Expression and clinical value of blood routine parameters in children with mycoplasma pneumonia
-
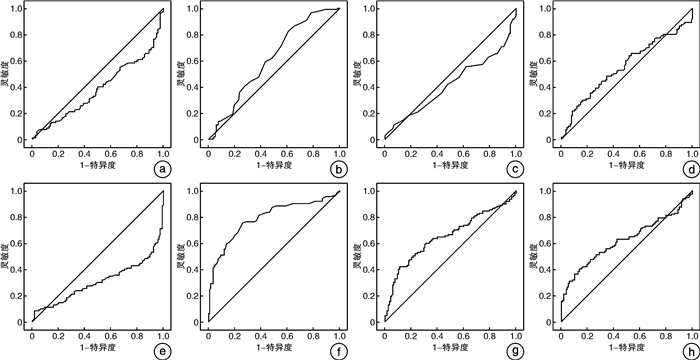
摘要: 目的 分析支原体肺炎患儿血常规检查中血小板相关参数:血小板(PLT)、平均血小板体积(MPV)、血小板比容(PCT)和中性粒细胞(NEUT)、淋巴细胞(LYMPH)、单核细胞(MONO)及中性粒细胞/淋巴细胞比率(NLR)、血小板/淋巴细胞比率(PLR)的表达,探究其与支原体肺炎发生及患儿疾病转归的关联性和临床价值。方法 选取2020年6月—2022年8月收治的支原体肺炎患儿315例作为研究对象,根据患儿临床表现和机体免疫反应进程,结合肺炎支原体抗体水平,将患儿分为3组:感染早期组(110例)、感染中期组(105例)和感染后期组(100例)。同时期的健康体检者118例作为健康对照组。比较健康对照组和支原体肺炎感染各组的血常规相关参数表达水平;采用logistic回归分析法研究血常规相关参数对于支原体肺炎感染的风险和患儿疾病转归的预测价值;绘制受试者工作特征(ROC)曲线,分析评价血常规相关参数对支原体肺炎的诊断价值。结果 支原体肺炎各组与健康对照组之间PLT、MPV、PCT、LYMPH、MONO、NLR、PLR比较差异均有统计学意义(P < 0.05),NEUT比较差异无统计学意义(P>0.05);低水平的LYMPH、高水平的MONO及高水平的PLR状态可以预测支原体肺炎感染的风险,PLT和MPV水平的波动可以较好地预测支原体肺炎患儿疾病转归;MONO最佳临界值为0.465时可辅助诊断支原体肺炎的感染,灵敏度为75.5%,特异度为73.7%。结论 血常规相关参数中MONO、NLR、PLR及LYMPH可作为支原体肺炎辅助诊断的潜在指标,血小板相关参数的监测可以预判机体免疫反应的进程和疾病转归。Abstract: Objective To analyze the expression of platelet-related parameters(PLT, MPV, PCT), neutrophils(NEUT), lymphocytes(LYMPH), monocytes(MONO), neutrophils/lymphocytes ratio(NLR) and platelet-lymphocyte ratio(PLR) in children with mycoplasma pneumonia, and explore the correlation and clinical value of mycoplasma pneumonia with the occurrence and prognosis of children.Methods A total of 315 children with mycoplasma pneumonia admitted from June 2020 to August 2022 were selected as the research objects. According to the level of mycoplasma pneumonia antibody, the children were divided into three groups: early infection group(n=110), middle infection group(n=105) and late infection group(n=100). In the same period, 118 healthy subjects were selected as healthy control group. The expression levels of blood routine parameters were compared between healthy control group and mycoplasma pneumonia infection group. Logistic regression analysis was used to study the predictive value of blood routine parameters for the risk of mycoplasma pneumonia infection and disease outcome in children. ROC curve was drawn to analyze and evaluate the diagnostic value of blood routine parameters for mycoplasma pneumonia.Results There were significant differences in PLT, MPV, PCT, LYMPH, MONO, NLR and PLR between the two groups(P < 0.05), and there was no significant difference in NEUT(P>0.05). The low level of LYMPH, high level of MONO and high level of PLR could predict the risk of mycoplasma pneumonia infection. The fluctuation of PLT and MPV levels could predict the disease outcome of children with mycoplasma pneumonia. The optimal cut-off value of MONO was 0.465. The sensitivity and specificity of MONO were 75.5% and 73.7%, respectively.Conclusion MONO, NLR, PLR and LYMPH could be used as potential indicators for auxiliary diagnosis of mycoplasma pneumonia. The monitoring of platelet related parameters could predict the process of immune response and disease outcome.
-

-
表 1 健康对照组和肺炎支原体感染各组血常规相关参数比较
X±S 项目 健康对照组
(n=118)感染早期组
(n=110)感染中期组
(n=105)感染后期组
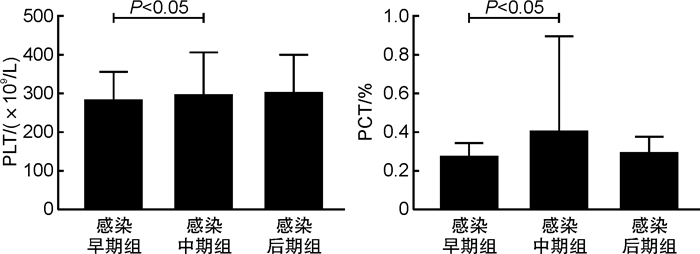
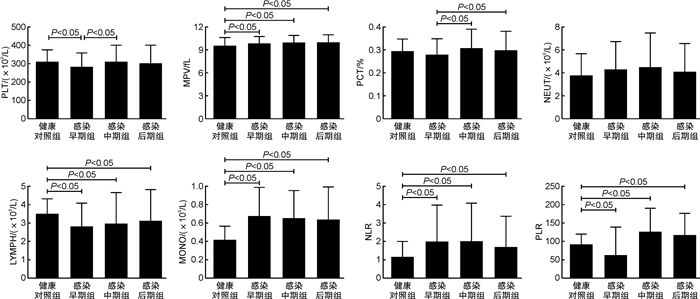
(n=100)P PLT/(×109/L) 312.36±63.35 284.89±74.05 311.8±89.15 304.13±96.91 0.041 MPV/fL 9.60±1.03 9.92±0.85 10.02±0.99 10.04±0.95 0.001 PCT/% 0.30±0.05 0.28±0.07 0.31±0.08 0.30±0.08 0.028 NEUT/(×109/L) 3.81±1.87 4.36±2.39 4.53±2.97 4.14±2.44 0.140 LYMPH/(×109/L) 3.53±0.80 2.83±1.26 2.99±1.67 3.13±1.69 0.001 MONO/(×109/L) 0.42±0.15 0.68±0.31 0.66±0.30 0.64±0.35 < 0.001 NLR 1.18±0.83 2.02±1.87 2.02±2.06 1.71±1.67 < 0.001 PLR 92.71±27.10 122.09±64.74 127.22±63.38 117.74±58.55 < 0.001 表 2 肺炎支原体感染早期组、感染中期组和感染后期组血常规相关参数比较
X±S 项目 感染早期组(n=110) 感染中期组(n=105) 感染后期组(n=100) P PLT/(×109/L) 284.89±74.05 311.80±89.15 304.13±96.91 0.044 MPV/fL 9.92±0.85 10.02±0.99 10.04±0.95 0.613 PCT/% 0.28±0.07 0.31±0.08 0.30±0.08 0.021 NEUT/(×109/L) 4.36±2.39 4.53±2.97 4.14±2.44 0.559 LYMPH/(×109/L) 2.83±1.26 2.99±1.67 3.13±1.69 0.362 MONO/(×109/L) 0.68±0.31 0.66±0.30 0.64±0.35 0.680 NLR 2.02±1.87 2.02±2.06 1.71±1.67 0.381 PLR 122.09±64.74 127.22±63.38 117.74±58.55 0.552 表 3 血常规相关参数与支原体肺炎发生相关性的无序多分类logistic回归分析表
影响因素 感染早期组 感染中期组 感染后期组 OR 95%CI P OR 95%CI P OR 95%CI P PLT 0.975 0.936~1.016 0.231 0.984 0.946~1.024 0.420 1.011 0.973~1.051 0.585 MPV 1.079 0.313~3.716 0.904 1.635 0.482~5.548 0.430 3.716 1.148~12.028 0.028 PCT 371.241 0~1.298×1021 0.786 11.772 0~8.020×1018 0.906 0 0~92 078.223 0.162 NEUT 0.611 0.368~1.015 0.057 0.641 0.389~1.058 0.082 0.645 0.392~1.063 0.085 LYMPH 2.357 1.226~4.53 0.010 2.515 1.322~4.783 0.005 2.830 1.514~5.287 0.001 MONO 24 448.237 2 001.183~298 681.493 <0.001 11 803.056 973.156~143 154.9 <0.001 14 647.711 1 196.835~179 269.054 <0.001 NLR 1.13 0.304~4.208 0.855 1.109 0.300~4.099 0.876 0.939 0.254~3.469 0.925 PLR 1.063 1.03~1.097 <0.001 1.065 1.033~1.099 <0.001 1.070 1.037~1.103 <0.001 表 4 血常规相关参数与肺炎支原体抗体分级水平有序logistic回归分析表
影响因素 β Wald P OR 95%CI PLT 0.026 4.229 0.040 1.026 1.001~1.051 MPV 0.939 5.824 0.016 2.557 1.192~5.484 PCT -25.057 3.563 0.059 0 0.000~2.616 NEUT 0.053 0.319 0.572 1.054 0.877~1.268 LYMPH 0.120 0.908 0.341 1.127 0.880~1.444 MONO -0.439 1.100 0.294 0.644 0.283~1.465 NLR -0.141 0.588 0.443 0.868 0.606~1.244 PLR 0.005 0.846 0.358 1.005 0.995~1.015 -
[1] Tong L, Huang SM, Zheng C, et al. Refractory Mycoplasma pneumoniae pneumonia in children: early recognition and management[J]. J Clin Med, 2022, 11(10): 2824. doi: 10.3390/jcm11102824
[2] 赖宇强, 黄婉怡, 胡婷. 血液标本采集情况及送检时间对血检结果的影响[J]. 中国卫生标准管理, 2020, 11(9): 99-101.
[3] 朱成斌, 蔡春莲. 血常规指标对初诊多发性骨髓瘤临床分期和预后预测价值的研究[J]. 临床血液学杂志, 2021, 34(10): 723-727. https://lcxy.whuhzzs.com/article/doi/10.13201/j.issn.1004-2806.2021.10.010
[4] 余超, 吴玉玲, 张手丽, 等. 血细胞相关比值与多发性骨髓瘤患者临床预后的相关性[J]. 临床血液学杂志, 2023, 36(4): 249-254. https://lcxy.whuhzzs.com/article/doi/10.13201/j.issn.1004-2806.2023.04.006
[5] Koupenova M, Livada AC, Morrell CN. Platelet and megakaryocyte roles in innate and adaptive immunity[J]. Circ Res, 2022, 130(2): 288-308. doi: 10.1161/CIRCRESAHA.121.319821
[6] Repsold L, Joubert AM. Platelet function, role in thrombosis, inflammation, and consequences in chronic myeloproliferative disorders[J]. Cells, 2021, 10(11): 3034. doi: 10.3390/cells10113034
[7] 邓胜, 陈键. 血细胞比值、平均血小板体积评估系统性红斑狼疮活动性研究[J]. 临床血液学杂志, 2021, 34(6): 415-418, 422. https://lcxy.whuhzzs.com/article/doi/10.13201/j.issn.1004-2806.2021.06.009
[8] 刘国才, 刘智强, 张江, 等. 新型冠状病毒感染后特异性IgM和IgG抗体变化规律的初步探索[J]. 实用医学杂志, 2020, 36(13): 1724-1728.
[9] Wang ZH, Bao HJ, Liu Y, et al. Interleukin-23 derived from CD16+ monocytes drives IL-17 secretion by TLR4 pathway in children with mycoplasma pneumoniae pneumonia[J]. Life Sci, 2020, 258: 118149.
[10] Andoh M, Koyama R. Comparative review of microglia and monocytes in CNS phagocytosis[J]. Cells, 2021, 10(10): 2555.
[11] Kloc M, Kubiak JZ. Monocyte and macrophage function diversity[J]. Int J Mol Sci, 2022, 23(20): 12404.
[12] 何婧瑜, 王晶. 单核细胞与成人支原体肺炎病程的关系及其在预测病程中的应用[J]. 首都医科大学学报, 2021, 42(1): 111-116.
[13] Zamora C, Cantó E, Vidal S. The dual role of platelets in the cardiovascular risk of chronic inflammation[J]. Front Immunol, 2021, 12: 625181.
[14] Sun S, Urbanus RT, Ten Cate H, et al. Platelet activation mechanisms and consequences of immune thrombocytopenia[J]. Cells, 2021, 10(12): 3386.
[15] Rolfes V, Ribeiro LS, Hawwari I, et al. Platelets fuel the inflammasome activation of innate immune cells[J]. Cell Rep, 2020, 31(6): 107615.
[16] Liao Y, Liu CG, He WJ, et al. Study on the value of blood biomarkers NLR and PLR in the clinical diagnosis of influenza a virus infection in children[J]. Clin Lab, 2021, 67(11).
[17] Asik Z. The role of the NLR and PLR in urinary tract infection[J]. Clin Lab, 2021, 67(10).
[18] Gasparyan AY, Ayvazyan L, Mukanova U, et al. The platelet-to-lymphocyte ratio as an inflammatory marker in rheumatic diseases[J]. Ann Lab Med, 2019, 39(4): 345-357.
-




 下载:
下载: