Study on correlation between four new coagulation factors and renal function during red blood cell transfusion therapy in patients with acute myeloid leukemia
-
摘要: 目的 分析新凝血四项与急性髓系白血病(acute myeloid leukemia,AML)患者红细胞输注治疗期间肾功能的关系。方法 选择2019年6月至2022年5月陕西省人民医院血液科收入的96例AML患者作为研究对象,均接受红细胞输注治疗,以治疗期间发生急性肾损伤(acute kidney injury,AKI)为终点事件。入科后即采血检测患者血常规、凝血四项、新凝血四项、肾功能及一般资料,根据检查结果,分析新凝血四项与AML患者红细胞输注治疗期间发生AKI的关系。结果 研究入选AML患者96例,红细胞输注无效4例,Ⅳ级骨髓抑制2例,最终90例患者作为最终研究对象。90例患者红细胞输注时间为13.00(11.75,14.00)周,22例(24.44%)患者在红细胞输注治疗期间发生AKI。AKI患者红细胞输注次数、红细胞输注量高于N-AKI患者,血浆血栓调节蛋白(TM)、组织型纤溶酶原激活物-抑制剂-1复合物(t-PAIC)、血浆胱抑素C(CysC)表达高于N-AKI患者,血浆凝血酶-抗凝血酶复合物(TAT)、纤溶酶a2纤溶酶抑制剂复合物(PIC)表达低于N-AKI患者,差异有统计学意义(P<0.05)。采用logistic回归分析发现,红细胞输注次数、血浆TM、t-PAIC表达上调是AML患者红细胞输注治疗期间发生AKI的独立因素(P<0.05)。绘制ROC曲线,新凝血四项中血浆TM、t-PAIC均能够预测AML患者红细胞输注治疗期间AKI发生。结论 新凝血四项中血浆TM、t-PAIC表达上调是AML患者红细胞输注治疗期间发生AKI的危险因素,红细胞输注治疗前检测血浆TM、t-PAIC有助于预测AKI发生。Abstract: Objective To analyze the relationship between the four new coagulation factors and renal function during red blood cell transfusion therapy in the patients with acute myeloid leukemia(AML).Methods 96 AML patients admitted to Department of Hematology of Shaanxi Provincial People's Hospital from June 2019 to May 2022 were selected as the study subjects, all receiving red blood cell transfusion therapy, with acute kidney injury(AKI) occurring during the treatment period as the endpoint event. After admission, blood samples were collected to test the patient's blood routine, coagulation, new coagulation, renal function, and general information. Based on the examination results, the relationship between new coagulation and AKI during red blood cell transfusion therapy in AML patients was analyzed.Results 96 patients with AML were selected in this study, 4 patients with ineffective red blood cell transfusion, 2 patients with grade IV Bone marrow suppression, and 90 patients were finally selected as the final study subjects. 90 patients underwent red blood cell infusion for 13.00(11.75, 14.00) weeks, and 22 patients(24.44%) developed AKI during red blood cell transfusion therapy. The number and amount of red blood cell transfusion in AKI patients were higher than those in N-AKI patients, the expression of plasma thrombomodulin(TM), tissue type plasmin activator inhibitor 1 complex(t-PAIC) and plasma cystatin C(CysC) were higher than those in N-AKI patients, and the expression of plasma thrombin antithrombin complex(TAT) and plasmin a2 plasmin inhibitor complex(PIC) were lower than those in N-AKI patients, with a statistical significant difference(P<0.05). Logistic regression analysis showed that the number of red blood cell transfusions, the up-regulation of plasma TM and t-PAIC expression were independent factors for AKI during red blood cell transfusion in AML patients(P<0.05). The ROC curve was drawn, and plasma TM and t-PAIC in the new coagulation four items could predict the occurrence of AKI during red blood cell transfusion therapy in AML patients.Conclusion Upregulation of plasma TM and t-PAIC expression in the four new coagulation factors may be a risk factor for AKI in AML patients during red blood cell transfusion therapy. Detection of plasma TM and t-PAIC before red blood cell transfusion therapy could help predict the occurrence of AKI.
-

-
表 1 AML患者一般临床资料
一般资料 AKI(n=22) N-AKI(n=68) t/χ2/Z P 年龄/岁 42.50±8.11 44.65±6.94 1.210 0.230 性别/例(%) 1.828 0.176 男 14(63.64) 32(47.06) 女 8(36.36) 36(52.94) FAB分型/例(%) 2.265 0.687 M0 3(13.64) 11(16.18) M1 5(22.73) 15(22.06) M2 5(22.73) 10(14.71) M4 7(31.82) 18(26.47) M5 2(9.09) 14(20.59) 预后危险度/例(%) 1.474 0.225 预后良好 5(22.73) 25(36.76) 预后中等 17(77.27) 43(63.24) 红细胞输注次数/次 7.50(6.00,8.00) 6.00(5.00,6.00) 4.350 <0.001 红细胞输注量/例(%) 8.668 0.003 ≥10 U 16(72.73) 25(36.76) <10 U 6(27.27) 43(63.24) WBC/(×109/L) 23.33±5.15 21.86±5.83 1.055 0.294 RBC/(×1012/L) 2.83±0.25 2.92±0.21 1.649 0.103 Hb/(g/L) 46.45±5.12 48.37±5.54 1.430 0.156 TT/s 18.00(17.00,19.00) 18.00(18.00,19.00) 0.980 0.327 PT/s 13.00(12.00,14.00) 13.00(11.25,13.00) 0.814 0.416 APTT/s 32.00(29.75,33.00) 31.00(29.00,33.00) 1.120 0.263 Fib/(g/L) 2.38±0.33 2.52±0.31 1.875 0.064 TM/(TU/mL) 25.16±3.53 20.91±3.06 5.445 <0.001 TAT/(ng/mL) 2.02±0.24 2.16±0.25 2.352 0.021 t-PAIC/(ng/mL) 11.27±2.08 8.82±1.82 5.296 <0.001 PIC/(μg/mL) 4.37±0.63 4.80±0.81 2.550 0.014 Scr/(μmol/L) 82.36±6.64 80.58±8.13 1.032 0.308 BUN/(mmol/L) 5.13±1.13 5.35±0.94 0.910 0.365 CysC/(mg/L) 6.77±1.22 6.12±1.15 2.264 0.026 β2-MG/(mg/L) 3.13±0.36 2.97±0.25 1.918 0.066 表 2 新凝血四项与AML患者红细胞输注治疗期间发生AKI的关系
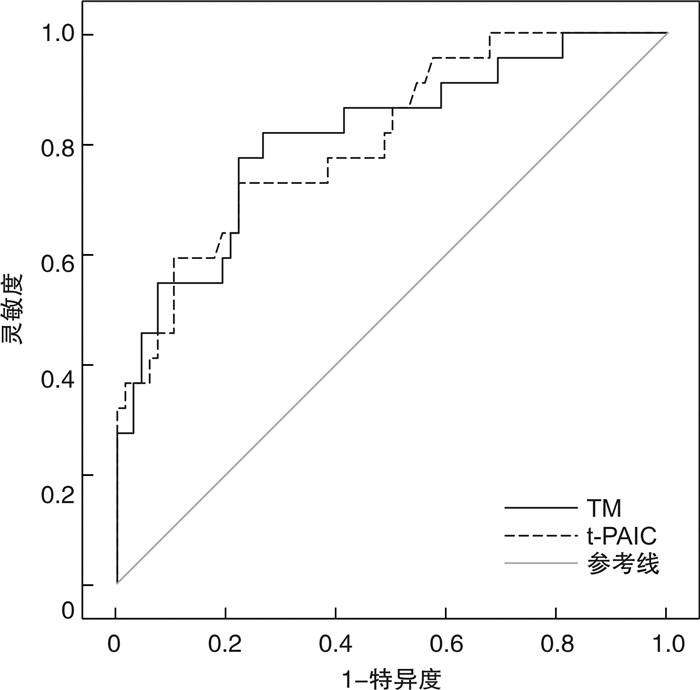
项目 β SE Wald P OR 95%CI 红细胞输注次数 1.051 0.387 7.377 0.007 2.861 1.340~6.110 红细胞输注量 0.038 0.964 0.002 0.968 1.039 0.157~6.877 TM 0.446 0.153 8.478 0.004 1.563 1.157~2.110 TAT -2.265 1.806 1.573 0.210 0.104 0.003~3.578 t-PAIC 0.959 0.339 7.996 0.005 2.609 1.342~5.072 PIC -1.066 0.710 2.255 0.133 0.344 0.086~1.384 CysC 0.334 0.442 0.570 0.450 1.396 0.587~3.318 常量 -20.403 7.252 7.915 0.005 - - 表 3 新凝血四项预测AML患者红细胞输注治疗期间发生AKI的ROC曲线
指标 AUC 95%CI 截断值 特异度 灵敏度 约登指数 TM 0.813 0.705~0.921 22.565 TU/mL 0.735 0.818 0.553 t-PAIC 0.808 0.704~0.912 8.965 ng/mL 0.515 0.818 0.333 -
[1] Lopes M, Duarte TL, Teles MJ, et al. Loss of erythroblasts in acute myeloid leukemia causes iron redistribution with clinical implications[J]. Blood Adv, 2021, 5(16): 3102-3112. doi: 10.1182/bloodadvances.2021004373
[2] Shimmer C, Hamouda K, Ozkur M, et al. Influence of storage time and amount of red blood cell transfusion on postoperative renal function: an observational cohort study[J]. Heart Lung Vessel, 2013, 5(3): 148-157.
[3] Dahl SL, Bapst AM, Khodo SN, et al. Fount, fate, features, and function of renal erythropoietin-producing cells[J]. Pflugers Arch, 2022, 474(8): 783-797. doi: 10.1007/s00424-022-02714-7
[4] 王伊娜, 董葆, 李欣, 等. 白血病肾损害患者的临床病理特征研究[J]. 中国全科医学, 2022, 25(8): 952-956, 962.
[5] 赵志明, 马诗静, 李莉. 慢性肾脏病患者凝血功能变化及与肾功能指标的相关性[J]. 微循环学杂志, 2022, 32(3): 52-56.
[6] 朱理平, 孙竞. 初诊243例急性白血病凝血等指标检测临床价值[J]. 昆明医科大学学报, 2019, 40(5): 103-107. doi: 10.3969/j.issn.1003-4706.2019.05.019
[7] 杨燕贻, 胡芸, 武明阳, 等. 长沙健康妊娠妇女新凝血标志物水平变化及其参考区间的建立[J]. 中南大学学报(医学版), 2022, 47(4): 469-478.
[8] 沈悌, 赵永强. 血液病诊断及疗效标准[M]. 4版. 北京: 科学出版社, 2018: 92-109.
[9] Palevsky PM, Liu KD, Brophy PD, et al. KDOQI US commentary on the 2012 KDIGO clinical practice guideline for acute kidney injury[J]. Am J Kidney Dis, 2013, 61(5): 649-672. doi: 10.1053/j.ajkd.2013.02.349
[10] Ballo O, Eladly F, Büttner S, et al. Acute kidney injury adversely affects the clinical course of acute myeloid leukemia patients undergoing induction chemotherapy[J]. Ann Hematol, 2021, 100(5): 1159-1167. doi: 10.1007/s00277-021-04482-3
[11] Gupta R. Red blood cell transfusion and cardiac surgery-associated acute kidney injury[J]. JACC Basic Transl Sci, 2022, 7(7): 639-641. doi: 10.1016/j.jacbts.2022.04.011
[12] Rasmussen SR, Kandler K, Nielsen RV, et al. Association between transfusion of blood products and acute kidney injury following cardiac surgery[J]. Acta Anaesthesiol Scand, 2020, 64(10): 1397-1404. doi: 10.1111/aas.13664
[13] 吴文军, 丁任重, 陈建明, 等. 机器人心脏外科术后急性肾功能损伤的危险因素分析[J]. 临床心血管病杂志, 2023, 39(1): 51-56.
[14] 储腊萍, 俞娅芬, 郭黎晨, 等. 补体及凝血指标对脓毒症并发急性肾损伤的预测价值[J]. 中华内科杂志, 2020, 59(11): 854-859.
[15] 冯爱梅, 赵朴, 徐钰, 等. 急性白血病患者免疫指标、凝血指标、基质衍生因子-1α及乳酸脱氢酶的检测及其临床意义[J]. 中国卫生检验杂志, 2020, 30(2): 183-185.
[16] 莫曼秋, 潘玲, 严官强, 等. 凝血指标与脓毒症相关急性肾损伤患者全因死亡的相关性分析[J]. 中华肾脏病杂志, 2019, 35(10): 758-764.
[17] 金宁, 徐晓芬, 张晓飞, 等. 血栓四项检测在急诊内科肺部疾病患者疾病严重程度判断中的价值[J]. 检验医学与临床, 2023, 20(1): 81-84.
[18] 张彤, 董夏昕, 雷娜, 等. 血栓四项指标与血栓弹力图参数检测对脓毒血症合并弥散性血管内凝血的早期诊断价值比较[J]. 陕西医学杂志, 2021, 50(1): 100-102, 110.
[19] 周坤, 周玉珍, 郑遵荣, 等. 血栓四项在恶性肿瘤患者静脉血栓形成中的应用研究[J]. 中国医师进修杂志, 2019, 42(11): 994-999.
[20] 郑洋洋, 闫海润, 李琪, 等. 恶性肿瘤患者血栓分子标志物的临床评价[J]. 中华检验医学杂志, 2020, 43(1): 78-84.
[21] Aratani S, Aburakawa S, Ryotokuji T, et al. Primary tumor infiltration and severe acute kidney injury in patients with acute myeloblastic leukemia[J]. Nippon Ika Daigaku Zasshi, 2020, 87(1): 43-48.
[22] Rehill AM, Preston RJS. A new thrombomodulin-related coagulopathy[J]. J Thromb Haemost, 2020, 18(9): 2123-2125.
[23] 刘力铭. 悬浮红细胞及血浆输注对大量输血手术患者凝血功能的影响[J]. 检验医学与临床, 2021, 18(9): 1254-1256, 1261.
[24] 王晓华, 孙琳, 常亚. 不同红细胞输注对再生障碍性贫血患者红细胞免疫功能及凝血的影响[J]. 国际免疫学杂志, 2021, 44(1): 29-34.
[25] 刘念, 徐晓玲, 舒会英. 红细胞悬液与血浆不同比例输注对急性创伤患者凝血功能、纤溶功能及血栓弹力图监测结果的影响[J]. 实用医院临床杂志, 2021, 18(2): 96-99.
-




 下载:
下载: