Preliminary study on clinical significance of iron metabolism indexes in myelodysplastic syndrome
-
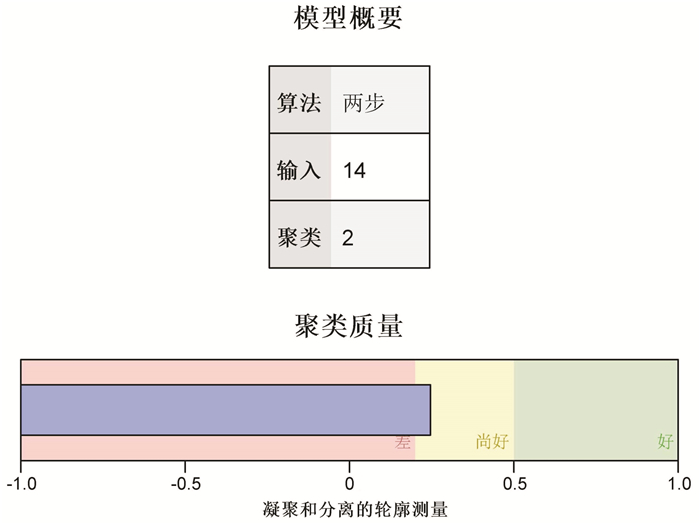
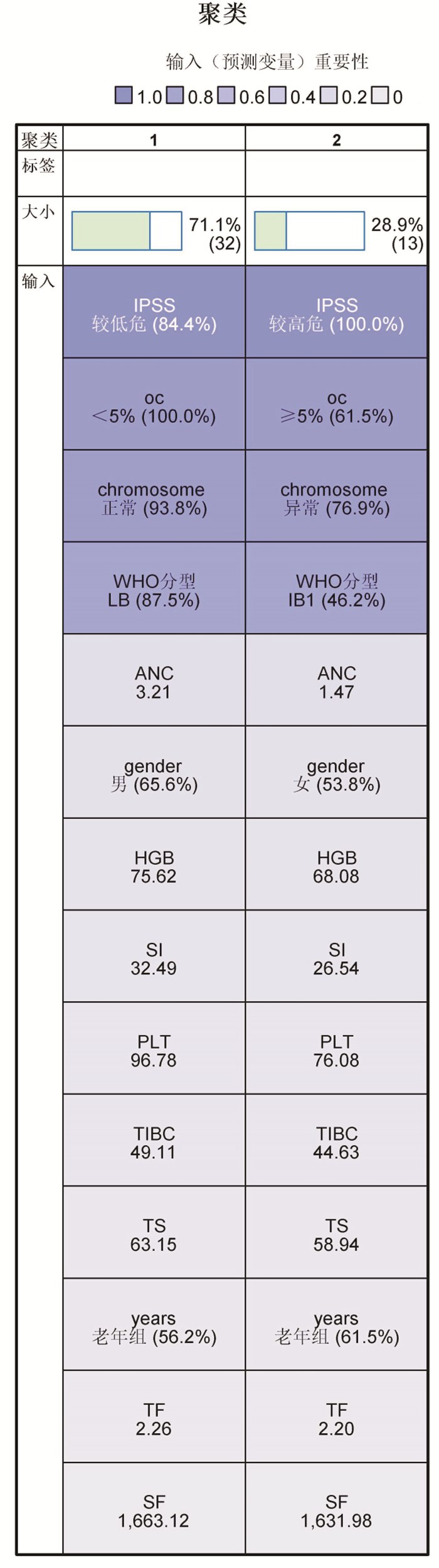
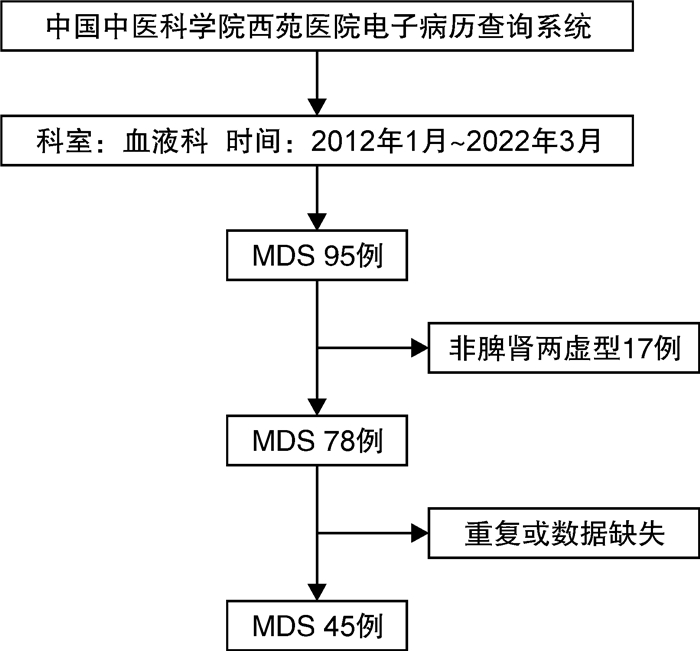
摘要: 目的 通过临床回顾性分析,研究不同年龄层骨髓增生异常综合征(MDS)的铁代谢指标:血清铁(SI)、血清铁蛋白(SF)、血清转铁蛋白(TF)、总铁结合力(TIBC)和血清铁饱和度(TS)与年龄分层、WHO分型、IPSS-R评分及与血红蛋白(HGB)、血小板计数(PLT)、绝对中性粒细胞计数(ANC)的变化规律和相关关系。方法 选取2012年1月—2022年3月就诊的45例MDS患者,分析铁代谢指标与血常规和铁代谢指标之间的相关性,并聚类分析临床资料的关系。结果 ① 老年组MDS患者SF较中青年组高(P < 0.05);②中青年组MDS-LB患者较MDS-IB1患者的TF和TIBC高(P < 0.05);③老年组的较低危比较高危患者的TF高(P < 0.05);④MDS患者的HGB水平与SF、TS呈负相关,与TF、TIBC呈正相关(P < 0.05)。ANC水平与TF、TIBC呈负相关(P < 0.05);⑤MDS患者通过临床资料可分为较低危和较高危两类。结论 ① 老年MDS患者铁负荷较高,预后较差;②中青年MDS患者铁转运能力及对铁过载的耐受能力强;③HGB低的患者铁负荷更加严重,ANC低的患者铁负荷可能较低;④TF可能参与对MDS患者铁过载评价和预后的评估。Abstract: Objective To study the changes and correlations of serum iron(SI), serum ferritin(SF), serum transferrin(TF), total iron binding capacity(TIBC), serum iron saturation(TS) and age stratification, WHO classification, IPSS-R score and hemoglobin(HGB), platelet(PLT) and absolute neutrophil count(ANC) in different age groups of myelodysplastic syndrome(MDS) through clinical retrospective analysis.Methods A total of 45 patients with MDS from January 2012 to March 2022 were selected to analyze the correlation between iron metabolism index and blood routine and iron metabolism index, and cluster analysis of clinical data.Results ① The SF of MDS patients in the elderly group was higher than that in the young and middle-aged group(P < 0.05). ②The TF and TIBC of MDS-LB patients in young and middle-aged group were higher than those of MDS-IB1 patients(P < 0.05). ③The TF of low risk patients was higher than that of high risk patients in the elderly group(P < 0.05). ④The level of HGB in patients with MDS was negatively correlated with SF and TS, and positively correlated with TF and TIBC(P < 0.05). The level of ANC was negatively correlated with TF and TIBC(P < 0.05). ⑤According to the clinical data, patients with MDS could be divided into two categories: lower risk and higher risk.Conclusion ① The iron load of elderly patients with MDS was higher and the prognosis was poor. ②Young and middle-aged patients with MDS had strong ability of iron transport and tolerance to iron overload. ③The iron load of patients with low HGB was more severe, and the iron load of patients with low ANC might be lower. ④TF might be involved in the evaluation of iron overload and prognosis in patients with MDS.
-
Key words:
- myelodysplastic syndrome /
- iron metabolism
-

-
表 1 45例MDS患者一般资料
项目 分类 例数 构成比/% 性别 男 27 60.0 女 18 40.0 年龄/岁 ≤60 19 42.2 >60 26 57.8 WHO分型 MDS-LB 32 71.1 MDS-IB1 6 12.3 MDS-IB2 3 6.7 MDS-SF3B1 4 8.9 IPSS-R积分/分 较低危(≤3.5) 27 60.0 较高危(>3.5) 18 40.0 表 2 MDS患者年龄分层与铁代谢指标检测结果及比较
M(P25,P75) 铁代谢指标 中青年组(n=19) 老年组(n=26) SI/(μmol/L) 21.56(16.13,36.04) 30.97(21.20,42.97) SF/(ng/mL) 815.50(159.60,2 421.80) 2 182.95(865.28,3 175.20)1) TF/(mg/dL) 2.33(1.80,3.08) 1.94(1.58,2.39) TIBC/(μmol/L) 51.53(36.43,60.36) 42.81(33.83,50.14) TS/% 45.38(30.92,62.53) 74.79(51.55,93.34) 与中青年组比较,1)P < 0.05。 表 3 MDS患者不同WHO分型的铁代谢指标检测结果比较
铁代谢指标 中青年组(n=19) 老年组(n=26) MDS-LB(n=16) MDS-IB1(n=3) MDS-LB(n=16) MDS-IB1(n=3) MDS-IB2(n=3) MDS-SF3B1(n=4) SI/(μmol/L) 27.65±17.40 13.13±8.24 34.12±19.11 33.40±8.44 30.99±19.66 27.59(21.15,74.27) SF/(ng/mL) 1 075.45(188.78,2 420.80) 1 146.97±1 278.59 2 405.75(674.48,3 239.40) 1 733.80±1 056.38 2 302.07±1 228.54 1 442.68±1 330.24 TF/(mg/dL) 2.60±0.73 1.66±0.261) 2.08(1.78,2.53) 2.16±0.56 2.20±0.84 1.55±0.43 TIBC/(μmol/L) 52.53±12.80 34.33±8.051) 42.83±11.70 43.84±8.40 43.59±13.06 37.45(29.00,140.93) TS/% 54.53±32.00 35.55±18.35 75.54(45.07,92.97) 78.85±22.79 66.51±35.51 68.62±20.50 与中青年组MDS-LB患者比较,1)P < 0.05。 表 4 MDS患者不同IPSS-R评分等级的铁代谢指标检测结果及比较
铁代谢指标 中青年组 老年组 较低危(n=12) 较高危(n=7) 较低危(n=15) 较高危(n=11) SI/(μmol/L) 23.88±17.18 27.88±17.77 29.97(19.25,50.06) 31.26(23.90,42.58) SF/(ng/mL) 1 319.98±1 184.96 1 138.37±1 015.88 1 296.00(500.80,3 143.10) 2 458.40(979.80,3 339.60) TF/(mg/dL) 2.46±0.72 2.43±0.87 1.96(1.59,2.32) 1.89(1.55,2.60)1) TIBC/(μmol/L) 50.50±12.55 48.23±16.68 42.94(32.85,50.36) 42.34(34.16,49.19) TS/% 49.44±32.72 55.11±28.94 67.06±28.62 72.92±23.01 与老年组较低危患者比较,1)P < 0.05。 表 5 MDS患者铁代谢指标与血常规的相关性分析
项目 中位数(四分位数) HGB/(g/L) r PLT/(×109/L) r ANC/(×1010/L) r SI/(μmol/L) 27.17(18.97,39.76) -0.112 -0.137 -0.172 SF/(ng/mL) 1 557.20(497.15,2 624.70) -0.4612) -0.106 0.006 TF/(mg/dL) 2.13(1.73,2.62) 72.00(58.50,83.50) 0.4592) 58.00(21.00,135.00) -0.178 1.54(0.81,3.50) -0.1781) TIBC/(μmol/L) 45.26(36.10,53.38) 0.3811) 0.026 -0.3521) TS/% 60.02(38.82,92.79) -0.2971) -0.020 -0.235 1)P < 0.05,2)P < 0.01。 表 6 MDS患者TF与其他铁代谢指标的相关性分析
项目 中位数(四分位数) r P TF/(mg/dL) 2.13(1.73,2.62) SI/(μmol/L) 27.17(18.97,39.76) 0.299 0.046 SF/(ng/mL) 1 557.20(497.15,2 624.70) -0.296 0.049 TIBC/(μmol/L) 45.26(36.10,53.38) -0.779 <0.001 TS/% 60.02(38.82,92.79) -0.062 0.688 -
[1] 中华医学会血液学分会, 吴德沛, 肖志坚, 等. 骨髓增生异常综合征中国诊断与治疗指南(2019年版)[J]. 中华血液学杂志, 2019, 40(2): 89-97.
[2] 汤如, 李承君, 吴燕明. 铁代谢参数判断骨髓增生异常综合征和再生障碍性贫血患者铁负荷过载的临床价值[J]. 临床和实验医学杂志, 2021, 20(11): 1181-1185. doi: 10.3969/j.issn.1671-4695.2021.11.017
[3] 周开慧. 铁代谢异常在骨髓增生异常综合征中的临床价值[J]. 国际检验医学杂志, 2016, 37(24): 3445-3448. doi: 10.3969/j.issn.1673-4130.2016.24.023
[4] Khoury JD, Solary E, Abla O, et al. The 5th edition of the World Health Organization classification of haematolymphoid tumours: myeloid and histiocytic/dendritic neoplasms[J]. Leukemia, 2022, 36(7): 1703-1719. doi: 10.1038/s41375-022-01613-1
[5] Greenberg PL, Tuechler H, Schanz J, et al. Revised international prognostic scoring system for myelodysplastic syndromes[J]. Blood, 2012, 120(12): 2454-2465. doi: 10.1182/blood-2012-03-420489
[6] 张惠琴. 铁超载在骨髓增生异常综合征中的研究进展[J]. 海南医学, 2019, 30(3): 384-387. doi: 10.3969/j.issn.1003-6350.2019.03.035
[7] 王文儒, 杜宇, 许勇钢, 等. 骨髓增生异常综合征与再生障碍性贫血的临床体征及淋巴亚群比较[J]. 临床血液学杂志, 2022, 35(10): 710-716. https://lcxy.whuhzzs.com/article/doi/10.13201/j.issn.1004-2806.2022.10.004
[8] 李章坤, 赖应昌, 李坤, 等. 地西他滨联合预激化疗对中老年MDS转化急性髓系白血病的近远期疗效及预后因素分析[J]. 中国实验血液学杂志, 2018, 26(6): 1713-1718. https://www.cnki.com.cn/Article/CJFDTOTAL-XYSY201806025.htm
[9] 姚灼新, 翟振民. 血清铁蛋白水平在MDS患者中危险度分层及预后评估的临床意义[J]. 中国处方药, 2019, 17(5): 129-130. https://www.cnki.com.cn/Article/CJFDTOTAL-ZGCF201905081.htm
[10] 聂琳. 骨髓增生异常综合征铁代谢的基础和临床研究[M]. 北京, 北京协和医学院中国医学科学院出版社, 2009: 17-18.
[11] 武霄云, 陈双, 赵芳, 等. 血清铁蛋白水平在初诊骨髓增生异常综合征患者的意义[J]. 中华临床医师杂志(电子版), 2013, 7(24): 11384-11387. doi: 10.3877/cma.j.issn.1674-0785.2013.24.068
[12] 李莉, 毕庆庆, 郑金菊, 等. 铁蛋白、叶酸和维生素B12检测在骨髓增生异常综合征诊疗中的价值[J]. 国际检验医学杂志, 2018, 39(18): 2256-2258. doi: 10.3969/j.issn.1673-4130.2018.18.015
[13] 刘娜, 张王芳, 张宝玺, 等. 铁调素与铁过载相关疾病关系的研究进展[J]. 广东医学, 2016, 37(13): 2048-2049. https://www.cnki.com.cn/Article/CJFDTOTAL-GAYX201613050.htm
[14] 雷宇, 曾清, 程纬民. β中间型地中海贫血患者血清铁调素、转化生长因子15和铁蛋白相关性研究[J]. 中国医药导报, 2020, 17(25): 100-103. https://www.cnki.com.cn/Article/CJFDTOTAL-YYCY202025026.htm
[15] 谢杨, 汪丹, 刘建会. 骨髓增生异常综合征贫血患者铁代谢、炎症指标与铁调素的关系及对病情转归的影响[J]. 临床误诊误治, 2022, 35(10): 58-62. https://www.cnki.com.cn/Article/CJFDTOTAL-LCWZ202210013.htm
[16] 顾树程, 常春康. 铁过载的调控与其在骨髓增生异常综合征中的研究进展[J]. 诊断学理论与实践, 2012, 11(4): 428-432. https://www.cnki.com.cn/Article/CJFDTOTAL-ZDLS201204030.htm
-




 下载:
下载: