Relationship of Hcy, β2-MG and hematopoietic score system and prognosis in patients with multiple myeloma
-
摘要: 目的 分析同型半胱氨酸(Hcy)、β2微球蛋白(β2-MG)和造血评分系统与多发性骨髓瘤(multiple myeloma,MM)患者预后的关系及预测价值。方法 选取2017年1月—2020年2月医院收治的100例MM患者,随访3年后依据患者存活情况分为存活组(66例)和死亡组(34例),依据国际分期系统(international staging system,ISS)将患者分为ISS Ⅰ期组(35例)、ISS Ⅱ期组(30例)与ISS Ⅲ期组(35例)。比较不同预后组和不同ISS分期患者Hcy、β2-MG及造血评分系统。结果 存活组与死亡组性别、体重指数(BMI)、是否合并高血压、是否合并糖尿病、吸烟史、饮酒史、骨髓浆细胞、血红蛋白(Hb)、血钙(Ca)、血肌酐(Scr)水平比较,差异无统计学意义(P>0.05),存活组年龄低于死亡组(P < 0.05);ISS Ⅰ期组血清Hcy、β2-MG低于ISS Ⅱ期组、ISS Ⅲ期组(P < 0.05),ISS Ⅱ期组Hcy、β2-MG低于ISS Ⅲ期组(P < 0.05),ISS Ⅰ期组造血评分系统≥1.5分比例低于ISS Ⅱ期组、ISS Ⅲ期组(P < 0.05),ISS Ⅱ期组造血评分系统≥1.5分比例低于ISSⅢ期组,P < 0.05);存活组血清Hcy、β2-MG低于死亡组(P < 0.05),存活组造血评分系统≥1.5分比例低于死亡组患者(P < 0.05);进行logistic回归分析:年龄、Hcy、β2-MG、造血评分系统是MM患者预后不良的影响因素(P < 0.05);Hcy、β2-MG、造血评分系统单独预测MM患者预后的受试者工作特征曲线(ROC)下面积(AUC)分别为0.883(0.807~0.959)、0.887(0.822~0.951)、0.762(0.702~0.865),灵敏度分别为0.852、0.867、0.895,特异度分别为0.855、0.830、0.816,Hcy、β2-MG、造血评分系统联合预测MM患者预后的ROC曲线下面积为0.928(0.877~0.979),灵敏度为0.908,特异度为0.810。结论 MM预后与患者血清Hcy、β2-MG水平及造血评分系统密切相关,Hcy、β2-MG和造血评分系统联合预测MM预后比单独预测价值更高。Abstract: Objective To analyse the relationship between Hcy, β2-microglobulin(β2-MG) and the hematopoietic scoring system and the prognosis of patients with multiple myeloma(MM) patients, and evaluate the value of predicting the prognosis with them.Methods The 100 patients with multiple myeloma admitted to the hospital from January 2017 to February 2020 were divided into survival group(66 patients) and death group(34 patients), and into ISS Ⅰ(35 patients), ISS Ⅱ(30 patients) and ISS Ⅲ(35 patients) according to the international staging system(ISS). The general data of patients including Hcy, β2-MG and the hematopoietic scoring systems were compared in different prognosis groups, and Hcy, β2-MG and the hematopoietic scoring systems were compared in different prognosis groups, and patients with different ISS stages.Results The comparsion of the group with good prognosis and the group with poor prognosis in gender, body mass index (BMI), hypertension, diabetes, smoking history, alcohol history, bone marrow plasma cells, hemoglobin(Hb), blood calcium(Ca) and blood creatinine (Scr) level was not statistically different (P>0.05). The age of the group with good prognosis was lower than the group with poor prognosis (P < 0.05). The Hcy and β2-MG in serum of ISS stageⅠ group was lower than those of ISS stage Ⅱ group and ISS stage Ⅲ group (P < 0.05). The Hcy and β2-MG in serum of ISS stage Ⅱ group was lower than those of ISS stage Ⅲ group(P < 0.05). The proportion of score ≥1.5 of ISS Ⅰ was lower than that of ISS Ⅱ and ISS Ⅲ (P < 0.05). The proportion of score ≥1.5 of ISS Ⅱ was lower than that in the ISS Ⅲ (P < 0.05). The Hcy and β2-MG in the survival group was lower than those of the death group (P < 0.05), the proportion of score ≥1.5 in the survival group was lower than that in the death group (P < 0.05). Logistic regression analysis showed that age, Hcy, β2-MG and the hematopoietic scoring system were the factors affecting the poor prognosis in patients with multiple myeloma (P < 0.05). The area under the ROC curve for Hcy, β2-MG and the hematopoietic scoring system alone predicting the prognosis of patients with multiple myeloma were 0.883(0.807-0.959), 0.887(0.822-0.951), 0.762(0.702-0.865), the sensitivities were 0.852, 0.867, and 0.895, the specificities were 0.855, 0.830, and 0.816, respectively. The area under the ROC curve of the Hcy, β2-MG and the hematopoietic scoring system combined to predict the prognosis of patients with multiple myeloma was 0.928 (0.877-0.979), the sensitivity was 0.908, and the specificity level was 0.810.Conclusion The prognosis of multiple myeloma might be closely related to serum Hcy, β2-MG level and hematopoietic scoring system, and the combination of Hcy, β2-MG and hematopoietic scoring system might have higher prediction value than alone.
-

-
表 1 2组一般资料比较
项目 存活组(n=66) 死亡组(n=34) t/χ2 P 性别/例(%) 0.017 0.905 男 38(57.58) 20(58.82) 女 28(42.42) 14(41.18) 年龄/岁 57.03± 2.05 59.12± 2.14 4.692 <0.001 BMI 23.15± 1.08 23.26± 1.14 0.473 0.637 高血压/例(%) 26(39.39) 14(41.18) 0.030 0.863 糖尿病/例(%) 20(30.30) 13(38.24) 0.639 0.424 吸烟史/例(%) 18(27.27) 12(35.29) 0.688 0.407 饮酒史/例(%) 15(22.73) 9(26.47) 0.172 0.678 骨髓浆细胞/例(%) 0.186 0.666 ≥30% 30(45.45) 17(50.00) <30% 36(54.55) 17(50.00) Hb/例(%) 0.364 0.546 ≥100 g/L 41(62.12) 19(55.88) <100 g/L 25(37.88) 15(44.12) Ca/例(%) 0.386 0.535 ≥2.5 mmol/L 43(65.15) 20(58.82) <2.5 mmol/L 23(34.85) 14(41.18) Scr/例(%) 0.172 0.679 ≥110 μmol/L 32(48.48) 15(44.12) <110 μmol/L 34(51.52) 19(55.88) 表 2 3组Hcy、β2-MG及造血评分系统比较
组别 例数 Hcy/(μmol/L) β2-MG/(mg/L) 造血评分系统/例(%) ≥1.5分 <1.5分 ISS Ⅰ期组 35 8.42±1.56 3.02±0.26 5(14.29) 30(85.71) ISS Ⅱ期组 30 13.78±2.33 4.30±0.37 13(43.33) 17(56.67) ISS Ⅲ期组 35 21.87±3.37 6.34±0.85 21(60.00) 14(40.00) t/χ2 248.180 308.182 15.711 P < 0.001 < 0.001 < 0.001 表 3 不同预后组Hcy、β2-MG及造血评分系统比较
组别 例数 Hcy/(μmol/L) β2-MG/(mg/L) 造血评分系统/例(%) ≥1.5分 <1.5分 存活组 66 10.86±1.85 4.19±0.48 14(21.21) 52(78.79) 死亡组 34 21.63±3.36 6.24±0.85 25(73.53) 9(26.47) t/χ2 -41.410 -15.430 25.818 P < 0.001 < 0.001 < 0.001 表 4 多因素分析
影响因素 β SE Walds P OR(95%CI) 年龄 0.498 0.168 10.524 0.002 1.136~1.963 Hcy 0.102 0.123 8.957 0.014 1.031~1.124 β2-MG 0.351 0.450 6.589 0.026 0.995~1.365 造血评分系统 0.524 0.342 4.631 0.041 1.125~2.314 表 5 3种指标单独及联合预测MM患者的预后价值
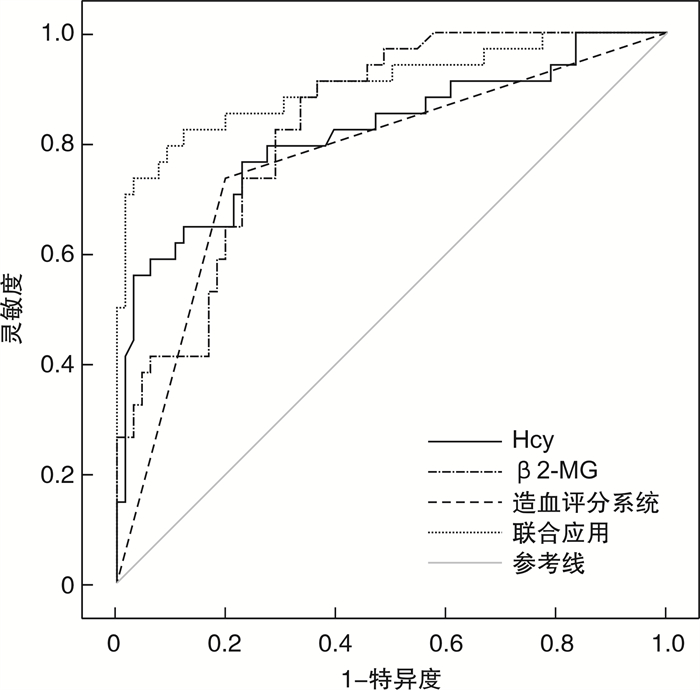
影响因素 灵敏度 特异度 AUC 95%CI Hcy 0.852 0.855 0.883 0.807~0.959 β2-MG 0.867 0.830 0.887 0.822~0.951 造血评分系统 0.895 0.816 0.762 0.702~0.865 联合 0.908 0.810 0.928 0.877~0.979 -
[1] Cowan AJ, Green DJ, Kwok M, et al. Diagnosis and Management of Multiple Myeloma: A Review[J]. JAMA, 2022, 327(5): 464-477. doi: 10.1001/jama.2022.0003
[2] 李其辉, 刘彦, 王晶, 等. 新药时代早期复发对新诊断多发性骨髓瘤患者预后的影响及其危险因素分析[J]. 中国实验血液学杂志, 2023, 31(1): 148-153. https://www.cnki.com.cn/Article/CJFDTOTAL-XYSY202301022.htm
[3] Minnie SA, Hill GR. Immunotherapy of multiple myeloma[J]. J Clin Invest, 2020, 130(4): 1565-1575. doi: 10.1172/JCI129205
[4] 凌小穗, 何海萍, 张丽华, 等. 多发性骨髓瘤患者来源间充质干细胞的最新研究进展[J]. 中国实验血液学杂志, 2023, 31(4): 1233-1236. https://www.cnki.com.cn/Article/CJFDTOTAL-XYSY202304047.htm
[5] 伏媛, 魏小芳, 冯友繁, 等. 血清同型半胱氨酸水平对初诊多发性骨髓瘤多发性骨髓瘤患者预后的影响及相关因素分析[J]. 中国实验血液学杂志, 2021, 29(2): 530-534. https://www.cnki.com.cn/Article/CJFDTOTAL-XYSY202102040.htm
[6] 费晓莉, 陶黎, 熊梅, 等. IL-37、VEGF、LDH和β2-MG在多发性骨髓瘤多发性骨髓瘤中的表达及其临床意义[J]. 重庆医学, 2021, 50(2): 275-279. doi: 10.3969/j.issn.1671-8348.2021.02.021
[7] 宋丽敏, 马艳萍, 薛茹, 等. 由HB、PLT和MCV组成的造血评分系统与多发性骨髓瘤多发性骨髓瘤患者预后及疗效相关性的研究[J]. 中国实验血液学杂志, 2022, 30(2): 481-486. https://www.cnki.com.cn/Article/CJFDTOTAL-XYSY202202026.htm
[8] 中国多发性骨髓瘤多发性骨髓瘤工作组. 中国多发性骨髓瘤多发性骨髓瘤诊治指南[J]. 中华内科杂志, 2008, 47(10): 869-872. doi: 10.3321/j.issn:0578-1426.2008.10.035
[9] 李淑娥, 葛洪峰, 孙晓星, 等. 不同国际分期体系分期的多发性骨髓瘤多发性骨髓瘤患者WB-DWI表现及预后[J]. 分子影像学杂志, 2021, 44(3): 492-495. https://www.cnki.com.cn/Article/CJFDTOTAL-FZYX202103015.htm
[10] AlSaleh AS, Sidiqi MH, Dispenzieri A, et al. Hemato-poietic score predicts outcomes in newly diagnosed multiple myeloma patients[J]. Am J Hematol, 2020, 95(1): 4-9. doi: 10.1002/ajh.25657
[11] Wallington-Beddoe CT, Mynott RL. Prognostic and predictive biomarker developments in multiple myeloma[J]. J Hematol Oncol, 2021, 14(1): 151. doi: 10.1186/s13045-021-01162-7
[12] 王亚茹, 马艳萍. NAMPT在多发性骨髓瘤患者中的表达及临床相关性研究[J]. 中国实验血液学杂志, 2023, 31(3): 769-776. https://www.cnki.com.cn/Article/CJFDTOTAL-XYSY202303022.htm
[13] Cossu G, Terrier LM, Benboubker L, et al. Spinal metastases in multiple myeloma: A high-risk subgroup for ISS Ⅲ patients[J]. Surg Oncol, 2018, 27(2): 321-326. doi: 10.1016/j.suronc.2018.05.005
[14] 王思英, 邱东飚, 范翠花. 血清白细胞介素-33、β2-微球蛋白水平与多发性骨髓瘤患者DS分期的相关性[J]. 中国实验血液学杂志, 2023, 31(3): 788-793. https://www.cnki.com.cn/Article/CJFDTOTAL-XYSY202303025.htm
[15] 王豪言, 孙晓白, 李梦一, 等. 多发性骨髓瘤患者首次治疗部分缓解时NLR、MLR与预后的关系[J]. 山东医药, 2023, 63(8): 1-5. https://www.cnki.com.cn/Article/CJFDTOTAL-SDYY202308001.htm
[16] 郝苗, 毛志刚, 罗开宏. 血清骨特异性碱性磷酸酶、同型半胱氨酸、护骨素变化对多发性骨髓瘤多发性骨髓瘤患者的临床应用价值[J]. 标记免疫分析与临床, 2020, 27(1): 32-36. https://www.cnki.com.cn/Article/CJFDTOTAL-BJMY202001008.htm
[17] Ying L, Zhang X, Lu N, et al. Evaluating the screening value of serum light chain ratio, β2 microglobulin, lactic dehydrogenase and immunoglobulin in patients with multiple myeloma using ROC curves[J]. PLoS One, 2023, 18(2): e0281743. doi: 10.1371/journal.pone.0281743
[18] 钟沂芮. 异基因造血干细胞移植治疗多发性骨髓瘤多发性骨髓瘤的诊治现状[J]. 重庆医学, 2022, 51(14): 2504-2509. doi: 10.3969/j.issn.1671-8348.2022.14.036
[19] 谷敏, 秦云, 白莎莎, 等. 血清Hcy、HMGB1水平与多发性骨髓瘤多发性骨髓瘤患者预后的关系[J]. 医学临床研究, 2023, 40(2): 173-175, 179. doi: 10.3969/j.issn.1671-7171.2023.02.004
[20] 张灵, 陈哲, 范凌, 等. 同型半胱氨酸代谢酶基因多态性与汉族多发性骨髓瘤多发性骨髓瘤预后的关系[J]. 中国医师进修杂志, 2022, 45(12): 1066-1070.
[21] 韩少玲, 吴亚兵, 张家友, 等. 多发性骨髓瘤多发性骨髓瘤患者血清β2-MG、CRP和IL-6水平与临床分期的关系[J]. 河北医药, 2021, 43(3): 353-356. doi: 10.3969/j.issn.1002-7386.2021.03.007
[22] 要星晨, 徐子彧, 史湘君, 等. 经皮椎体后凸成形术与经皮椎体成形术治疗多发性骨髓瘤多发性骨髓瘤椎体病理性骨折的疗效及预后分析[J]. 中国骨与关节杂志, 2021, 10(4): 293-299. https://www.cnki.com.cn/Article/CJFDTOTAL-GZGL202104013.htm
[23] 毛沛沛, 乔莎, 肖晶晶. 多发性骨髓瘤多发性骨髓瘤患者血清β2-MG、TNF-α、LDH的水平变化及与预后相关性[J]. 分子诊断与治疗杂志, 2023, 15(2): 273-276. https://www.cnki.com.cn/Article/CJFDTOTAL-YXYQ202302023.htm
[24] 刘宁洒, 李玉陶, 徐晓奇, 等. 造血评分系统对初诊多发性骨髓瘤患者的预后价值[J]. 临床血液学杂志, 2021, 34(1): 13-17, 23. https://lcxy.whuhzzs.com/article/doi/10.13201/j.issn.1004-2806.2021.01.004
-




 下载:
下载: