Analysis of factors associated with high frequency transfusion in very low and ultra-low birth weight infants
-
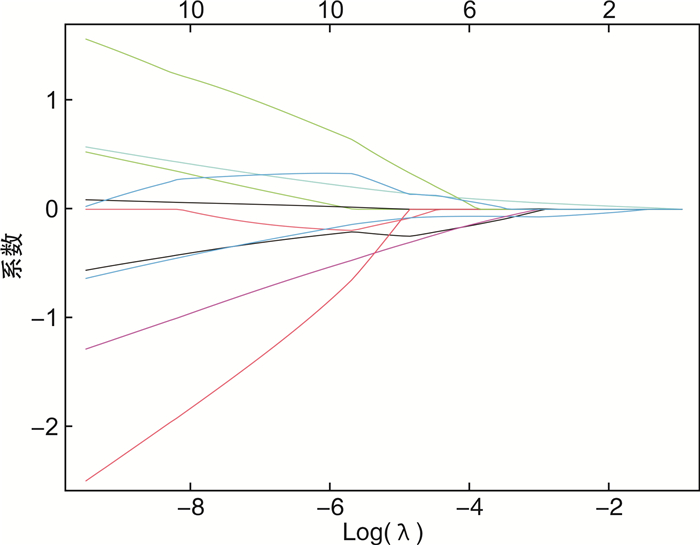
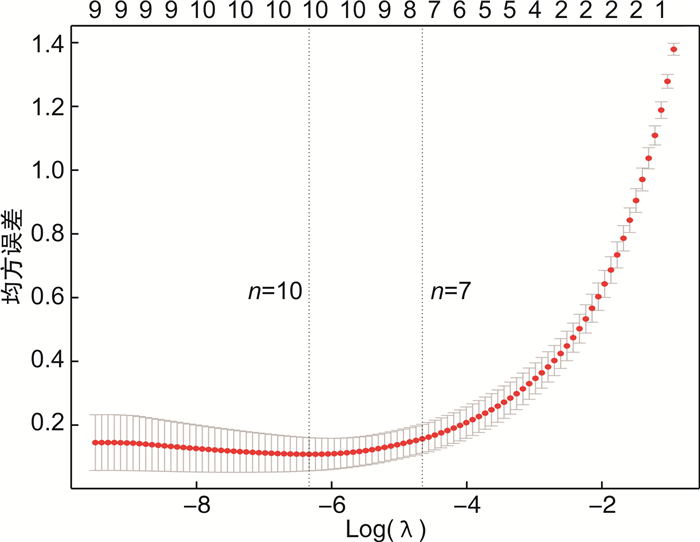
摘要: 目的 分析影响极低和超低出生体重儿高频次输血的相关危险因素,为此类患儿临床输血治疗提供帮助。方法 回顾性分析2019年1月—2022年6月出生并输血的极低出生体重儿(very low birth weight infant,VLBWI)和超低出生体重儿(extremely low birth weight infant,ELBWI)临床资料。根据输血次数分为普通组(输血次数≤3次)和高频次组(输血次数>3次),收集2组患儿的一般资料、住院期间疾病发生和治疗情况及母亲一般情况,比较2组差异,通过Lasso回归结合logistic回归分析影响VLBWI和ELBWI高频次输血的危险因素。结果 本研究共纳入142例,其中普通组79例,高频次组63例。2组间出生体重、胎龄、阿氏评分1 min、阿氏评分5 min、出生时血红蛋白、住院时长、首次输血日龄、首次输血前抽血次数、累计输血量、平均输血量、新生儿败血症、早产儿视网膜病变(retinopathy of prematurity,ROP)、新生儿脑病、支气管肺发育不良(bronchopulmonary dysplasia,BPD)比较,差异均有统计学意义(P < 0.05)。Lasso回归筛选出7个显著变量,即胎龄、阿氏评分1 min、首次输血日龄、累计输血量、平均输血量、早产儿脑病、BPD。多因素logistic回归结果显示,首次输血日龄≥14 d(OR=0.036,95%CI 0.012~0.104,P < 0.01)是VLBWI和ELBWI高频次输血的保护因素,BPD(OR=6.275,95%CI 2.101~18.742,P < 0.01)是VLBWI和ELBWI高频次输血的独立危险因素。结论 本回顾性研究提示首次输血日龄≥14 d是VLBWI和ELBWI高频次输血的保护因素,BPD是VLBWI和ELBWI高频次输血的独立危险因素。Abstract: Objective To analyze the risk factors related to high frequency blood transfusion in very low and ultra-low birth weight infants, and provide help for clinical blood transfusion treatment of such infants.Methods Clinical data were retrospectively analyzed for very low birth weight infants(VLBWI) and ultra-low birth weight infants(ELBWI) that were born and transfused in our hospital from January 2019 to June 2022. According to the frequency of transfusion, they were divided into normal group(≤3 times of transfusion) and high frequency group(>3 times of transfusion), and the general data, disease occurrence and treatment during hospitalization, and general condition of their mothers were collected for both groups of preterm infants. The differences between the two groups were compared, and the risk factors influencing high frequency transfusions in VLBWI and ELBWI were analyzed by Lasso regression combined with logistic regression.Results A total of 142 cases were included in this study, including 79 cases in the normal group and 63 cases in the high frequency group. Birth weight, gestational age, Alzheimer's score at 1 minute, Alzheimer's score at 5 minutes, hemoglobin at birth, length of hospitalization, date at first transfusion day, number of blood draws before first transfusion, cumulative transfusion volume, mean transfusion volume, neonatal sepsis, retinopathy of prematurity(ROP), neonatal encephalopathy and bronchial pulmonary dysplasia(BPD) were statistically significant(all P < 0.05). Lasso regression selected seven significant variables, namely gestational age, Alzheimer's score at 1 minute, date at first transfusion day, cumulative transfusion volume, mean transfusion volume, encephalopathy of prematurity, and BPD. Multifactorial logistic regression showed that the date of first transfusion day ≥14 days(OR=0.036, 95%CI 0.012-0.104, P < 0.01) was a protective factor for high frequency transfusion in VLBWI and ELBWI, and BPD(OR=6.275, 95%CI 2.101-18.742, P < 0.01) was an independent risk factor for high frequency transfusion in VLBWI and ELBWI.Conclusion This retrospective study suggested that the date of first transfusion day ≥14 days might be a protective factor for high frequency transfusion in VLBWI and ELBWI, and BPD might be an independent risk factor for high frequency transfusion in VLBWI and ELBWI.
-
Key words:
- anemia of prematurity /
- blood transfusion /
- bronchopulmonary dysplasia
-

-
表 1 2组患儿一般资料比较
变量 普通组(79例) 高频次组(63例) Z/χ2 P 出生体重/g 1 300(1 210,1 390) 1 130(970,1 250) -5.02 < 0.01 胎龄/周 31.00(29.57,31.71) 29.57(28.71,30.43) -4.60 < 0.01 男婴/例(%) 27(34.18) 29(46.03) 2.06 >0.05 双胎/例(%) 13(16.46) 11(17.46) 0.03 >0.05 阿氏评分1 min/例 9(8,9) 8(7,9) -3.52 < 0.01 阿氏评分5 min/例 9(9,9) 9(8,9) -3.09 < 0.01 出生时Hb/(g/L) 164(156,179) 157(146,171) -2.55 < 0.05 住院时长/d 39(33,45) 58(45,70) -7.07 < 0.01 表 2 2组患儿住院治疗情况比较
变量 普通组(79例) 高频次组(63例) Z/t/χ2 P 首次输血日龄/d 20(15,23) 7(4,11) -7.94 < 0.01 首次输血前抽血次数 17(14,19) 13(10,15) -5.99 < 0.01 累计输血量/mL 54(48,60) 114(99,144) -10.10 < 0.01 平均输血量/mL 25.88±4.10 22.84±3.67 4.60 < 0.01 新生儿肺炎/例(%)* 73(92.41) 62(98.41) - >0.05 新生儿败血症/例(%) 17(21.52) 38(60.32) 22.23 < 0.01 NEC/例(%)* 2(2.53) 3(4.76) - >0.05 ROP/例(%) 12(15.19) 32(50.79) 20.78 < 0.01 早产儿脑病/例(%) 49(62.03) 50(79.37) 4.99 < 0.05 BPD/例(%) 24(30.38) 50(79.37) 33.70 < 0.01 *采用Fisher精确检验。 表 3 2组患儿母亲一般资料比较
变量 普通组(79例) 高频次组(63例) Z/χ2 P 年龄/岁 31(28,33) 31(29,34) -0.35 >0.05 孕次/次 2(1,3) 2(1,3) -1.71 >0.05 产次/次 1(1,2) 1(1,2) -0.61 >0.05 人工助孕/例(%) 8(10.13) 8(12.70) 0.23 >0.05 妊娠期贫血/例(%) 22(27.85) 19(30.16) 0.09 >0.05 胎膜早破/例(%) 24(30.38) 18(28.57) 0.05 >0.05 胎盘早剥/例(%) 13(16.46) 12(19.05) 0.16 >0.05 妊娠期高血压/例(%) 40(50.63) 23(36.51) 2.83 >0.05 前置胎盘/例(%)* 2(2.53) 1(1.59) - >0.05 妊娠期肝内胆汁淤积症/例(%)* 6(7.59) 4(6.35) - >0.05 胎儿宫内窘迫/例(%) 14(17.72) 19(30.16) 3.04 >0.05 *采用Fisher精确检验。 表 4 logistic回归变量赋值情况
变量 赋值 胎龄 < 30周=0,≥30周=1 阿氏评分1 min < 8分=0,≥8分=1 首次输血日龄 < 14 d=0,≥14 d=1 早产儿脑病 否=0,是=1 BPD 否=0,是=1 表 5 logistic回归分析影响VLBWI和ELBWI高频次输血的因素
影响因素 β SE Wald P OR 95%CI 胎龄 -0.243 0.533 0.208 0.648 0.784 0.276~2.228 阿氏评分1 min -0.322 0.681 0.223 0.637 0.725 0.191~2.754 首次输血日龄 -3.327 0.543 37.466 < 0.001 0.036 0.012~0.104 早产儿脑病 0.270 0.586 0.212 0.645 1.309 0.416~4.126 BPD 1.837 0.558 10.824 0.001 6.275 2.101~18.742 常量 0.400 0.830 0.233 0.630 1.492 - -
[1] Keir AK, Yang J, Harrison A, et al. Temporal changes in blood product usage in preterm neonates born at less than 30 weeks' gestation in Canada[J]. Transfusion, 2015, 55(6): 1340-1346. doi: 10.1111/trf.12998
[2] Ghirardello S, Dusi E, Cortinovis I, et al. Effects of red blood cell transfusions on the risk of developing complications or death: an observational study of a cohort of very low birth weight infants[J]. Am J Perinatol, 2017, 34(1): 88-95.
[3] 李琦, 李宇丹, 许婧. 早产儿贫血与输血治疗相关因素分析[J]. 中国输血杂志, 2022, 35(6): 618-621. https://www.cnki.com.cn/Article/CJFDTOTAL-BLOO202206007.htm
[4] 纪卫华, 王金元, 王红宇. 首次输血日龄与极低和超低出生体重儿近期主要并发症的相关性[J]. 中国妇幼健康研究, 2021, 32(9): 1326-1330. https://www.cnki.com.cn/Article/CJFDTOTAL-SANE202109017.htm
[5] Raffaella C, Laura S, Daniele T. Anemia and transfusion in the neonate[C]//Seminars in Fetal and Neonatal Medicine: Elsevier, 2016: 2-9.
[6] 林燕, 张妮妮, 谢小敏, 等. 超低出生体重儿及超早产儿输血治疗的相关危险因素分析[J]. 中国妇幼健康研究, 2020, 31(1): 11-15. https://www.cnki.com.cn/Article/CJFDTOTAL-SANE202001003.htm
[7] 宗海峰, 冯琪. 早产儿输血相关合并症及输血策略[J]. 中华围产医学杂志, 2015(3): 234-237.
[8] 徐春彩, 朱佳骏, 朱以琳, 等. 极低出生体质量儿输血相关危险因素分析[J]. 临床儿科杂志, 2017, 35(9): 641-644. https://www.cnki.com.cn/Article/CJFDTOTAL-LCAK201709001.htm
[9] 王星, 王雅茹, 李亭, 等. 233例儿童非传染性输血不良反应相关因素分析[J]. 临床血液学杂志, 2021, 34(6): 399-402. https://lcxy.whuhzzs.com/article/doi/10.13201/j.issn.1004-2806.2021.06.005
[10] 江苏省新生儿重症监护病房母乳质量改进临床研究协作组. 多中心回顾性分析极低及超低出生体重儿支气管肺发育不良的临床特点及高危因素[J]. 中华儿科杂志, 2019, 57(1): 33-39.
[11] 于洋, 殷其改. 胎龄 < 31周的早产儿发生支气管肺发育不良危险因素的分析[J]. 当代医药论丛, 2020, 18(21): 152-154.
[12] 段灵, 陈萍, 胡红兵. 极低出生体重儿红细胞输注的危险因素分析[J]. 临床血液学杂志, 2022, 35(12): 867-871. https://lcxy.whuhzzs.com/article/doi/10.13201/j.issn.1004-2806.2022.12.006
-




 下载:
下载: