Predictive study of platelet count in early-onset neonatal sepsis on occurrence of purulent meningitis
-
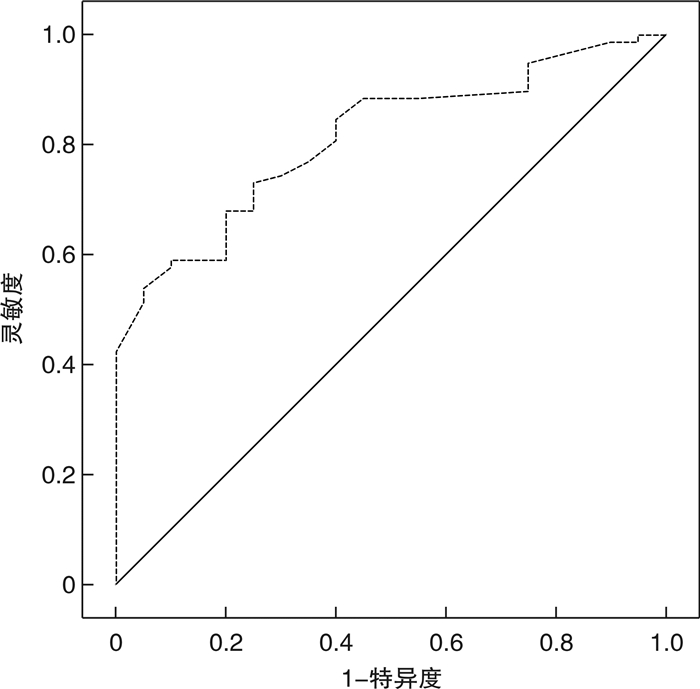
摘要: 目的 分析早发型新生儿败血症(early-onset neonatal sepsis,EOS)患儿血小板计数(PLT)对化脓性脑膜炎发生的预测效能,探讨EOS患儿化脓性脑膜炎发生的预测因子。方法 使用前瞻性队列研究的方法,入选2019年12月—2022年1月在重庆市开州区人民医院诊断为EOS的104例新生儿作为研究对象,以明确诊断EOS至疾病完全康复为观察终点,统计化脓性脑膜炎发生情况。入院检查项目包括血常规参数、C反应蛋白(CRP)、降钙素原(PCT)、白细胞介素(IL)-6等炎症指标。使用logistic回归分析PLT与EOS患儿化脓性脑膜炎发生的关系,绘制受试者工作特征(ROC)曲线,检验PLT对EOS患儿化脓性脑膜炎发生的预测效能。结果 共收录104例EOS患儿,治疗期间6例符合剔除标准,最终98例完成研究。98例新生儿PLT检测结果为(100.09±14.81)×109/L,发生化脓性脑膜炎20例,发生率为20.41%(20/98)。PLT < 100×109/L的患儿中性粒细胞,血清CRP、PCT、IL-6水平均高于PLT≥100×109/L的患儿,淋巴细胞低于PLT≥100×109/L的患儿,化脓性脑膜炎发生率高于PLT≥100×109/L的患儿,差异有统计学意义(P < 0.05)。Logistic回归数据显示,PLT减少,CRP、PCT高表达均能够增加EOS患儿并发化脓性脑膜炎的风险(P < 0.05)。ROC曲线数据显示,PLT预测EOS患儿化脓性脑膜炎发生风险的曲线下面积(AUC)为0.813,具有一定预测价值。结论 EOS患儿PLT减少能够导致治疗期间化脓性脑膜炎风险增加,检测PLT能够预测EOS并发化脓性脑膜炎的风险。Abstract: Objective To analyze the predictive effect of platelet count on the occurrence of purulent meningitis in the children with early-onset neonatal sepsis(EOS), and explore the predictive factors of the occurrence of purulent meningitis in the children with EOS.Methods A prospective cohort study was used to select 104 neonates who were diagnosed with EOS in the People's Hospital of Kaizhou District of Chongqing from December 2019 to January 2022 as the study objects. The observation endpoint was from clear diagnosis of EOS to complete recovery of the disease, and the incidence of purulent meningitis was counted. The items of admission examination include blood routine parameters, C-reactive protein(CRP), procalcitonin(PCT), interleukin(IL) -6 and other inflammatory indicators. Logistic regression was used to analyze the relationship between platelet count and the occurrence of purulent meningitis in the children with EOS, draw the ROC curve of subjects, and test the predictive efficacy of platelet count on the occurrence of purulent meningitis in children with EOS.Results Totally 104 EOS children were included. During the treatment, 6 patients met the exclusion criteria, and 98 patients completed the study. The platelet count of 98 neonates was(100.09±14.81)×109/L, 20 cases had purulent meningitis, the incidence was 20.41%(20/98). In children with platelet count < 100×109/L, neutrophils(NE), serum CRP, PCT, and IL-6 levels were higher than those with platelets≥100×109/L, lymphocyte and the incidence of purulent meningitis were lower than those with platelets≥100×109/L. The difference was statistically significant(P < 0.05). Logistic regression data showed that decreased platelet count and high expression of CRP and PCT could increase the risk of purulent meningitis in the children with EOS(P < 0.05). The ROC curve data showed that the area under the curve(AUC) of platelet count predicting the risk of purulent meningitis in the children with EOS was 0.813, which had certain predictive value.Conclusion The decrease of platelet count in the children with EOS can increase the risk of purulent meningitis during treatment, and the detection of platelet count can predict the risk of EOS complicated with purulent meningitis.
-
Key words:
- early-onset neonatal sepsis /
- purulent meningitis /
- platelet /
- predictive effectiveness
-

-
表 1 不同PLT检测结果的EOS患儿一般资料比较
一般资料 PLT < 100×109/L(n=50) PLT≥100×109/L(n=48) t/Z/χ2 P 性别/例(%) 1.974 0.160 男 34(68.00) 26(54.17) 女 16(32.00) 22(45.83) 胎龄/周 34.00(33.00,37.00) 33.50(33.00,36.50) 1.251 0.211 分娩方式/例(%) 0.352 0.553 剖宫产 40(80.00) 36(75.00) 自然分娩 10(20.00) 12(25.00) 出生体重/g 2 285.41±247.58 2 196.19±238.67 1.815 0.073 PROM≥18 h/例(%) 1.640 0.200 是 27(54.00) 32(66.67) 否 23(46.00) 16(33.33) 感染病原谱/例(%) 2.234 0.525 GBS 22(44.00) 15(31.25) 大肠埃希菌 15(30.00) 18(37.50) 李斯特菌 6(12.00) 9(18.75) 铜绿假单胞菌 7(14.00) 6(12.50) WBC/(×109/L) 27.50±4.16 26.75±4.35 0.941 0.349 RBC/(×1012/L) 4.00(4.00,4.00) 4.00(4.00,4.25) 1.069 0.285 NE/% 70.50±6.62 67.46±7.66 2.107 0.038 嗜酸性粒细胞/% 4.43±0.51 4.59±0.46 1.642 0.104 淋巴细胞/% 21.07±2.81 22.17±2.40 2.075 0.041 Hb/(g/L) 131.42±12.65 132.72±15.42 0.460 0.647 CRP/(mg/L) 12.64±1.65 11.42±1.56 3.772 < 0.001 PCT/(ng/mL) 14.21±2.02 11.42±1.56 2.430 0.018 IL-6/(pg/mL) 241.31±17.86 231.03±19.48 2.726 0.008 化脓性脑膜炎/例(%) 5.782 0.016 是 15(30.00) 5(10.42) 否 35(70.00) 43(89.58) 表 2 PLT对EOS并发化脓性脑膜炎的影响
项目 β SE Wald P OR 95%CI PLT -0.094 0.043 4.781 0.029 0.910 0.736~0.990 NE 0.092 0.092 1.003 0.317 1.097 0.916~1.313 淋巴细胞 -0.523 0.273 3.668 0.055 0.593 0.347~1.012 CRP 0.866 0.403 4.609 0.032 2.377 1.078~5.242 PCT 0.866 0.425 4.145 0.042 2.378 1.033~5.475 IL-6 0.037 0.031 1.374 0.241 1.037 0.976~1.103 常量 -20.353 13.146 2.397 0.122 - - -
[1] Glaser MA, Hughes LM, Jnah A, et al. Neonatal Sepsis: a review of pathophysiology and current management strategies[J]. Adv Neonatal Care, 2021, 21(1): 49-60. doi: 10.1097/ANC.0000000000000769
[2] 张敏, 杨帆, 程玲, 等. 82例新生儿败血症病原学与临床特点[J]. 中华医院感染学杂志, 2021, 31(12): 1791-1795. https://www.cnki.com.cn/Article/CJFDTOTAL-ZHYY202112007.htm
[3] 中华医学会儿科学分会新生儿学组, 中国医师协会新生儿科医师分会感染专业委员会. 新生儿败血症诊断及治疗专家共识(2019年版)[J]. 中华儿科杂志, 2019, 57(4): 252-257. doi: 10.3760/cma.j.issn.0578-1310.2019.04.005
[4] Panda SK, Nayak MK, Thangaraj J, et al. Platelet parameters as a diagnostic marker in early diagnosis of neonatal sepsis-Seeking newer answers for older problems[J]. J Family Med Prim Care, 2022, 11(5): 1748-1754. doi: 10.4103/jfmpc.jfmpc_1271_21
[5] 林垦, 刘鹏, 杨锋, 等. 新生儿败血症病原菌分布及血清炎性因子、血小板参数诊断价值分析[J]. 宁夏医科大学学报, 2020, 42(7): 701-704. https://www.cnki.com.cn/Article/CJFDTOTAL-XNXY202007012.htm
[6] Arabdin M, Khan A, Zia S, et al. Frequency and severity of thrombocytopenia in neonatal Sepsis[J]. Cureus, 2022, 14(2): e22665.
[7] Hodgins C. Apgar score[J]. J Obstet Gynecol Neonatal Nurs, 1997, 26(1): 15-16.
[8] Vilnits AA, Skripchenko NV, Gorelik EY, et al. Possibilities for optimizing the pathogenetic therapy of purulent meningitis in children[J]. Zh Nevrol Psikhiatr Im S S Korsakova, 2019, 119(12): 46-50. doi: 10.17116/jnevro201911912146
[9] 郑孟秋, 曹传顶, 丁颖, 等. 81例新生儿化脓性脑膜炎临床分析[J]. 中国感染控制杂志, 2020, 19(5): 440-446. https://www.cnki.com.cn/Article/CJFDTOTAL-GRKZ202005009.htm
[10] 张战强, 张改玲, 李文倩, 等. 血小板数值与CD19-CAR-T细胞治疗难治/复发急性B淋巴细胞白血病疗效的关系[J]. 临床血液学杂志, 2022, 35(9): 674-676, 679. https://lcxy.whuhzzs.com/article/doi/10.13201/j.issn.1004-2806.2022.09.013
[11] Kerris EWJ, Hoptay C, Calderon T, et al. Platelets and platelet extracellular vesicles in hemostasis and sepsis[J]. J Investig Med, 2020, 68(4): 813-820.
[12] Al Saleh K, AlQahtani RM. Platelet count patterns and patient outcomes in sepsis at a tertiary care center[J]. Medicine, 2021, 100(18): e25013.
[13] Menard CE, Kumar A, Houston DS, et al. Evolution and impact of thrombocytopenia in septic shock: a retrospective cohort study[J]. Crit Care Med, 2019, 47(4): 558-565.
[14] 岳福仁, 闫瑞振, 魏志斌, 等. 血流感染患者血小板参数动态变化及其预后价值[J]. 临床检验杂志, 2021, 39(7): 514-516. https://www.cnki.com.cn/Article/CJFDTOTAL-LCJY202107005.htm
[15] Dib PRB, Quirino-Teixeira AC, Merij LB, et al. Innate immune receptors in platelets and platelet-leukocyte interactions[J]. J Leukoc Biol, 2020, 108(4): 1157-1182.
[16] 周南君, 汤展宏. 血小板减少症对脓毒症患者预后的影响: 系统回顾和Meta分析[J]. 中国实用内科杂志, 2021, 41(3): 238-242, 256. https://www.cnki.com.cn/Article/CJFDTOTAL-SYNK202103016.htm
-




 下载:
下载: