/(mg/L) 0.15±0.02 0.14±0.04 1.683 0.097 HCT/% 43.55±2.17 43.29±2.21 0.720 0.472 注:a1 mmHg=0.133 kPa。 表 2 2组脂代谢波动指标比较
X±S 项目 存活组(n=98) 病死组(n=52) t P 血清TC波动/(mmol/L) 1.19±0.25 2.27±0.71 8.358 < 0.001 血清TG波动/(mmol/L) 0.22±0.07 0.72±0.28 12.664 < 0.001 血清HDL-C波动/(mmol/L) 0.46±0.15 0.61±0.18 5.742 < 0.001 血清LDL-C波动/(mmol/L) 0.42±0.17 0.62±0.19 6.921 < 0.001 血清ApoA1波动/(g/L) 0.31±0.04 0.35±0.06 3.707 < 0.001 表 3 高龄SP患者脂代谢波动指标间的相关性
指标 TC TG HDL-C LDL-C ApoA1 r P r P r P r P r P TC 0.622 < 0.001 0.408 < 0.001 0.297 < 0.001 0.006 < 0.001 TG 0.622 < 0.001 0.350 < 0.001 0.403 < 0.001 0.263 < 0.001 HDL-C 0.408 < 0.001 0.350 < 0.001 0.183 < 0.001 0.038 < 0.001 LDL-C 0.297 < 0.001 0.403 < 0.001 0.183 < 0.001 0.243 < 0.001 ApoA1 0.006 < 0.001 0.263 < 0.001 0.038 < 0.001 0.243 < 0.001 表 4 脂代谢波动对高龄SP患者氧疗期间病死的多因素Cox回归分析
多因素 β SE Walds P HR 95%CI 血清TC波动 0.181 0.219 0.681 0.409 1.198 0.780~1.842 血清TG波动 2.087 0.557 14.038 < 0.001 8.058 2.705~24.004 血清HDL-C波动 0.896 0.900 0.991 0.320 2.449 0.420~14.289 血清LDL-C波动 1.256 0.670 3.513 0.061 3.510 0.944~13.050 血清ApoA1波动 0.430 2.859 0.023 0.880 1.537 0.006~417.483 表 5 脂代谢波动对高龄SP患者氧疗期间病死的评估效能分析
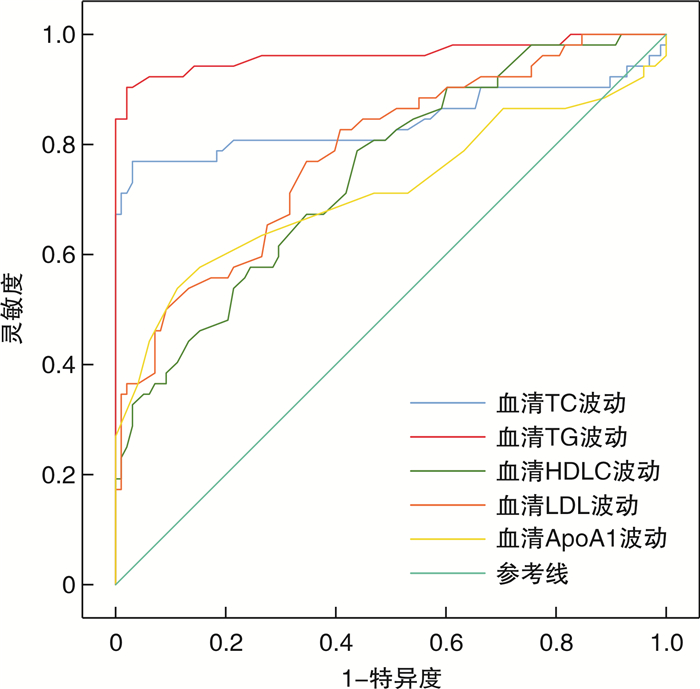
指标 AUC AUC的95%CI SE P 最佳阈值 特异度 灵敏度 约登指数 血清TC波动 0.842 0.756~0.928 0.044 < 0.001 1.575 mmol/L 0.969 0.769 0.738 血清TG波动 0.964 0.925~1.000 0.020 < 0.001 0.365 mmol/L 0.980 0.904 0.884 血清HDL-C波动 0.746 0.650~0.828 0.042 < 0.001 0.485 mmol/L 0.561 0.788 0.349 血清LDL-C波动 0.783 0.705~0.861 0.040 < 0.001 0.505 mmol/L 0.653 0.769 0.422 血清ApoA1波动 0.716 0.618~0.814 0.050 < 0.001 0.345 g/L 0.847 0.577 0.424 -
[1] 姜晓燕. 可溶型Fms样酪氨酸激酶1在重症肺炎预后中的应用价值[J]. 临床血液学杂志, 2020, 33(8): 525-528. https://lcxy.whuhzzs.com/article/doi/10.13201/j.issn.1004-2806-b.2020.08.002
[2] 杨文娜, 张琳. 保守氧疗法在重症肺炎机械通气患者中的应用效果观察[J]. 中华危重病急救医学, 2021, 33(9): 1069-1073. doi: 10.3760/cma.j.cn121430-20210617-00902
[3] 宋剑南. 脂代谢紊乱是当今对人类健康的最大威胁[J]. 中国动脉硬化杂志, 2006, 14(11): 921-924.
[4] 陈永生, 付斌, 郑永先, 等. 血清活化蛋白C及内皮素1和血管细胞黏附分子-1对老年重症肺炎合并呼吸衰竭患者病情进展及预后评估的价值[J]. 临床急诊杂志, 2022, 23(7): 494-497, 509.
[5] 葛均波, 徐永健, 王辰. 内科学[M]. 9版. 北京: 人民卫生出版社, 2018: 41-45.
[6] 张倩, 张俊杰. 老年重症肺炎伴发呼吸衰竭采用无创呼吸机治疗的疗效[J]. 中国老年学杂志, 2020, 40(12): 2547-2549.
[7] Mizgerd JP. Pathogenesis of severe pneumonia: advances and knowledge gaps[J]. Curr Opin Pulm Med, 2017, 23(3): 193-197. doi: 10.1097/MCP.0000000000000365
[8] 岳江, 周勇, 徐华, 等. 糖脂代谢在新型冠状病毒肺炎普通型和重型患者中的特点分析及比较[J]. 上海交通大学学报(医学版), 2021, 41(3): 355-359. doi: 10.3969/j.issn.1674-8115.2021.03.012
[9] Pechous RD. With friends like these: the complex role of neutrophils in the progression of severe pneumonia[J]. Front Cell Infect Microbiol, 2017, 7: 160. doi: 10.3389/fcimb.2017.00160
[10] Schauer AE, Klassert TE, von Lachner C, et al. IL-37 causes excessive inflammation and tissue damage in murine pneumococcal pneumonia[J]. J Innate Immun, 2017, 9(4): 403-418. doi: 10.1159/000469661
[11] 王凡, 陈旭昕, 韩志海. 重症肺炎早期患者外周血T淋巴细胞亚群比例变化及预后预测效能[J]. 山东医药, 2021, 61(27): 32-36. doi: 10.3969/j.issn.1002-266X.2021.27.008
[12] Venet F, Monneret G. Advances in the understanding and treatment of sepsis-induced immunosuppression[J]. Nat Rev Nephrol, 2018, 14(2): 121-137. doi: 10.1038/nrneph.2017.165
[13] 占林兵, 谢波, 华锋, 等. 重症肺炎患者免疫治疗前后免疫功能的变化[J]. 实用医学杂志, 2015, 31(13): 2145-2147. doi: 10.3969/j.issn.1006-5725.2015.13.024
[14] 傅中明, 顾霄. 老年重症肺炎患者细胞炎症因子、凝血功能和肺功能变化及危险因素[J]. 中国老年学杂志, 2018, 38(19): 4663-4666. https://www.cnki.com.cn/Article/CJFDTOTAL-ZLXZ201819023.htm
[15] 张玲, 邵敏, 高磊, 等. 重症肺炎患者病感染原菌情况及相关因子检测分析[J]. 中国病原生物学杂志, 2019, 14(3): 350-353, 357.
-




 下载:
下载: