Predictive value and influence of C-reactive protein/albumin on renal insufficiency in patients with diabetic kidney disease
-
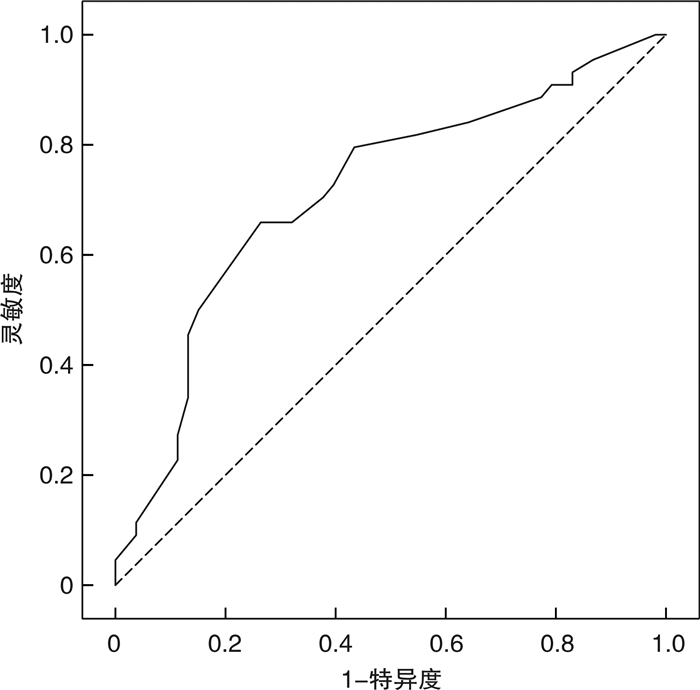
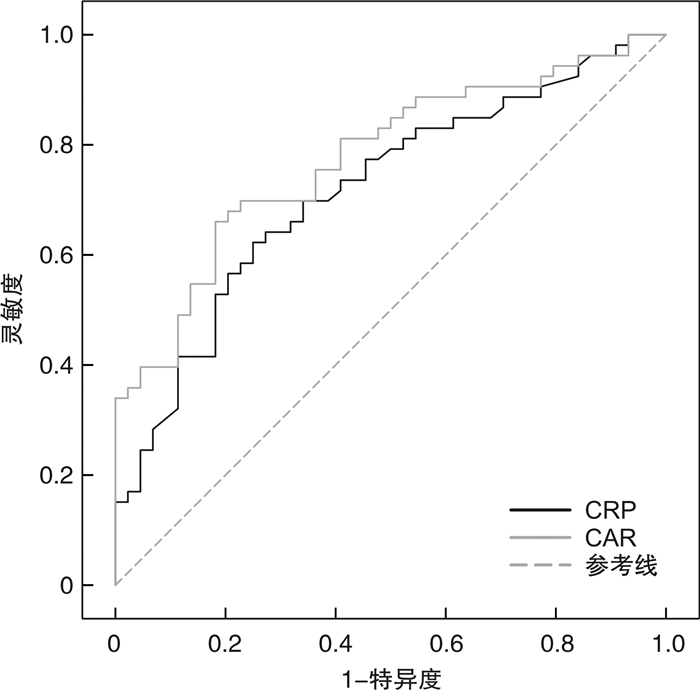
摘要: 目的 分析C反应蛋白(CRP)、血清白蛋白(ALB)及C反应蛋白/血清白蛋白(CAR)对糖尿病肾病(DKD)肾功能不全的预测价值。方法 选取2015年4月至2020年10月,静安区、杨浦区中心医院就诊治疗的DKD患者97例,根据肾小球滤过率(e-GFR)是否 < 60 mL/(min·1.73 m2),将患者分为肾功能不全组(53例)和非肾功能不全组(44例),比较CRP、ALB、CAR对肾功能不全的预测价值。结果 CRP、CAR对肾功能不全预测的曲线下面积(AUC)分别为0.717、0.776,ALB预测非肾功能不全的AUC为0.714,CAR预测价值高于CRP、ALB,差异有统计学意义(P< 0.05)。CAR≥0.37与CAR < 0.37的DKD患者间病程、e-GFR、肾功能不全占比、尿酸(UA)、CRP、ALB、CAR、空腹血糖(FPG)、血红蛋白(Hb)、中性粒细胞/淋巴细胞(NLR)、白细胞计数(WBC)比较,差异均有统计学意义(均P< 0.05)。单因素分析显示,肾功能不全和非肾功能不全组间病程、e-GFR、UA、CRP、ALB、CAR、CAR≥0.37占比、Hb、NLR差异有统计学意义(P< 0.05)。二元logistic回归分析显示,CAR≥0.37、病程、NRL均为DKD患者肾功能不全的独立影响因素(均P< 0.05)。纠正混杂因素后CAR≥0.37为DKD患者肾功能不全的影响因素(P< 0.05),而CRP、ALB均不是DKD患者肾功能不全的影响因素。结论 CAR≥0.37对DKD患者肾功能不全的预测价值高于CRP、ALB,且CAR≥0.37为肾功能不全独立的影响因素。Abstract: Objective To analyze the predictive value of C-reactive protein(CRP), serum albumin(ALB) and CRP/ALB(CAR) on renal insufficiency in patients with diabetic nephropathy(DKD).Methods A total of 97 patients with DKD treated in Jing'an District, Yangpu District Central Hospital from April 2015 to October 2020 were selected. According to whether the glomerular filtration rate(e-GFR) was less than 60 mL/(min·1.73 m2), all patients were divided into renal insufficiency group(53 cases) and non-renal insufficiency group(44 cases). The predictive value and influence of CRP, ALB and CAR on renal insufficiency were compared.Results The areas under the curve(AUC) of CRP and CAR in predicting renal insufficiency were 0.717 and 0.776 respectively, and the AUC of ALB in predicting non-renal insufficiency was 0.714. The predictive value of CAR was higher than that of CRP and ALB(allP< 0.05). There were significant differences in disease course, e-GFR, proportion of renal insufficiency, uric acid(UA), CRP, ALB, CAR, fasting plasma glucose(FPG), hemoglobin(Hb), neutrophil/lymphocyte(NLR) and white blood cell count(WBC) between DKD patients with CAR≥0.37 and CAR < 0.37(P< 0.05). Binary logistic regression analysis showed that CAR≥0.37, course of disease and NRL were independent influencing factors of renal insufficiency in the patients with DKD(P< 0.05). After correcting confounding factors, CAR≥0.37 was the influencing factor of renal insufficiency in the patients with DKD(P< 0.05), while CRP and ALB were not the influencing factors of renal insufficiency in the patients with DKD.Conclusion The predictive value of CAR≥0.37 for renal insufficiency in patients with DKD is higher than that of CRP and ALB, and CAR≥0.37 may be an independent influencing factor of renal insufficiency.
-

-
表 1 3种检测指标AUC比较
检测方法 面积差异 Se z P CRP vs ALB 0.003 0.072 0.214 0.637 CRP vs CAR 0.059 0.045 1.947 0.036 ALB vs CAR 0.062 0.055 2.012 0.029 表 2 不同CAR组间临床资料比较
X±S 临床资料 CAR≥0.37(43例) CAR < 0.37(54例) t/χ2 P 性别/例 0.446 0.504 男 26 29 女 17 25 年龄/岁 61.14±7.23 61.11±9.00 0.017 0.987 病程/年 9.23±2.31 8.07±2.71 2.231 0.028 SBP/mmHg 141.91±11.06 143.07±9.68 0.554 0.581 DBP/mmHg 84.53±8.71 85.39±5.89 0.575 0.567 e-GFR/(mL·min-1·1.73 m-2) 47.24±12.93 64.86±12.37 6.832 < 0.001 是否肾功能不全/例 22.311 < 0.001 是 35 18 否 8 36 UA/(mmol·L-1) 367.02±26.08 354.85±32.26 2.006 0.048 CRP/(mg·L-1) 17.56±2.56 12.18±2.53 10.307 < 0.001 ALB/(g·L-1) 36.09±5.51 42.31±5.17 5.713 < 0.001 CAR/(mg·L-1) 0.494±0.09 0.289±0.05 14.172 < 0.001 HbA1c/% 7.21±0.45 7.16±0.43 0.614 0.541 FPG/(mmol·L-1) 8.45±1.08 7.95±1.19 2.142 0.035 Hb/(g·L-1) 110.14±9.90 114.94±7.97 2.648 0.009 NLR 2.47±0.45 2.15±0.24 4.468 < 0.001 WBC/(×109·L-1) 6.40±0.99 5.98±1.05 2.040 0.044 表 3 DKD肾功能不全单因素分析
X±S 临床资料 肾功能不全组(53例) 非肾功能不全组(44例) t/χ2 P 性别/例 0.713 0.378 男 28 27 女 25 17 年龄/岁 60.17±8.32 61.91±8.13 0.856 0.394 病程/年 9.58±1.98 7.38±2.75 4.567 < 0.001 SBP/mmHg 144.17±11.35 140.61±8.53 1.713 0.090 DBP/mmHg 84.55±7.98 85.57±6.30 0.689 0.493 e-GFR/(mL·min-1·1.73 m-2) 45.44±9.48 71.03±7.08 14.809 < 0.001 UA/(mmol·L-1) 366.98±27.19 352.14±31.82 2.477 0.015 CRP/(mg·L-1) 15.89±3.60 12.97±3.16 4.208 < 0.001 ALB/(g·L-1) 37.60±5.72 41.91±5.85 3.650 < 0.001 CAR/(mg·L-1) 0.44±0.13 0.31±0.08 5.499 < 0.001 CAR≥0.37/例 22.311 < 0.001 是 35 8 否 18 36 HbA1c/% 7.24±0.51 7.13±0.39 1.174 0.244 FPG/(mmol·L-1) 8.37±1.12 8.03±1.16 1.465 0.146 Hb/(g·L-1) 110.56±9.19 115.53±8.44 2.744 0.006 NLR 2.44±0.43 2.13±0.23 4.223 < 0.001 WBC/(×109·L-1) 6.10±0.97 6.25±1.13 0.719 0.474 表 4 DKD患者肾功能不全多因素分析
变量 P OR 95%CI 下限 上限 CAR≥0.37 0.006 3.845 1.570 8.946 病程 0.003 1.420 1.128 1.788 NRL < 0.001 4.605 1.838 9.681 Hb 0.333 0.969 0.909 1.033 表 5 纠正混采因素不同指标对肾功能不全的影响
变量 P OR 95%CI 下限 上限 CAR≥0.37 0.006 3.845 1.570 8.946 CRP 0.140 1.135 0.959 1.342 ALB 0.054 0.913 0.832 1.001 -
[1] 张新研. 外周血及尿液中相关指标在中老年早期糖尿病肾病中的研究[J]. 临床血液学杂志, 2021, 34(8): 564-567. https://www.cnki.com.cn/Article/CJFDTOTAL-LCXZ202108009.htm
[2] Wang FZ, Sun HH, Zuo BJ, et al. Metformin attenuates renal tubulointerstitial fibrosis via upgrading autophagy in the early stage of diabetic nephropathy[J]. Sci Rep, 2021, 11(1): 16362. doi: 10.1038/s41598-021-95827-5
[3] 代俊伟, 唐晓磊. 血清中CysC、RBP、Hcy、CRP水平与糖尿病肾病分期相关性研究[J]. 国际泌尿系统杂志, 2020, 40(3): 385-388.
[4] Zhang JL, Zhang R, Wang YT, et al. The Level of Serum Albumin Is Associated with Renal Prognosis in Patients with Diabetic Nephropathy[J]. J Diabetes Res, 2019, 2019: 7825804.
[5] 中华医学会糖尿病学分会微血管并发症学组. 中国糖尿病肾脏疾病防治临床指南[J]. 中华糖尿病杂志, 2019, 11(1): 15-28.
[6] 肖梦瑶, 杨迎, 刘松梅. 2型糖尿病肾病的临床生化指标变化特征和危险因素分析[J]. 国际检验医学杂志, 2021, 42(14): 1671-1674, 1678. https://www.cnki.com.cn/Article/CJFDTOTAL-GWSQ202114002.htm
[7] Sagoo MK, Gnudi L. Diabetic Nephropathy: An Overview[J]. MethodsMol Biol, 2020, 2067: 3-7.
[8] Zhang J, Zhang R, Wang Y, et al. Effects of neutrophil-lymphocyte ratio on renal function and histologic lesions in patients with diabetic nephropathy[J]. Nephrology(Carlton), 2019, 24(11): 1115-1121.
[9] Bhandarkar N, Save S, Bavdekar SB, et al. Serum Albumin and C-Reactive Protein as Predictors of Adverse Outcomes in Critically Ⅲ Children: A Prospective Observational Pilot Study[J]. Indian J Pediatr, 2019, 86(8): 758-759.
[10] Tamer F, Avcı E. Serum C-reactive protein to albumin ratio as a novel inflammation biomarker in psoriasis patients treated with adalimumab, ustekinumab, infliximab, and secukinumab: a retrospective study[J]. Croat Med J, 2020, 61(4): 333-337.
[11] 王晓红, 左淑丽. 2型糖尿病患者血清淀粉样蛋白A的表达及与糖尿病肾病的关系[J]. 中国实用医药, 2021, 16(17): 18-20. https://www.cnki.com.cn/Article/CJFDTOTAL-ZSSA202117005.htm
[12] Dieter BP, Meek RL, Anderberg RJ, et al. Serum amyloid A and Janus kinase 2 in a mouse model of diabetic kidney disease[J]. PLoS One, 2019, 14(2): e0211555.
[13] 何霁, 孙娜, 袁宁, 等. 外周血SFRP1、SAA检测在早期糖尿病肾病诊断中的价值[J]. 国际检验医学杂志, 2021, 42(4): 493-496. https://www.cnki.com.cn/Article/CJFDTOTAL-GWSQ202104026.htm
[14] 王涛, 高志琪, 高志戎, 等. 尿MA联合血清TRFα1-MG胱抑素C检测在糖尿病早期肾损伤诊断中的应用[J]. 河北医学, 2021, 27(5): 727-732. https://www.cnki.com.cn/Article/CJFDTOTAL-HCYX202105006.htm
[15] Wada J, Makino H. Innate immunity in diabetes and diabetic nephropathy[J]. Nat Rev Nephrol, 2016, 12(1): 13-26.
[16] Magzal F, Sela S, Szuchman-Sapir A, et al. In-vivo oxidized albumin-a pro-inflammatory agent in hypoalbuminemia[J]. PLoS One, 2017, 12(5): e0177799.
[17] Zhu Y, Cai XL, Liu Y, et al. Serum Albumin, but not Bilirubin, is Associated with Diabetic Chronic Vascular Complications in a Chinese Type 2 Diabetic Population[J]. Sci Rep, 2019, 9(1): 12086.
-




 下载:
下载: