Predictive value of expression of IL-7 and NK cells in peripheral blood of children with acute B-lymphocytic leukemia on effect of chemotherapy
-
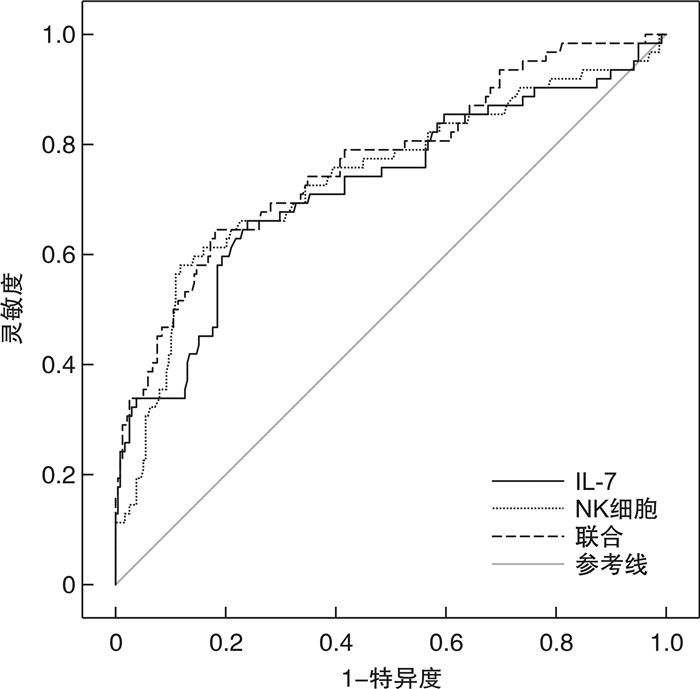
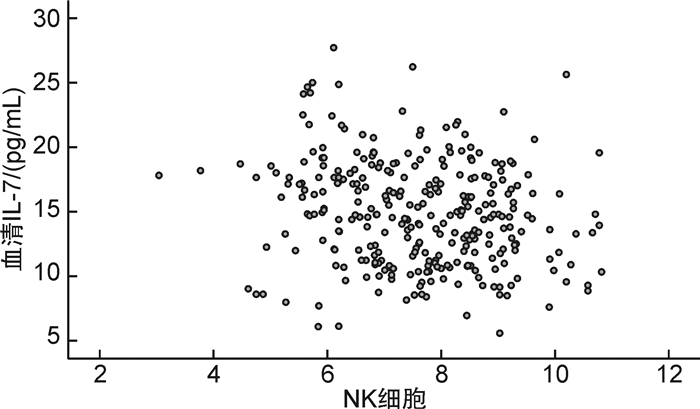
摘要: 目的 分析急性B淋巴细胞白血病(B-ALL)患儿外周血白细胞介素-7(IL-7)、自然杀伤(NK)细胞表达对化疗效果的预测价值,为临床治疗B-ALL提供经验指导。方法 采用前瞻性研究方法,研究对象来源2015年4月—2020年2月治疗的B-ALL患儿,所有患儿均采用VDLD方案(长春新碱+柔红霉素+门冬酰胺酶+地塞米松)化疗,化疗前检测外周血IL-7、NK细胞水平,化疗33 d后统计化疗效果。比较不同化疗效果中B-ALL患儿性别、年龄、临床危险度、IL-7、NK细胞等资料,分析B-ALL患儿外周血IL-7、NK细胞表达对化疗效果的预测价值。结果 本研究共纳入308例B-ALL患儿进行研究,300例按规定完成33 d的规范治疗,其中完全缓解140例(46.67%),部分缓解98例(32.67%),疾病进展36例(12.00%),疾病复发26例(8.67%)。缓解组白细胞计数、IL-7低于未缓解组,纤维蛋白原、D-二聚体及NK细胞水平高于未缓解组,差异有统计学意义(P < 0.05)。经点二列相关性分析显示,B-ALL患儿IL-7水平与化疗效果呈正相关(r=0.350,P < 0.05),NK细胞水平与化疗效果呈负相关(r=-0.342,P < 0.05)。经Pearson相关性分析显示,B-ALL患儿外周血IL-7与NK细胞呈负相关(r=-0.191,P < 0.05);绘制受试者工作特征曲线,结果显示化疗前IL-7、NK细胞单独及联合预测B-ALL患儿化疗效果的曲线下面积分别为0.722、0.739、0.768,均有一定预测价值,当IL-7与NK细胞临界值分别取15.590 pg/mL、7.185时预测价值最佳。结论 B-ALL患儿外周血IL-7水平升高、NK细胞水平降低,外周血IL-7、NK细胞可作为化疗效果的预测指标。
-
关键词:
- 急性B淋巴细胞白血病 /
- 白细胞介素-7 /
- 自然杀伤细胞 /
- 化疗 /
- 预测
Abstract: Objective To analyze the predictive value of the expression of interleukin-7(IL-7) and natural killer(NK) cells in the peripheral blood of children with acute B-lymphocytic leukemia(B-ALL) on the effect of chemotherapy, so as to provide experience guidance for clinical treatment of B-ALL.Methods A prospective study was conducted. The subjects were children with B-ALL who were treated in the Affiliated Children's Hospital of Suzhou University from April 2015 to February 2020. All children were treated with VDLD regimen(vincristine+daunorubicin+asparaginase+dexamethasone). The levels of IL-7 and NK cells in peripheral blood were detected before chemotherapy, and the chemotherapy effect was counted 33 days after chemotherapy. The sex, age, clinical risk, IL-7, NK cells and other data of children with B-ALL with different chemotherapy effects were compared, and the predictive value of the expression of IL-7, NK cells in the peripheral blood of children with B-ALL on the chemotherapy effect were analyzed.Results A total of 308 children with B-ALL were included in this study. 300 patients completed the standardized treatment for 33 days according to the regulations. Among the 300 children, 140(46.67%) had complete remission, 98(32.67%) had partial remission, 36(12.00%) had disease progression, and 26(8.67%) had disease recurrence. The WBC count and IL-7 in remission group were lower than those in non remission group, while the levels of fibrinogen, D-dimer and NK cells in remission group were higher than those in non remission group, with a statistical significant difference(P < 0.05). The point binary correlation analysis showed that the level of IL-7 in children with B-ALL was correlated with the effect of chemotherapy(r=0.350, P < 0.05), and the level of NK cells was negatively correlated with the effect of chemotherapy(r=-0.342, P < 0.05). Pearson correlation analysis showed that there was a negative correlation between IL-7 and NK cells in peripheral blood of children with B-ALL(r=-0.191, P < 0.05). The ROC curve of the subjects was drawn. The results showed that the AUC of IL-7 and NK cells alone and jointly predicting the chemotherapy effect of children with B-ALL before chemotherapy were 0.722, 0.739 and 0.768, respectively, which had certain predictive value. When the critical values of IL-7 and NK cells were 15.590 pg/mL and 7.185, respectively, the predictive value was the best.Conclusion The levels of IL-7 and NK cells in peripheral blood of children with B-ALL increased and decreased, respectively. IL-7 and NK cells in peripheral blood could be used as predictive indicators of chemotherapy effect.-
Key words:
- acute B-lymphocytic leukemia /
- interleukin-7 /
- natural killer cells /
- chemotherapy /
- prediction
-

-
表 1 基线资料及实验室指标对比
组别 缓解组(n=238) 未缓解组(n=62) 统计值 P 性别/例(%) χ2=0.732 0.392 男 116(48.74) 34(54.84) 女 122(51.26) 28(45.16) 年龄/例(%) χ2=0.974 0.324 ≥8岁 93(39.08) 20(32.26) < 8岁 145(60.92) 42(67.74) 体重/kg 24.58±2.86 24.73±2.90 t=0.366 0.714 临床危险度/例(%) Z=0.223 0.823 低危 46(19.33) 11(17.74) 中危 102(42.86) 27(43.55) 高危 90(37.81) 24(38.71) 血小板计数/(×109/L) 93.02±8.13 92.48±8.20 t=0.465 0.642 红细胞计数/(×1012/L) 4.68±0.65 4.72±0.70 t=0.321 0.748 白细胞计数/(×109/L) 55.56±6.75 65.10±6.58 t=9.956 < 0.001 中性粒细胞计数/(×109/L) 1.06±0.23 1.10±0.19 t=1.043 0.298 血红蛋白/(g/L) 75.46±5.42 74.10±5.48 t=1.754 0.080 PT/s 12.51±1.02 12.58±0.98 t=0.484 0.629 APTT/s 31.84±2.02 31.75±1.96 t=0.313 0.754 TT/s 14.79±1.24 14.83±1.28 t=0.169 0.866 FIB/(g/L) 2.80±0.50 2.45±0.46 t=4.964 < 0.001 D-D/(μg/L) 162.85±20.54 156.74±20.63 t=2.085 0.038 IL-7/(pg/mL) 14.15±3.49 17.66±4.82 t=6.458 < 0.001 NK细胞 7.85±1.25 6.66±1.57 t=6.280 < 0.001 表 2 IL-7、NK细胞与化疗效果的关系分析
指标 r P IL-7 0.350 < 0.001 NK细胞 -0.342 < 0.001 表 3 化疗前IL-7、NK细胞单独及联合对化疗效果的预测价值
指标 AUC AUC的95%CI SE P 最佳阈值 特异度 灵敏度 约登指数 IL-7 0.722 0.643~0.801 0.040 < 0.001 15.590 pg/mL 0.647 0.710 0.357 NK细胞 0.739 0.661~0.817 0.040 < 0.001 7.185 0.676 0.694 0.370 联合 0.768 0.696~0.839 0.036 < 0.001 - 0.651 0.742 0.393 -
[1] 蔡玉丽, 邹尧, 陈晓娟, 等. 982例儿童急性淋巴细胞白血病流行病学研究[J]. 中国实验血液学杂志, 2020, 28(2): 371-376. doi: 10.19746/j.cnki.issn1009-2137.2020.02.003
[2] 田云, 艾昊, 纪旭, 等. 维奈托克联合TKI及含地塞米松小剂量化疗对复发/难治Ph +急性B淋巴细胞白血病的疗效分析[J]. 中华医学杂志, 2022, 102(10): 745-748. doi: 10.3760/cma.j.cn112137-20210728-01676
[3] 张战强, 张改玲, 李文倩, 等. 血小板数值与CD19-CAR-T细胞治疗难治/复发急性B淋巴细胞白血病疗效的关系[J]. 临床血液学杂志, 2022, 35(9): 674-676, 679. https://lcxy.whuhzzs.com/article/doi/10.13201/j.issn.1004-2806.2022.09.013
[4] Ribeiro D, Melão A, van Boxtel R, et al. STAT5 is essential for IL-7-mediated viability, growth, and proliferation of T-cell acute lymphoblastic leukemia cells[J]. Blood Adv, 2018, 2(17): 2199-2213. doi: 10.1182/bloodadvances.2018021063
[5] Sportoletti P, de Falco F, del Papa B, et al. NK cells in chronic lymphocytic leukemia and their therapeutic implications[J]. Int J Mol Sci, 2021, 22(13): 6665. doi: 10.3390/ijms22136665
[6] 中华医学会儿科学分会血液学组, 《中华儿科杂志》编辑委员会. 儿童急性淋巴细胞白血病诊疗建议(第四次修订)[J]. 中华儿科杂志, 2014, 52(9): 641-644. https://www.cnki.com.cn/Article/CJFDTOTAL-ZHEK200605032.htm
[7] 沈悌, 赵永强. 血液病诊断及疗效标准[M]. 4版. 北京: 科学出版社, 2018: 91-95.
[8] 宋妤, 薛彦. IL-7通过调节CD127表达调控脓毒症患者CD8+T细胞的体外活性[J]. 中华微生物学和免疫学杂志, 2022, 42(4): 293-301. https://www.cnki.com.cn/Article/CJFDTOTAL-SGLC202206004.htm
[9] 杨丽葭, 刘文洁, 孙倩, 等. NK细胞绝对值对初诊慢性粒细胞白血病慢性期患者TKI治疗反应的预测价值[J]. 南京医科大学学报(自然科学版), 2020, 40(7): 991-995. https://www.cnki.com.cn/Article/CJFDTOTAL-NJYK202205014.htm
[10] Buffière A, Uzan B, Aucagne R, et al. T-cell acute lymphoblastic leukemia displays autocrine production of Interleukin-7[J]. Oncogene, 2019, 38(48): 7357-7365. doi: 10.1038/s41388-019-0921-4
[11] Locatelli F, Pende D, Falco M, et al. NK cells mediate a crucial graft-versus-leukemia effect in haploidentical-HSCT to cure high-risk acute leukemia[J]. Trends Immunol, 2018, 39(7): 577-590.
[12] Almeida ARM, Neto JL, Cachucho A, et al. Interleukin-7 receptor α mutational activation can initiate precursor B-cell acute lymphoblastic leukemia[J]. Nat Commun, 2021, 12(1): 7268.
[13] Zhang XY, Tu HJ, Yang YZ, et al. Bone marrow-derived mesenchymal stromal cells promote resistance to tyrosine kinase inhibitors in chronic myeloid leukemia via the IL-7/JAK1/STAT5 pathway[J]. J Biol Chem, 2019, 294(32): 12167-12179.
[14] 苌哲宗, 余红岚, 费樱, 等. 儿童急性淋巴细胞白血病患者外周血IL-7、TK1、LDH水平变化的临床意义及其相关性研究[J]. 贵州医药, 2018, 42(4): 401-403. https://www.cnki.com.cn/Article/CJFDTOTAL-GZYI201804006.htm
[15] 曹勋红, 王志东, 孙于谦, 等. 两种扩增体系NK细胞生物学特性比较及治疗异基因造血干细胞移植后白血病复发的初步研究[J]. 中华血液学杂志, 2022, 43(5): 400-407.
[16] 金婷, 王芳, 王利. 老年AML微移植治疗前后NK细胞比例与IFN-γ浓度的相关性研究[J]. 重庆医学, 2021, 50(17): 2963-2967. https://www.cnki.com.cn/Article/CJFDTOTAL-CQYX202117019.htm
[17] 刘露, 陈肖, 金慧敏, 等. 急性髓系白血病患者NK细胞表达及功能变化研究[J]. 中国实验血液学杂志, 2022, 30(1): 49-55. https://www.cnki.com.cn/Article/CJFDTOTAL-XYSY202201008.htm
-




 下载:
下载: